 A 50-year-old white male presented with blurred vision in his left eye that persisted for two weeks. He said he woke up one morning and noticed that something was just not right with his vision. When the patient covered his right eye, he noted blurry vision in the left eye.
A 50-year-old white male presented with blurred vision in his left eye that persisted for two weeks. He said he woke up one morning and noticed that something was just not right with his vision. When the patient covered his right eye, he noted blurry vision in the left eye.
He said that he never experienced any eye problems in the past. He began wearing glasses when he was in college, but has always had good corrected visual acuity.
The patients medical history is significant for systemic hypertension, for which he takes Norvasc (amlodipine besylate, Pfizer).
On examination, his best-corrected visual acuity measured 20/20 O.D. and 20/60 O.S. Confrontation visual fields were full to careful finger counting O.U., but with some difficulty superiorly O.S. Motility testing was normal. His pupils were equally round and reactive, with a trace left afferent pupillary defect.
The anterior segment exam was normal O.U. His intraocular pressure measured 17mm Hg O.U.
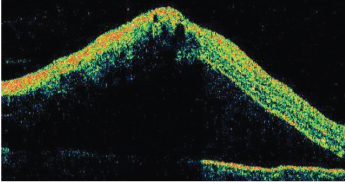
1. Optical coherence tomography of the macula O.S. What finding does it show?
Optical coherence tomography (OCT) was ordered O.S. (figure 1). On dilated fundus examination, the right eye was completely normal; however, the left eye showed obvious changes (figure 2).
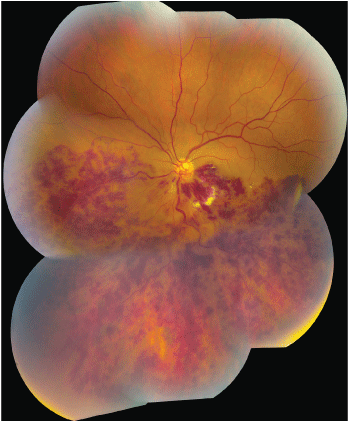
2. A wide-field fundus photo of the left eye shows an obvious retinal pathology.
Take the Retina Quiz
1. What is the correct diagnosis in this case?
a. Central retinal vein occlusion (CRVO).
b. Hemiretinal vein occlusion (HRVO).
c. Branch retinal vein occlusion (BRVO).
d. Cytomegalovirus (CMV) retinitis.
2. What is the most likely cause for the patients reduced visual acuity?
a. Cystoid macular edema (CME).
b. Ischemia.
c. Retinal hemorrhage.
d. Combination of CME and subretinal fluid.
3. What is he at greatest risk for developing?
a. Iris and angle neovascularization.
b. Retinal neovascularization.
c. Vitreous hemorrhage.
d. All of the above.
4. How should this patient be managed initially?
a. Observation.
b. Laser photocoagulation.
c. Intravitreal Kenalog injection (triamcinolone, Bristol-Myers Squibb).
d. Pars plana vitrectomy.
5. Which management strategy offers the safest and best opportunity for improving the patients vision?
a. Observation.
b. Laser photocoagulation.
c. Intravitreal Kenalog injection.
d. Intravitreal Avastin injection (bevacizumab, Genentech).
For answers, see below.
Discussion
Our patient has a hemiretinal vein occlusion that involves the inferior half of his retina O.S. He also has both cystoid macular edema and subretinal fluid under the macula, which contributed to his reduced visual acuity. (This is very apparent on the OCT.)
Retinal vein occlusions affect the venous blood supply of the retina. They present as a central retinal vein occlusion or as a branch retinal vein occlusion, in which only a quadrant of one of the branches of the central retinal vein is affected. HRVOs are variants of CRVOs, but the clinical course can follow either that of a CRVO or a BRVO, depending on its origin.1
Other than diabetic retinopathy, CRVO is the most common vision-threatening vascular disorder in American patients past age 50.1 About 43% of all retinal vein occlusions are CRVOs.1 The etiology of CRVO can be attributed to atherosclerosis within the adjacent central retinal artery. This can result in increased blood viscosity, damage to vascular endothelial cells or abnormal platelet formation.
The site of the occlusion in CRVO is usually at or posterior to the lamina cribosa before the central retinal vein bifurcates into its main branches. Typically, the more posterior the occlusion occurs within the optic nerve, the more severe and ischemic the CRVO will be.
HRVO occurs when one of the major branches of the central retinal vein becomes occluded at or near the anterior portion of the optic disc. HRVO can also occur when a dual-trunked central retinal vein becomes occluded in the anterior part of the optic nerve. This dual trunk is the result of a congenital variant in one of the central retinal veins that persists in the anterior part of the optic nerve. This anomaly occurs in 20% of the population.2,3
It is difficult to determine the natural history of an HRVO based on the clinical exam alone, and most studies have had insufficient HRVO cases to compare the risk factors for the different types of RVOs.
It is important to determine the risk of secondary complications, such as iris or angle neovascularization, that can lead to neovascular glaucoma. Neovascular glaucoma is more likely to occur with a CRVO. Patients with ischemic BRVO are more likely to develop vitreous hemorrhage from retinal neovascularization. Follow-up for all RVOs is predicated on the risk of developing these complications.
The treatment that is most effective depends on the nature of the RVO. BRVOs tend to have a better visual outcome with laser photocoagulation than CRVOs.
However, the Central Vein Occlusion Study Group did not find any significant difference in visual acuity between laser-treated and untreated eyes at any time during follow-up.4 Also, the prognosis of CRVOs and HRVOs is very poor without treatment. Studies have shown an improvement of two or more Snellen lines in only 18% of eyes with untreated CRVO over 36 months and 21% of eyes with untreated HRVO over 14.4 months.4,5
Intravitreal Kenalog has demonstrated varying results when used to treat refractory macular edema in patients with retinal vein occlusions.5,6 Unfortunately, the risk of glaucoma and cataracts has limited its use, especially with the recent availability of intravitreal Avastin.
Avastin is an anti-VEGF drug that inhibits pathologic neovascularization and reduces capillary permeability. So far, it has exhibited great promise in reducing refractory macular edema due to several causes, including retinal vein occlusions.
Retinal specialists have debated about what should be the standard of care for treating retinal vein occlusions. There is no easy answer for BRVO considering that laser treatment has been shown to improve vision vs. observation alone. With CRVO, there is no effective treatment for macular edema, so investigators have been quick to use off-label treatments, such as Kenalog or anti-VEGF drugs.
So, does Avastin represent the Holy Grail for the treatment of retinal vein occlusions? At this point, it is too early to tell. There are several ongoing clinical trials that may answer this question.
We explained the diagnosis of HRVO to our patient along with his treatment options, including observation and intravitreal Avastin injection O.S. The patient elected for the Avastin injection. One month later, he returned with reduced macular edema, and visual acuity improved to 20/30 O.S.
A second injection was administered at his one-month follow-up visit, followed by a third injection one month later. Our patients vision ultimately stabilized at 20/30 O.S., with complete resolution of his macular edema.
One question remains, however: Would he have had the same outcome from observation alone? Not likely, but that question highlights why clinical trials are necessary to scientifically determine if one treatment is better than another, or if a treatment would be even better than the natural course of the disease. Hopefully, we will learn the answer to that question in the future.
Retina Quiz Answers: 1) b; 2) d; 3) d; 4) a; 5) d
1. Hayreh SS. Classification of central retinal vein occlusion. Ophthalmology 1983 May;90(5):458-74.
2. Chopdar A. Dual trunk central retinal vein incidence in clinical practice. Arch Ophthalmol 1984 Jan;102(1):85-7.
3. Sperduto RD, Hiller R, Chew E, et al. Risk factors for hemiretinal vein occlusion: comparison with risk factors for central and branch retinal vein occlusion. The eye disease case-control study. Ophthalmology 1998 May;105(5):765-71.
4. The Central Vein Occlusion Study Group M report. Evaluation of grid pattern photocoagulation for macular edema in central vein occlusion. Ophthalmology 1995 Oct;102(10):1425-33.
5. Cekic O, Chang S, Tsent JJ, et al. Intravitreal triamcinolone treatment for macular edema associated with central retinal vein occlusion and hemiretinal vein occlusion. Retina 2005 Oct-Nov;25(7):846-50.
6. Ip MS, Gottlieb JL, Kahana A. Intravitreal triamcinolone for the treatment of macular edema associated with central retinal vein occlusion. Arch Ophthalmol 2004 Aug;122(8):1131-6.

