 History
History
A 43-year-old white man required a bedside consultation for what the intensive care floor attending referred to as “recalcitrant bacterial conjunctivitis OD.” The man suffered from multi-organ disease and was intubated, rendering him incapable of providing additional historical information.
His medical chart indicated that he had hypertension, diabetes, chronic obstructive pulmonary disease and kidney disease. He reported no known allergies.
Diagnostic Data
His pupils were equally round, with no evidence of afferent defect. Extraocular muscle movements were full and unrestricted via doll’s eyes (oculocephalic) reflex testing.
His intraocular pressure measured 16mm Hg OS. Slit lamp examination of the patient’s left eye revealed normal and healthy anterior segment structures.
Dilated fundus examination uncovered normal posterior poles with healthy and intact peripheries OS. The accompanying photograph reveals a gross exterior view of his right eye.
Your Diagnosis
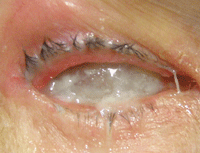
Exterior view of our 43-year-old patient’s right eye. What is your diagnosis?
How would you approach this case? Does the patient require any additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Discussion
The diagnosis in this issue is bacterial conjunctivitis associated with a poorly sanitized ocular spacer. The spacer was removed and disinfected, and the eye socket was properly lavaged and debrided.
We initiated dosing with a combination of ciprofloxacin ophthalmic ointment BID and bacitracin ophthalmic ointment BID, as well as daily lid and socket hygiene.
- Enucleation is the removal of the globe from the orbital area.
- Evisceration is the removal of ocular contents, allowing the sclera and its muscular attachments to remain.
- Exenteration is the most radical intervention for an anophthalmic patient, and involves removal of the globe and portions of the adnexa and/or orbit.1,2
Enucleation often is associated with intraoperative and postoperative complications; however, it remains the procedure of choice in patients who require histopathologic examination.1 Cases that involve intraocular neoplasm or ocular trauma with visual loss often are treated with this procedure.1
Technically, evisceration is a simpler and faster operation than enucleation.1 Further, because the sclera remains connected to the extraocular muscles, the procedure frequently yields a better cosmetic result than that exhibited following enucleation.1 It is indicated in patients with longstanding history of blind, unsightly or painful eyes, and in select instances of ocular trauma following a discussion of the risks associated with sympathetic ophthalmia.1
It is contraindicated in patients with possible intraocular malignancy.1 In appropriate cases, a cosmetic shell can be implanted to improve orbital volume and increase cosmesis.1

Cleaned and disinfected temporary shell following explanation.
A variety of materials may be used for orbital implantation in an anophthalmic socket.3 Autogenous grafts have been used successfully to treat superior sulcus deformities, extruding implants and incidences where the socket begins to contract. The major advantage of autogenous material is that it is minimally inflammatory and inherently compatible with the host.3
Regardless whether the spacer is autogenous, evidence suggests that anterior exposure can allow bacterial colonization and the development of a heavy inflammatory infiltrate in patients who are immunodeficient.4 Poor tissue ingrowth may limit the penetration of topical or systemic antibiotic therapy. In such instances, explanation may be required.4
The follow-up photograph reveals a cleaned and disinfected temporary shell following explanation. Because the shell was not sutured in place, it was removed at the patient’s bedside and kept out over the duration of therapy.
1. Dortzbach RK, Woog JJ. Choice of procedure. Enucleation, evisceration, or prosthetic fitting over globes. Ophthalmology. 1985 Sept;92(9):1249-55.
2. Rubin PA. Enucleation, evisceration, and exenteration. Curr Opin Ophthalmol. 1993 Nov;4(5):39-48.
3. Petrelli RL. Use of autogenous materials in reconstructing the anophthalmic socket. Adv Ophthalmic Plast Reconstr Surg. 1990;8:153-69.
4. Chuo JY, Dolman PJ, Ng TL et al. Clinical and histopathologic review of 18 explanted porous polyethylene orbital implants. Ophthalmology. 2009 Feb;116(2):349-54.

