
A 76-year-old white female with sudden vision loss in her right eye is referred emergently from her primary-care physician. Her visual acuity is light perception O.D. and 20/25 O.S. She has a marked relative afferent pupillary defect in the right eye. Ophthalmoscopic evaluation of the same eye reveals a pale, swollen optic disc with some peripapillary retinal hemorrhages. The left eye reveals no abnormalities.
Upon reviewing her medical history, she mentions that she was diagnosed with polymyalgia rheumatica but has received no treatment for the past eight months. She reports that she has been feeling poorly for the past four weeks with a flu and fever that she hasnt been able to shake. She says that she has lost more than 12 pounds during this time because she lost her appetite and chewing hurts her jaw. She also reports a constant temporal headache.
The most obvious diagnosis in this case is arteritic anterior ischemic optic neuropathy (AAION) secondary to giant cell arteritis (GCA). Erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP) are urgently performed and confirm the suspected diagnosis. The patient is then scheduled for a confirmatory temporal artery biopsy, but anti-inflammatory therapy must be initiated immediately to prevent vision loss in her left eye, which is currently uninvolved.
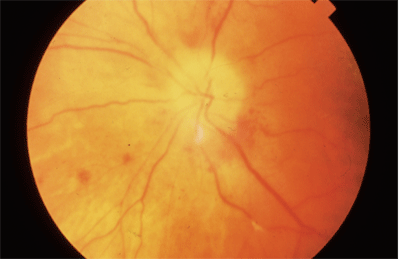 |
| Arteritic anterior ischemic optic neuropathy (AAION), seen here, is secondary to giant cell arteritis (GCA) in this diagnosis. |
Clearly, the patient needs systemic corticosteroids, but the amount and route of administration are not as obvious. Should the patient be given oral steroids, or should she be admitted to a hospital for intravenous (I.V.) steroids? This is the question that we attempt to answer in this months column.
GCA Explained
GCA is a granulomatous inflammation of medium- and large-sized arteries with defined internal and external elastic laminae.1 The muscular walls of these vessels are infiltrated by T lymphocytes, macro- phages, histiocytes, plasma cells and multinucleate giant cells. Histologic criteria for diagnosing GCA require that specimens show the infiltration of inflammatory cells within the vessel walls; giant cells need not specifically be present on biopsy to make the diagnosis.2,3
GCA is a multi-system, multi-symptom disorder that afflicts the elderly, and virtually any artery within the body may be involved. The degree of ischemia tolerated varies by system. There is often a symptomatic period of weeks to months before a diagnosis of GCA is reached.
Ocular symptoms of ischemia can include amaurosis fugax, intermittent diplopia and ophthalmoplegia prior to complete occlusion of the posterior ciliary, retinal or ophthalmic arteries. There is a much shorter interval until severe permanent vision loss ensues when these specific signs and symptoms are present.
Due to widespread vascular involvement in GCA, fatal myocardial infarction and cerebrovascular accident may occur. These events, however, are generally not attributed to GCA due to the advanced age of the patient at the time of the occurrence.4
 |
| Should a patient with GCA be treated with oral or intravenous steroids? |
The Therapeutic Conundrum
While the nature of GCA management is well known, the amount and route of steroid administration is controversial. Because of the high risk of morbidity of the disease, we lack controlled studies that could indicate the optimal dosage and administration of steroids. Clearly, when dealing with a disease that can rapidly cause blindness or death, studies involving placebos are inappropriate. Therefore, most information regarding successful treatment comes from case series and anecdotal reports.
Many reports suggest aggressive treatment with I.V. steroids followed by high-dose oral steroids.5-8 One report recommends that patients who have ophthalmologic complications receive three to four daily infusions of 250mg of methylprednisolone for three days.5 For oral administration, the initial prednisolone dose is 40 to 70mg/day. It should be reduced weekly by 5 to 10mg until 20mg/d, and then by 2.5mg until 10mg/d. At that point, the dose is reduced by 1mg per month, depending on symptoms, ESR and CRP.
While many clinicians advocate I.V. steroids, a 27-year study of steroid therapy for GCA found no difference between I.V. and oral routes of administration.9 This study included 145 patients who had GCA, as confirmed by temporal artery biopsy (96 with and 49 without visual loss). Patients were followed for six weeks or more, with a median follow-up time of 2.43 years. (Some cases exceeded 20 years.) I.V. megadose steroid therapy was initially given to 33% of patients followed by oral steroids; the rest received only oral therapy. The median starting dose of oral prednisone was 80mg/day. All patients were maintained at high-dose prednisone until ESR and CRP stabilized at low levels. Tapering of prednisone then began, guided by the ESR and CRP levels. The study found no evidence that intravenous megadose steroid therapy was more effective than oral therapy in improving vision or preventing visual deterioration due to GCA.
In an effort to reduce the levels of systemic steroids and their attendant complications, investigators have looked into adding systemic immunosuppresants to GCA treatment regimens. However, no corticosteroid-sparing benefit has been attributed to the combined methotrexate and corticosteroid therapy to date.10,11 One study found that adjunctive use of low-dose aspirin (100mg/day) in steroid-treated GCA patients decreases the rate of visual loss and cerebrovascular accidents from the disease, probably by suppressing proinflammatory cytokines in the vascular lesions of GCA.12,13
So, where does this leave clinicians when managing patients who have GCA? At the very least, high-dose oral prednisone should be started immediately. However, admitting the patient to the hospital for I.V. steroid therapy is certainly not inappropriate, given that oral and I.V. steroid therapy likely have similar outcomes for patients who have this disease.
Drs. Sowka and Kabat are full-time faculty members at Nova Southeastern University College of Optometry.
1. Rahman W, Rahman FZ. Giant cell (temporal) arteritis: an overview and update. Surv Ophthalmol 2005 Sep-Oct;50(5): 415-28.
2. Albert DM, Searl SS, Craft JL. Histologic and ultrastructural characteristics of temporal arteritis. The value of the temporal artery biopsy. Ophthalmology 1982 Oct;89:1111-26.
3. Ashton-Key M, Gallagher PJ. Surgical pathology of cranial arteritis and polymyalgia rheumatica. Baillieres Clin Rheumatol 1991 Dec;5:387-404.
4. Karger B, Fechner G. Sudden death due to giant cell coronary arteritis. Int J Legal Med 2006 Apr 27; [Epub ahead of print].
5. Schmidt WA. Current diagnosis and treatment of temporal arteritis. Curr Treat Options Cardiovasc Med 2006 Apr;8(2):145-51.
6. Hayreh SS, Zimmerman B, Kardon RH. Visual improvement with corticosteroid therapy in giant cell arteritis. Report of a large study and review of literature. Acta Ophthalmol Scand 2002 Aug;80(4):355-67.
7. Nordborg E, Nordborg C. Giant cell arteritis: strategies in diagnosis and treatment. Curr Opin Rheumatol 2004 Jan;16(1): 25-30.
8. Hwang JM, Girkin CA, Perry JD, et al. Bilateral ocular ischemic syndrome secondary to giant cell arteritis progressing despite corticosteroid treatment. Am J Ophthalmol 1999 Jan; 127(1):102-4.
9. Hayreh SS, Zimmerman B. Management of giant cell arteritis. Our 27-year clinical study: new light on old controversies. Ophthalmologica 2003 Jul-Aug;217(4):239-59.
10. Spiera F, Mitnick HJ, Kupersmith M, et al. A prospective, double-blind, randomized, placebo controlled trial of methotrexate in the treatment of giant cell arteritis (GCA). Clin Exp Rheumatol 2001 Sep-Oct;19(5):495-501.
11. Hoffman GS, Cid MC, Hellmann DB, et al. A multicenter, randomized, double-blind, placebo-controlled trial of adjuvant methotrexate treatment for giant cell arteritis. Arthritis Rheum 2002 May;46(5):1309-18.
12. Nesher G, Berkun Y, Mates M, et al. Low-dose aspirin and prevention of cranial ischemic complications in giant cell arteritis. Arthritis Rheum 2004 Apr;50(4):1332-7.
13. Weyand CM, Kaiser M, Yang H, et al. Therapeutic effects of acetylsalicylic acid in giant cell arteritis. Arthritis Rheum 2002 Feb;46(2):457-66.

