A 56-year-old Hispanic male presented for an updated spectacle Rx. He reported a 10-year history of reduced visual acuity in his right eye; however, his left eye was unaffected. When questioned about the cause of his reduced acuity, he said that he wasn’t sure, but remembered seeing an eye doctor several times when his vision started to decline. His medical history was unremarkable, and he reported taking no medications.

His best-corrected visual acuity measured 20/400 O.D. and 20/20 O.S. Extraocular motility testing was normal. Confrontation visual fields were full to careful finger counting O.U. and his pupils were equally round and reactive, with no afferent defect. Amsler grid testing showed a dense central scotoma in his right eye. The anterior segment examination was unremarkable O.U.
On dilated fundus exam, the vitreous was clear in both eyes. He had small cups with good rim coloration and perfusion in both eyes. Examination of the right macula showed nonspecific retinal pigment epithelium (RPE) mottling (figure 1).
There was no obvious subretinal fluid present, and the peripheral retinal exam was unremarkable. The left eye was normal. We performed a spectral-domain OCT (SD-OCT) scan (figure 2) as well as fundus autoflorescence (FAF) (figure 3).
Take the Retina Quiz
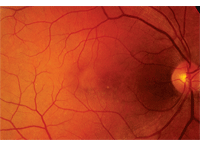
1. Fundus photograph of our patient’s right eye shows unusual changes in his macula. What do these changes represent?
1. What does the SD-OCT show?
a. Occult neurosensory detachment.
b. Occult choroidal neovascularization (CNV).
c. Polypoidal choroidal lesions.
d. Loss of the photoreceptor integrity line (PIL).
2. What does the FAF reveal?
a. Occult CNV.
b. Nonspecific RPE atrophy.
c. Trough demarcation line.
d. Loss of the RPE secondary to lipofuscin accumulation.
3. What is the most likely diagnosis?
a. Stargardt’s macular dystrophy (SMD).
b. Resolved idiopathic central serous choroidopathy (ICSC).

2. A horizontal slice through the macula of our patient’s right eye on SD-OCT.
c. Occult CNV.
d. Polypoidal choroidal vasculopathy.
4. How should this patient be managed?
a. Observation along with protective eye wear.
b. Avastin (bevacizumab, Genentech) or Lucentis (ranibizumab, Genentech).
c. Photodynamic therapy (PDT).
d. Laser therapy.
For answers, see below.
Discussion
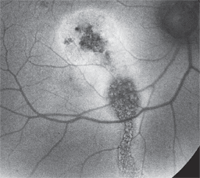
3. The fundus autoflorescence results of our patient’s right macula. What do you notice?
Based on the fundus exam of our patient’s right eye, it was difficult to explain why he could see no better than 20/400. Indeed, it did not appear to be a 20/400 macula; there was no obvious subretinal fluid nor any macular edema that could be appreciated based on the clinical exam. However, we noted some nonspecific RPE alterations, including a circular, yellow-appearing change located temporal to the fovea. This presentation also looked flat and didn’t fit into any recognizable clinical diagnosis. Without any clear answers, we performed an
SD-OCT and FAF. The diagnostic tests revealed some surprising findings.
The SD-OCT provided the first real clue as to what was affecting this patient. First, we ruled out the pertinent negatives; we saw no subretinal fluid, retinal detachments, CME or other obvious changes. In fact, at first glance, the SD-OCT looked quite normal.
However, on closer inspection, it appears anything but normal. Just above (or anterior to) the RPE, there is a darker white line that represents the junction of the photoreceptor inner and outer segments. This line is called the photoreceptor integrity line, and it is incomplete in our patient’s right eye. Starting on either edge of the SD-OCT scan, the PIL is easily located and can be followed to just outside the fovea. Then, it stops. This explains why our patient sees 20/400 O.D.––he has no photoreceptors in his macula. But why?
The FAF provides the final clue. FAF is a non-invasive photographic method of documenting pathological retinal changes. More specifically, it uses the fluorescent properties of lipofuscin to study retinal disease in vivo. It is most commonly used in patients with AMD where lopofuscin accumulation is a marker for retinal toxicity and disease progression. Other diseases may also show hypo- or hyperfluorescent changes, depending on the retinal condition.
In our patient, the FAF image is quite striking. There is a central zone of RPE atrophy, which corresponds to the area seen on the SD-OCT where the PIL was missing. Additionally, there is a linear zone of RPE atrophy that extends posteriorly to the inferior retina. This represents an old fluid trough line. We can postulate that our patient had a chronic serous detachment involving his macula. Then, over time, the fluid extended inferiorly. The fluid eventually dried up, but not before it caused scarring and atrophy of his macula, as well as created the trough line that can be seen on the FAF. Remarkably, this finding is virtually invisible on the clinical exam.
So what caused the fluid and macula scarring? More than likely, these findings were caused by ICSC. Clinically, the hallmark of ICSC is a neurosensory retinal detachment that usually involves the macula.1 Typically, it affects otherwise healthy patients between 20 and 45 years of age. Also, men are five to 10 times more likely to develop ICSC than women. The condition usually is associated with emotional stress, and is frequently seen in patients who exhibit achievement-oriented, “type A” personalities.1 The disease is usually self-limiting with an excellent visual prognosis. However, not everybody responds with a successful outcome, as was the case with our patient. Indeed, recurrences develop in one-third to one half of patients with ICSC (usually within one year), and 10% of patients experience three or more episodes.
At this point, we could not do much for our patient other than recommend protective eye wear for his good eye. The damage from the disease has been done, and unfortunately, nothing can restore the photoreceptors. We explained the findings and asked him to return for annual follow-ups.
Retina Quiz Answers: 1) d; 2) c; 3) b; 4) a.
1. Gass JD. Stereoscopic atlas of macular disease: diagnosis and treatment, 4th ed. St. Louis: Mosby; 1997:52-70.

