 he glands of the endocrine system include the pituitary, thyroid, parathyroid, adrenal, gonads, pancreas, thymus and pineal glands.1 Disorders of the endocrine system can cause a hormone imbalance. This hormone imbalance (or endocrine disease/condition) can affect a person’s health in myriad ways.
he glands of the endocrine system include the pituitary, thyroid, parathyroid, adrenal, gonads, pancreas, thymus and pineal glands.1 Disorders of the endocrine system can cause a hormone imbalance. This hormone imbalance (or endocrine disease/condition) can affect a person’s health in myriad ways.
Neoplastic disease is a fairly common cause of pituitary disorders. Given the anatomic region of the pituitary gland, ocular manifestations are not uncommon.
Case Report
A 62-year-old female presented with complaints of fluctuating vision in each eye and peripheral vision loss that was consistent with bitemporal hemianopia. Onset was gradual over the past few months. She also reported frontal headaches for the past two to three months.
Her systemic history was remarkable for type 2 diabetes for the past eight years, hypertension for two months, hypercholesterolemia, and thyroid surgery 32 years ago. Her medications included glyburide, lisinopril, metformin and simvastatin. The patient is 5 feet, 3 inches tall and weighs 150lbs.
Best-corrected visual acuity was 20/30 O.D. and 20/40 O.S., with no improvement on pinhole. Pupils were equal in size with a mild relative afferent defect in the right eye.
Confrontation fields and Humphrey visual field testing revealed a dense bitemporal hemianopia. Intraocular pressure measured 15mm Hg O.D. and 17mm Hg O.S. Optic disc evaluation revealed bilateral diffuse pallor of the neuroretinal rim. No disc edema was visible.
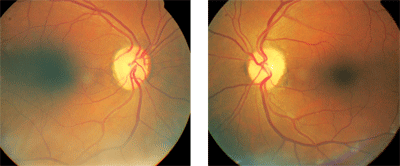
Optic disc evaluation of this
patient revealed diffuse pallor of the neuroretinal rims in both eyes.
Confrontation fields revealed bitemporal hemianopia, with the right eye
more affected than the left. A pituitary problem was suspected.
We diagnosed bitemporal hemianopia and bilateral optic nerve atrophy, both of unknown etiology.
Referral and Testing
At this point, we sent the patient for a neuro-ophthalmic consultation. In the neuro-ophthalmic exam, her acuity was unchanged and color vision was excellent. Pupils were isocoric, with a relative afferent pupillary defect in the right eye.
Confrontation fields revealed a bitemporal hemianopia, with the right eye more affected than the left. There was no evident proptosis. Ocular motility testing was normal. Cover testing at distance revealed an orthophoric horizontal and vertical deviation that was comitant in all positions of gaze.
Dilated fundus examination demonstrated optic discs with distinct margins and no edema. There was moderate cupping in both eyes. The neuroretinal rim demonstrated diffuse pallor of grade 2+ O.D. and grade 1+ O.S. The patient was alert and oriented to time, place and person. Neurologic examination revealed cranial nerve V and nerves VII to XII to be intact. Motor, sensory and coordination testing were unremarkable.
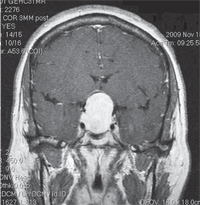
MRI of the brain revealed a very large mass in the suprasellar cistern, compressing the optic chiasm. It appeared to be an extension of the pituitary gland—likely a pituitary macroadenoma. Her lab test results were remarkable for a low luteinizing hormone (<0.2IU/L) and an elevated prolactin level (64.7ng/mL).
We promptly scheduled the patient to see a neurosurgeon for further evaluation and treatment. She subsequently underwent successful surgical removal of the tumor.
MRI of the brain (coronal view) revealed a large mass in the suprasellar cistern, compressing the optic chiasm.
Treatment and Management
In some pituitary tumor cases (prolactinomas), treatment consists of medical therapy with a dopamine agonist, such as Parlodel (bromocriptine mesylate, Novartis) or cabergoline. Normal pituitary lactotrophs are under the tonic inhibitory control of dopamine released by the hypothalamus and transmitted down the infundibulum to the anterior pituitary gland. Dopamine receptors, when stimulated, inhibit prolactin synthesis, which promotes shrinkage of the tumor.2
Although the response of prolactinomas to dopamine agents is variable, 70% to 100% of treated patients attain normalized prolactin levels, and 80% to 90% of treated patients experience a decrease in tumor size. Regrowth of a pituitary tumor can occur if medical therapy is discontinued too early.2
Standard therapy is surgical removal of the tumor, if it is not a prolactinoma. The most common surgical approach is called transsphenoidal adenectomy because the surgery is performed through the sphenoid sinus.3 If surgery is unable to remove the entire tumor, then complementary radiation treatment may be necessary to control the tumor and inhibit its growth.3-5
Radiosurgery (cyberknife) is a new option for treating pituitary adenoma. By focusing the radiation on only the tumor, this form of treatment minimizes the anatomical spread of radiation to the normal brain. Emerging data indicate that radiosurgery may be more effective than conventional radiation in lowering abnormal hormone production, and does so over a shorter time.2,3
Radiosurgery, however, is not currently considered the standard treatment, especially for a pituitary adenoma. The risk of radiation is notable in this region in terms of pituitary and optic nerve function, as well as many other close structures.
The Optometrist’s Role
Eye care practitioners should be familiar with symptoms and signs of pituitary tumors. The same signs and symptoms that occur with an adenoma may also occur with other suprasellar mass lesions. If you suspect such a lesion, appropriate ophthalmic workup and neuro-imaging are essential.
If a pituitary tumor is suspected or found, the optometrist or neurosurgeon should order lab testing of the pituitary hormones. This needs to be done before the patient sees the surgeon to determine the mode of therapy; a prolactinoma, for instance, is treated differently than other pituitary tumors.2 Tests include measuring levels of thyroid-stimulating hormone (TSH), follicle-stimulating hormone (FSH), luteinizing hormone (LH), adrenocorticotropic hormone (ACTH), prolactin, growth hormone (GH) and insulin-like growth factor 1 (IGF-1).
Once the condition is diagnosed and characterized, comanagement with a neurosurgeon is imperative. The other key member of the surgical team is an ear/nose/throat (ENT) specialist. ENT evaluation and follow-up is essential, especially for important complications, such as a cerebrospinal fluid leak. Other members of the health care team for these patients include an endocrinologist, neuroradiologist and neurophthalmologist.2,4,5
Patients with pituitary tumors should be followed closely with visual field testing and periodic optic nerve evaluation. If a patient’s visual field defect worsens, consider regrowth of the tumor, pituitary apoplexy, or chiasmal herniation into an empty sella (empty sella syndrome).5
Neuro-ophthalmic rehabilitation is a growing subspecialty in optometry. This involves using optical and non-optical methods of enhancing a patient’s visual efficiency and visual field. Consider this post-treatment option for patients with pituitary tumors.
Pituitary tumors may present as an expanding sellar mass and result in visual field defects and/or headaches. The optometrist is in a unique position to identify such masses so that timely treatment can be administered. The optometrist may also implement rehabilitative care to improve visual and overall function.
Thanks to Kelly Malloy, O.D., for her expert consultation and contribution to this column.
1. Rosdahl CB. The Endocrine System. In: Textbook of Basic Nursing. 6th ed. Philadelphia: J.B. Lippincott; 1995:196-205.
2. Hendrick AM, Kahook MY, Daoud YJ, Hazin R. Ophthalmic manifestations of endocrine disorders: approaches and medical management. Curr Opin Ophthalmol. 2009 Nov;20(6):495-503.
3. Sheehan JP, Niranjan A, Sheehan JM, et al. Stereotactic radiosurgery for pituitary adenomas: an intermediate review of its safety, efficacy, and role in the neurosurgical treatment armamentarium. J Neurosurg. 2005 Apr;102(4):678-91.
4. Wormington CM. Pituitary adenoma: diagnosis and management. J Am Optom Assoc. 1989 Dec;60(12):929-35.
5. Dorotheo EU, Tang RA, Bahrani HM, et al. Her vision was tied down. Surv Ophthalmol. 2005 Nov-Dec;50(6):588-97.

