 |
Q:
I have a patient who has been unable to get eye care at the nearest Veterans Affairs (VA) Medical Center in a timely manner. What are his options?
A 65-year-old male patient with a family history of glaucoma was “examined remotely” through the Technology-based Eye Care Services (TECS) program in the rural mountains of Georgia. His IOPs were measured at 28mm Hg OD and 29mm Hg OS. His optic nerve photographs revealed rim tissue thinning, with the OCT showing corresponding thinning of the nerve fiber layer. He was diagnosed with glaucoma by the remote optometrist reviewing the patient’s findings and started on latanoprost OU qhs.
The patient was then referred for an in-person gonioscopy exam at the main VA medical center eye clinic but will come back to the TECS site near his home for further testing, including a VF test and monitoring in the teleglaucoma program. “This is one example of thousands that has already prevented blindness through telemedicine,” says Trennda Rittenbach, OD, reader for the Atlanta VA TECS program. “This patient might not have sought out care because the closest VA Medical Center was over 2.5 hours away in Atlanta.” Dr. Rittenbach and her team were able to get him started on medication immediately, all from the Seattle area.
 |
|
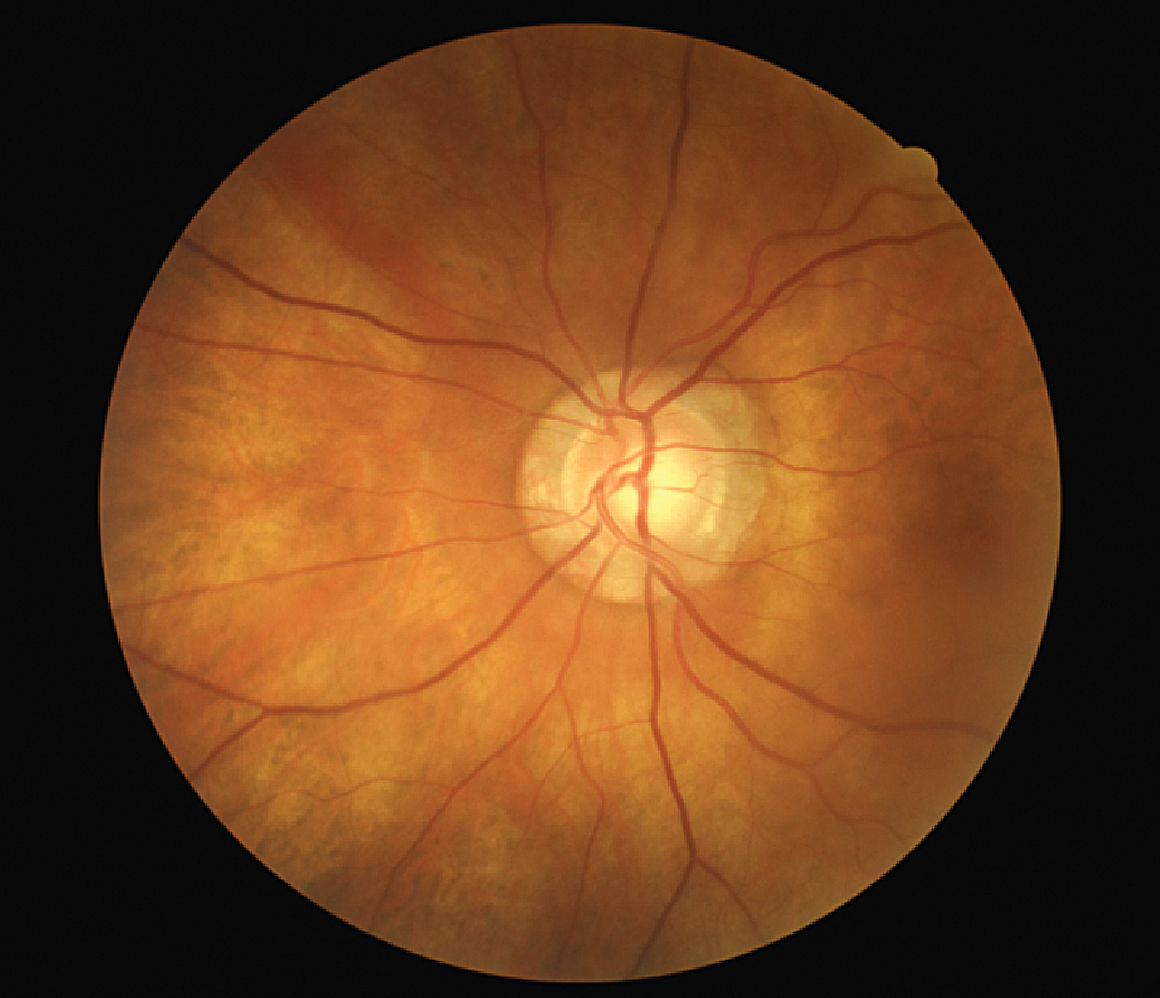
Optic nerve with neuroretinal rim loss could be diagnosed in a VA telehealth setting. Photo: Kimberly Simmons, COT. Click image to enlarge. |
A Growing Need
The US has a very large rural population that has difficulty accessing our healthcare system. The projected number of adults with a diagnosis of diabetes will increase from 22.3 million in 2014 to 39.7 million in 2030, and to 60.6 million in 2060.1 By 2020, it is expected that approximately 76 million people will suffer from glaucoma, with that number estimated to reach 111.8 million by 2040.2 The number of people with AMD was estimated to be 196 million in 2020 and predicted to be 288 million in 2040.3
“These are ocular diseases that can be diagnosed and often times managed and treated in the telemedicine setting,” Dr. Rittenbach says.
In 2015, the VA launched the TECS program to bring specialty eye care to underserved veterans who have limited access to eye and vision exams. Quality care measures are in place that monitor the initiative, and so far those evaluations have proven that vision care and medical eye care can be more conveniently accessed, and that patients are very happy with the process.
The Way It Works
Trained technicians at community-based outpatient clinics gather information such as visual acuity, ancillary testing and fundus photography. Doctors such as Dr. Rittenbach then come up with an assessment and treatment plan for the patient. Veterans who need follow-up care can see an eye care provider at a VA medical center or a local provider in the community.4 This newer tele-eye program goes beyond the diabetic eye screening to look for other common conditions.5
“We see a lot of ocular disease each and every day in this program and can treat and manage much of this via telemedicine,” says Dr. Rittenbach. “Some of the conditions regularly seen beside diabetic retinopathy include hypertensive retinopathy, retinal artery and vein occlusions, Hollenhorst plaques, AMD, glaucoma and cataracts.”
Dr. Rittenbach recently detected an eyelid lesion based on an external photo, and she suspected basal cell carcinoma and was able to get the patient in quickly for a biopsy which confirmed the diagnosis. “This type of patient may not have been seen in a timely manner due to their rural location, and the lesion could have grown in size and become invasive,” she says. “By using telemedicine, I was able to refer this patient promptly to a community specialist.” Dry eye, pinguecula, pterygium and cataracts are conditions also frequently seen in the TECS protocol using anterior segment photography.
“The private practitioner could model a similar telehealth clinic after the TECS program and be quite successful in improving access to either underserved populations or in urban areas where shortages of eyecare providers exist,” Dr. Rittenbach says. “Doctors in the private sector can use available exam lanes in their office—offices that don’t have a doctor staffed on a particular day,” she notes. “If we as a profession don’t embrace tele-optometry, other groups will and we will be left behind,” she warns.
Dr. Rittenbach and a panel of other experts recently discussed the new paradigm at the opening session at SECO’s 100th anniversary meeting titled, “Remote Exams: Virtual Reality or Virtual Certainty?”
Dr. Ajamian is board certified by the American Board of Optometry and serves as Center Director of Omni Eye Services of Atlanta. He is vice president of the Georgia State Board of Optometry and general CE chairman of SECO International. He has no financial interests to disclose.
1. Lin J, Thompson TJ, Cheng YJ, et al. Projection of the future diabetes burden in the United States through 2060. Popul Health Metr. 2018;16(1):9. 2. Allison K, Patel D, Alabi O. Epidemiology of glaucoma: the past, present, and predictions for the future. Cureus. 2020;12(11):e11686. 3. Jonas JB, Cheung CMG, Panda-Jonas S. Updates on the epidemiology of age-related macular degeneration. Asia Pac J Ophthalmol (Phila). 2017;6(6):493-7. 4. Technology-based Eye Care Services in the Department of Veterans Affairs. American Academy of Ophthalmology. 2018. www.aao.org/Assets/2f74bebb-f24d-4eaf-a9ac-3913e3b8ac5f/636589766568530000/va-tecs-program-issue-brief-2018-final-pdf?inline=1. Accessed January 27, 2023. 5. Maa AY, Patel S, Chasan JE, et al. Retrospective evaluation of a teleretinal screening program in detecting multiple nondiabetic eye diseases. Telemed J E Health. 2016;23(1):41-8. |

