 |
I am astounded by the new technologies that help us deliver higher levels of patient care, whether it’s a retinal analyzer that allows me to look at numerous layers of the retina and choroid with a single scan, a fundus image where facial recognition software identifies typical retinal pathologies instead of faces, or the ability to have an autofluorescent image of the retina without using IV sodium fluorescein.
Future Reimbursement
These technological advancements have changed the way we describe the testing that is performed on a daily basis within ophthalmological and optometric practices, and in many respects the CPT coding definitions and rules can be somewhat behind the technology. We now have a single instrument that can provide a high-resolution fundus photograph (92250), an OCT of the optic nerve (92133) and retina (92134) and an autofluorescent image of the retina (92250).
It wouldn’t surprise me if, in the future, all retinal imaging is grouped together and a new reimbursement paradigm is applied, allowing practitioners to perform any test at the frequency they believe would deliver the best outcome for the patient at a fixed cost per patient per year.
It’s possible a carrier could propose a fixed global reimbursement per patient for all retinal images. It would most likely reduce the amount of testing performed—and it would certainly contain costs from a carrier’s perspective.
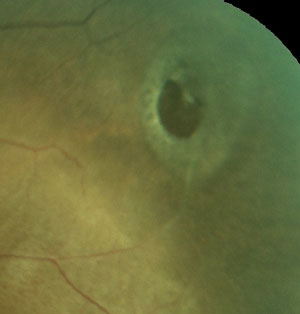 | |
| Fundus imaging reveals a horseshoe tear. Image: Mohammad Rafieetary, OD. |
Whether this would be a good policy or not is immaterial. The powers driving health care reform have a mandate to deliver high quality care in an efficient manner and at the lowest cost. Reducing the use of health care is also a mandate, and creating a coding and reimbursement paradigm that reflects the current technological advances and anticipates future ones is a priority of the American Medical Association and the Centers for Medicare & Medicaid Services.
Current Coding
So how does this affect us today? It is important to know the current definitions of the CPT for retinal imaging. In December 2014, the CPT refined its definition of autofluorescent imaging of the retina performed without sodium fluorescein. Prior to this ruling, CPT code 92499, “unlisted ophthalmic procedure,” was the typical code used to describe autofluorescent imaging of the retina. But after the December ruling, the CPT now stipulates that the appropriate code is 92250, “fundus photography.”
The implications of this decision affect your practice, considering that today, in many jurisdictions, a practitioner is allowed a limited number of fundus photographs (92250) in a given year on a per patient basis. So if you’ve already performed one and want to take another, you may not be allowed to and have a carrier pay for it. Special ophthalmic tests cannot be done prognostically—you must establish medical necessity prior to ordering the test. Yet, much of the technology on the market today allows practitioners to make better diagnoses earlier in the disease life cycle. It’s a conundrum for sure, but one that a global annual allowance for retinal imaging would solve.
How we provide care and are reimbursed for it is under intense scrutiny with the mandate to do it better, faster and cheaper. Advancing technologies that offer multiple retinal imaging methods contained within a single instrument can certainly help us care for our patients better, faster and, in the future, most likely at a lower reimbursement. This same paradigm has been applied to almost every sector of the business world, and it’s now being applied to health care. It’s all about “big data” and data analysis, and we are about to get our numbers crunched.
Send questions and comments to ROcodingconnection@gmail.com.
