 |
Q:
One of my patients presented with a swollen left eye with lid edema. Where do I go from here?
A:
While there are many conditions in the differential, first ask if the patient has any prior history of trauma and has noticed any decrease in vision, pain, fever or restricted eye movements, says Jessica Schiffbauer, OD, of Virginia Eye Consultants in Norfolk, VA. “Also ask if the patient has been exposed to any chemicals or foreign materials in order to rule out an allergic reaction.”
Dr. Schiffbauer recently saw a 46-year-old African American female who reported that the left side of her face was swollen. She was seen in the ER the night before, where she was diagnosed with an abrasion. The patient complained of decreased vision and pain. Exam showed 4+ upper lid edema, 4+ chemosis of the conjunctiva and a 4mm corneal abrasion temporally. “However, on physical exam, it appeared that the left eye was proptotic, and the patient experienced significant motility restriction in all positions of gaze,” she says.
The patient was sent to the ER with an order for a CT scan of the orbits. The CT revealed a diagnosis of orbital cellulitis. The patient was admitted to the hospital and given antibiotics. This hospital did not have ophthalmology on staff, so the patient was transferred to a different location. A CT performed at the second hospital showed no signs of cellulitis but rather a significant preseptal edema. At this point, the patient was starting to develop a corneal ulcer as well.
CT-A to the Rescue
The hospital wanted to discharge the patient back for treatment of the corneal ulcer; however, the amount of lid edema and chemosis along with the proptosis was inconsistent with the corneal ulcer alone, according to Dr. Schiffbauer. As the swelling started to develop on the opposite side of the patient’s face, Dr. Schiffbauer dug deeper into the case. Her team ordered CT-angiography (CT-A). “While not a commonly used test, CT-A contrast media is used to image blood vessels and tissue in a given area, allowing for detection of arterial and venous diseases,” Dr. Schiffbauer notes.
The CT-A results showed dilated veins in the right neck involving the external jugular venous system. The patient had severe bilateral constriction of the outflow veins from her face, backing up the blood trying to get out of her face, which then flowed through the conjunctiva and drained out of the back of the orbit into the intracranial venous sinus system. “These same issues can be seen with dialysis patients,” notes Dr. Schiffbauer.
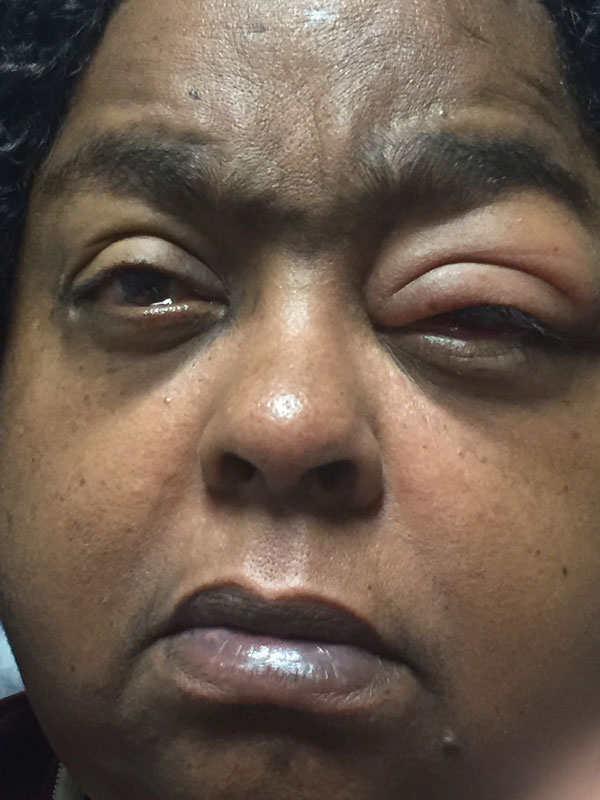 |
| The patient’s vision, 20/200 best corrected, had dropped from 20/30 recorded a week prior. |
Follow Up
A vascular surgeon performed a balloon angioplasty to help open up the blood vessels, eliminate the occlusion that was affecting blood flow and dramatically reduce the lid edema, chemosis and swelling. The patient’s vision was now 20/40 with no extraocular motility restrictions, and the proptosis had resolved. The patient reported that her pain was gone.
All findings must be considered in every patient. Doing a good external exam and confrontation field, motility and pupil testing on every patient, even emergency add-on red eyes, cannot be overemphasized. It would be easy to assume that the lid swelling was caused by the ulcer, but that would have been disastrous for the patient, Dr Schiffbauer cautions. Look at every finding and, if it doesn’t make sense, get some help, she adds. In this case, motility, proptosis and the amount of swelling didn’t make sense and led to a deeper and more curious diagnosis.

