Q: Of the few infections that occur following LASIK, why is there such a high prevalence of mycobacterium infections, while other infections are exceedingly rare? Most practitioners never see a single case.
A: Mycobacterium is a genus of Gram-positive, mostly slow-growing, ubiquitous microorganism that contains 50 species, including M. tuberculosis and M. leprae, the causal agents of tuberculosis and leprosy, respectively.1,2 Members of the other species are termed atypical, anonymous, non-tuberculosis and mycobacteria other than tuberculosis.2 The atypical strainsM. chelonae and M. fortuitumare most commonly implicated in bacterial keratitis.3
So, why do LASIK patients have such a high prevalence of mycobacterial infections?
The organisms may be introduced at the time of surgery, postoperatively or through exposure in the operating room environment, says Jay S. Pepose, M.D., Ph.D., of St. Louis. So, for example, if a bottle of balanced salt solution is chilled or rinsed with cold tap water, this could be a source of contamination. Also, mycobacterium can enter through air conditioning ducts. Finally, the gentian violet marking solution used during the procedure may be a source.4
Mycobacterium is a ubiquitous organism, but it rarely implants, adds ophthalmologist Peter S. Hersh, of Teaneck, N.J. During LASIK, however, there is a breakdown of barriers to infection, mostly because of the subclinical trauma to the epithelium and also because the flap-bed interface leaves a potential space for the organism to embed. That potential space can leave the patient with an anatomic circumstance that may induce infection with mycobacterium.
Q: What course of action should I take if I suspect mycobacterial infection?
A: First, make sure it is mycobacterium. Diffuse lamellar keratitis (DLK) can masquerade as mycobacterium and a fungal infection. Therefore, it is crucial you make a differential diagnosis so you can provide the patient with the correct medication, Dr. Pepose says. Patients who have a mycobacteria infection and are misdiagnosed as having DLK often experience necrosis and flap melt, which necessitates either partial or complete amputation of the flap.
Suspect a mycobacterial infection in a patient who has intrastromal inflammation and a focal infiltrate for more than a month after undergoing LASIK but no history of eye trauma since undergoing the procedure, says ophthalmologist Eric D. Donnenfeld, of Rockville Centre, N.Y.
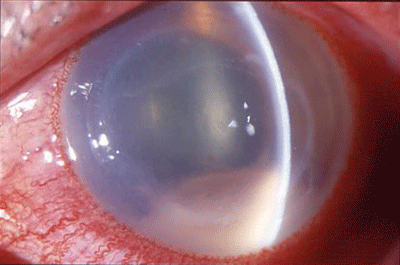
If the infiltrate appears dense and white, but you dont see surrounding inflammatory speckling, which is indicative of DLK, you are most likely dealing with a mycobacterium infection, Dr. Pepose says. Mycobacterium appears as a dense focal lesion.
Suspect a mycobacterial infection in a patient who has intrastromal inflammation and a focal infiltrate for more than a month after undergoing LASIK but no history of eye trauma since undergoing the procedure, says ophthalmologist Eric D. Donnenfeld, of Rockville Centre, N.Y.
If the infiltrate appears dense and white, but you dont see surrounding inflammatory speckling, which is indicative of DLK, you are most likely dealing with a mycobacterium infection, Dr. Pepose says. Mycobacterium appears as a dense focal lesion.
|
|
|
Mycobacterium appears as a dense focal lesion. |
Other signs of mycobacterial infection: pain, epithelial defect over and above the infiltrate, and an infiltrate that encompasses more than just the interface, such as the flap and the corneal bed. DLK generally is not painful and generally has a sand-like diffuse appearance that does not typically affect the flap or the corneal bed, Dr. Hersh says.
Clinical observation is important, but do not treat patients until you have a definitive diagnosis from culturing. Organisms may be most present underneath the flap, so refer the patient back to the ophthalmologist to lift the flap and then scrape the cornea, Dr. Hersh says. Then, send the culture to a lab that has Lowenstein-Jensen culture media in addition to blood chocolate agar and Sabourauds agar, as these media are made to identify mycobacteria.
If the culture comes back positive for mycobacteria, prescribe a combination therapy of fortified amikacin (3.3%), clarithromycin 1% and a fourth-generation fluorquinolone.5 (For the treatment of DLK, see Cornea + Contact Lens Q + A: DLK More Likely than Infection, November 15, 2005.)
A lot of these organisms have variable resistance to different antibiotics, and the fourth-generation fluoroquinolones are not as effective as they once were, Dr. Pepose says. For these reasons, I think its a mistake to pick only one antibiotic to treat mycobacteria and hope for the best.
Each doctor we talked with recommends a slightly different method of treatment using these medications.
Dr. Peposes method: Have the patient switch between fortified amikacin and clarithromycin 1% every half hour. After instilling each drug, have the patient wait five minutes before instilling a fourth-generation fluoroquinolone so as not to dilute the other medication. At night, have the patient wake every hour and alternate between the amikacin and the clarithromycin 1%, then complement these drugs with a fourth-generation fluoroquinolone. Taper this regimen if the patient has a positive response to it, but be aware that he or she could be on this therapy for months, Dr. Pepose says.
Dr. Hersh, however, advises that you start this patient on fortified amikacin and clarithromycin every hour, alternating with a fourth-generation fluoroquinolone every hour (i.e., drops every half hour). Sometimes these may be supplemented with oral clarithromycin. Youre generally starting early on medications and tapering over the course of the month based on clinical response, he says. You are probably looking at a three-month course in many of these patients. Each patient will have a different degree of response and mycobacteria activity.
Dr. Donnenfelds advice: Start this patient on an alternating regimen of fortified amikacin and gatifloxacin every half hour during the day and night for one week. If the patient does not respond, add clarithromycin 1% to the mix, then taper. Therapy for this type of bacteria is usually two to three months.
The key to beating a mycobacterial infection is speed. You cant wait a week and observe the patient, Dr. Pepose says. If your suspicion is raised, immediately refer the patient for culturing so you can get him or her on the correct medication and ensure [the patients] vision and long-term outcome.
1. Dorlands Illustrated Medical Dictionary. 28th ed. Philadelphia: W.B. Saunders, 1994:1086.
2. Lalitha P, Rathinam SR, Srinivasan M. Ocular infections due to non-tuberculosis mycobacteria. Indian J Med Microbiol 2004;22(4):231-37.
3. Abshire R, Cockrum P, Crider J, Schlech B. Topical antibacterial therapy for mycobacterial keratitis: potential for surgical prophylaxis and treatment. Clin Ther 2004 Feb;26(2):191-6.
4.Safranek TJ, Jarvis WR, Carson LA, et al. Mycobacterium chelonae wound infections after plastic surgery employing contaminated gentian violet skin-marking solution. N Engl J Med 1987 Jul 23;317(4):197-201.
5. Hamam RN, Noureddin B, Salti HI, et al. Recalcitrant post-LASIK Mycobacterium chelonae keratitis eradicated after the use of fourth-generation fluoroquinolone. Ophthalmology 2006 Jun;113(6):950-4.
Vol. No: 143:12Issue:
12/15/2006