 |
History
A 52-year-old black male reported to the office with a chief complaint of a lump in the left eyelid. He explained that the lump had been progressively worsening over the last four months. His systemic and ocular histories were unremarkable and he denied exposure to chemicals or allergies of any kind.
Diagnostic Data
His best-corrected entering visual acuities were 20/20 in each eye at distance and near. His external examination was normal with no evidence of afferent pupil defect. The pertinent anterior segment findings are demonstrated in the photograph. Goldmann applanation tonometry measured 15mm Hg OU. Dilated funduscopy was within normal limits, both eyes, revealing symmetric cup-to-disc ratios measuring 0.3/0.3 OD and 0.3/0.35 OS, respectively, with normal peripheries.
Discussion
Additional testing should include palpating the lesion—evaluating for firmness, potential extension, elicitation of pain to rule out cellulitis and ease of motility. Observation should be completed to rule out madarosis and additional historical questions must include whether or not similar lesions have been excised before.
This patient’s diagnosis is a chalazion. Chalazia typically present as one or more focal, firm, painless nodules in the upper or lower eyelid.1-7 While many patients seek care because of cosmetic concern, some cases of larger lesions may produce mechanical ptosis resulting in some degree of obstructed vision. In many instances, especially when the lesions are small or off the central axis, patients may be unaware of their presence. The lesions do not cause discomfort, though a history of a painful lid infection (such as a hordeolum or preceptal cellulitis) may be uncovered prior to its discovery. Enlargement of the lesion over time is possible. Often, there is a history of concurrent blepharitis, usually in the form of meibomian gland obstruction/dysfunction.1-7 In some patients, chalazia may be recurrent and indicative of chronic blepharitis, lid hygiene issues, acne rosacea or, in rare cases, meibomian gland carcinoma.5 Men appear to be affected somewhat more often than women.8
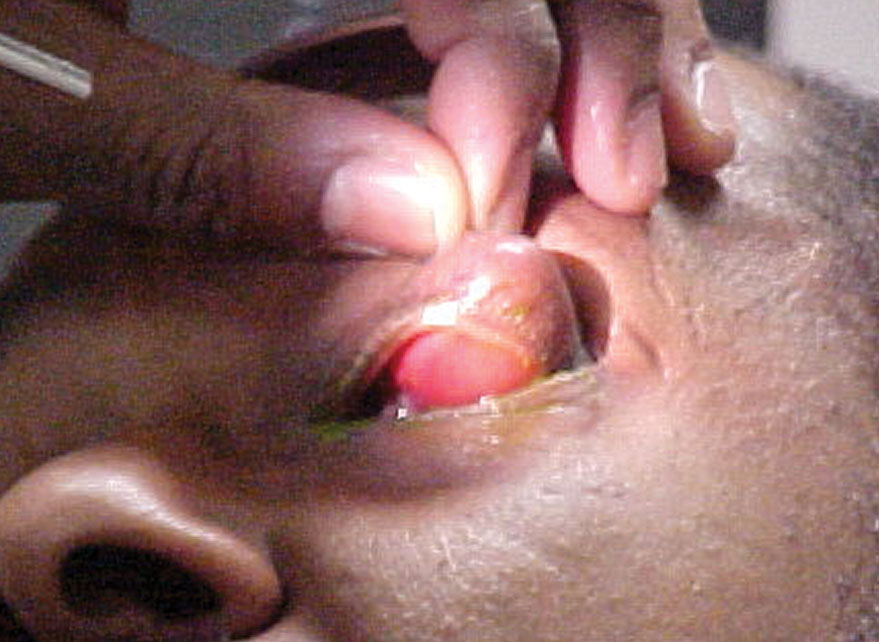 |
| Can this image of our 52-year-old patient’s presenation help you identify his diagnosis? Click image to enlarge. |
Chalazia are the most common inflammatory lesion of the eyelid.1,4-6 They are non-infectious and sterile, representing a lipogranulomatous inflammation of the sebaceous meibomian gland(s).4 The typical etiology is obstruction of meibomian ducts with resultant retention of glandular secretions.4 This frequently occurs in cases of chronic posterior blepharitis.2,7,8 Occasionally, chalazia form from the collection of inflammatory cells following eyelid infection such as a hordeolum or preseptal cellulitis; this is referred to as a secondary chalazion.2
Histological evaluation of chalazia reveals an inert collection of corticosteroid-sensitive histiocytes, multinucleate giant cells, plasma cells, polymorphonuclear leukocytes and eosinophils.7,8 The nodule is encapsulated by connective tissue, often interdigitating with the tarsal plate.
Treatment
In cases not exhibiting concurrent infection, the use of oral antibiotics is unnecessary. While chalazia do respond to anti-inflammatory therapy, the anatomically deep nature of this condition renders topical medication virtually ineffective. Nevertheless, warm compresses (to clear the meibomian ducts of stagnant oils), accompanied by gentle digital massage (to rupture and express the nodule) can be attempted on a TID-QID basis for lesions discovered early in their process (less than three weeks old).9-12 Unfortunately, this therapy tends to be ineffective, with less than 25% of lesions resolving spontaneously or with hot compresses.9-12
Patients with chalazia should be cautioned against vigorous massage of the involved area. While gentle massage is beneficial, vigorous massage may cause further extravasation of the granulomatous inflammation into the surrounding tissue and exacerbation or complication of the condition.
Chalazia that do not respond to conservative therapy can be treated with excision or intralesional corticosteroid injection.10,13-17 Studies document a success rate of approximately 80% to 90% using intralesional injection.10,13-17 Using a standard 1cc tuberculin syringe and 30-gauge needle, 0.1ml to 0.3ml of triamcinolone acetonide 10mg/ml or 40 mg/ml is injected directly into the lesion. The approach should preferably be from the palpebral side, since eyelid skin depigmentation may occur when the injection occurs on the dermal side.17 This side effect is more common in dark-skinned individuals.17 The use of a chalazion clamp and topical anesthesia may be helpful, but is not absolutely necessary.15 One report documented adequate anesthesia with topical lidocaine gel only.6 The study noted success compared with procedures with standard injectable anesthesia.6
Patients usually demonstrate marked improvement within one week of initial treatment, though repeat injections may be necessary for larger chalazia.12-17 Should intralesional steroid injections prove ineffective or if the patient cannot tolerate the procedure, surgical curettage under local anesthesia is indicated.
Recurrence
Finally, recurrent multiple giant chalazia have been recognized as an ophthalmic feature of Job's syndrome (hyperimmunoglobulinemia E with connective tissue, skeletal and immunologic abnormalities).18,19 In addition to meibomian gland carcinoma, this unusual syndrome should be suspected in cases where recurrent giant chalazia are documented, regardless of the patient's age.18 Measurement of serum IgE and eosinophils is essential to establish a proper diagnosis.18
While vision problems are uncommon with chalazia, large lesions may cause a mechanical ptosis and resultant obscuration of the vertical visual field. For this reason, it is important to treat chalazia aggressively in young children. Obscuration of the visual field in children has been documented to produce a deprivational amblyopia. Also, the induced chronic external pressure produced by larger lesions can induce alterations in corneal curvature; several cases of chalazion-induced astigmatism have been documented.20,21
Recurrent chalazia, especially those that recur in the same location within the same lid after surgical excision or lesions associated with maderosis, warrant excisional biopsy.5 The greatest concern in these cases is sebaceous gland carcinoma.5 This is an extremely aggressive form of eyelid malignancy, which carries a high mortality rate and great propensity toward metastasis. Although the majority of misdiagnosed recurrent chalazia represent sebaceous gland carcinomas, other significant lesions include basal cell carcinoma and pyogenic granuloma.6,7
This patient’s chalazion was removed using the standard surgical approach from the palpebral side. Despite its size, the surgeon did not work the patient up for Job’s syndrome. The patient was referred back to our office for follow-up care with Tobradex (tobramycin/dexamethasone, Novartis) BID in the left eye. Over a three-week period, the lesion healed without complications or raised intraocular pressure.
|

