 |
History
A 38-year-old Asian male presented emergently following blunt trauma from a fist. While there was pain to the touch, the eye didn’t ache and vision was not compromised. He did explain that he saw double when he looked to his left. The patient was otherwise free of systemic disease, previous history of trauma or ocular surgery. He denied having any allergies to medications or the environment.
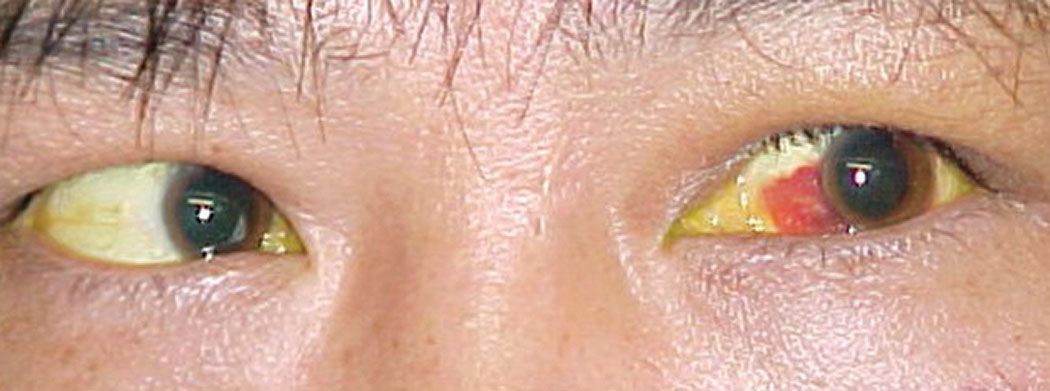 |
| The patient’s left eye demonstrated subconjunctival hemorrhage and he reported double vision. Click image to enlarge. |
Diagnostic Data
His best-corrected entering visual acuity was 20/20 OU. His external exam was unremarkable, with no evidence of afferent pupillary defect. Biomicroscopic evaluation of the anterior segment showed mild ecchymosis adjacent to the area of impact and a small subconjunctival hemorrhage, OS. The pertinent exam finding is demonstrated in the photograph. Goldmann applanation tonometry measured 17mm Hg OU.
Additional testing included forced duction motilities to expose the limits of range of motion and magnetic resonance imaging of the face and head.
Discussion
Blunt trauma to the orbital rim is the typical cause of orbital floor and medial orbital wall fractures.1-4 While there is no epidemiologic predilection for “blowout fracture,” there are clinical trends regarding those most likely to sustain these injuries: male, between the ages of 18–30, engaged in activities of poor judgment with most incidents occurring in or near the home.3,5-8 Traffic accident is the most common cause of unilateral or bilateral blowout fracture in males between the ages of 30-60 years with violent assault also seen commonly.7,8
The specific term “blowout fracture” is reserved to connote an isolated orbital floor or medial wall fracture in the setting of an intact orbital rim.1-4 Patients present with a history of blunt-force trauma, such as being struck with a projectile, like a ball, bat or fist, or being a participant in a collision injury, such as those caused by the impact of an air bag or contact with an object following a fall.7-9
Pain, photophobia and lacrimation associated with post-traumatic uveal inflammation (iritis or iridocyclitis), variable facial swelling secondary to fluid or air (orbital emphysema), crepitus (a crackling noise when tissue infiltrated with air is palpated), gaze-evoked diplopia and pain upon movement of the eyes are all common.6-10
Other associated collateral injuries may include subconjunctival hemorrhage, ruptured globe, corneal abrasion, conjunctival laceration, hyphema, iridodialysis, lenticular subluxation, retinal detachment, vitreous hemorrhage, choroidal rupture, traumatic optic neuropathy and optic nerve evulsion. If the eye settles inferiorly or medially into the exposed sinus, enophthalmos with restricted ocular motility will be present with or without loss of facial sensation.1-10
The seven bones of the orbit include the frontal, zygomatic, maxillary, ethmoid, sphenoid, lacrimal and pterygopalentine.4,11 The orbital roof includes the orbital plate of the frontal bone and the lesser wing of the sphenoid; the lateral wall is composed of the zygomatic bone and the greater wing of the sphenoid; the floor of the orbit is composed of the orbital plate of the maxilla, the zygomatic and orbital process of the pterygopalentine bone; the medial wall of the orbit is composed of the maxilla, the lacrimal, the ethmoid and body of the sphenoid.4,11
The other critical anatomical players are the surrounding paranasal air sinuses.12 Several sinuses surround the orbit help to lessen the weight of the skull and aid in the resonance of the voice.12 Pneumatized ethmoid air cells, which maintain structural stability and resist fractures of the medial orbital wall, act as a safeguard for the eyeball during trauma.4 Unfortunately, these structures leave the superior, medial and inferior walls of the orbit less supported and vulnerable to catastrophic failure (blowout fracture, trap door fracture) from blunt force trauma. The sinuses surrounding the orbit include the ethmoidal air cells (anterior, middle and posterior), the sphenoidal sinuses, the maxillary sinuses and the frontal sinuses.11,12
There is some debate about the mechanism of blowout fracture. These injuries can be classified into three types: greenstick (partial break), simple and complex.13 When a blunt force impacts the face, it may produce a combination of effects: (1) the force may strike the bone producing a shock wave, causing “bone buckling,” (2) the force may be transmitted to the eyeball, causing the globe to strike one of the orbital walls such that it fractures (“eye to wall”) or (3) the force may be transmitted by the globe, via the principle of fluid incompressibility, causing generalized increased orbital content pressure or a “hydraulic” effect resulting in bone fractures.12-17
The point of breakage usually occurs along the axis of least support in an area where the tissue is weakest.13-17 Since the orbital floor is not parallel to the horizontal plane, the vector of the striking force seems to affect the resultant fracture patterns.12 While all three mechanisms are mentioned in the literature, the “buckling” mechanism and the hydraulic mechanism seem to have the most support.14-17 Fractures produced by the “buckling” mechanism are often limited to the anterior part of the orbital floor.14 In contrast, “hydraulic” fractures are often larger, involving both the anterior and posterior parts of the floor as well as the medial wall of the orbit.16,17
The orbital floor has a lower threshold for fracture than the medial wall and other orbital bones and occurs most commonly. When it gives way, the globe and its attached components become unsupported, slipping down into the vacant sinus below, producing visible enophthalmos and gaze-evoked, symptomatic diplopia along with degrees of extraocular muscle dysfunction and infraorbital nerve hypoesthesia.15-18
The treatment of blowout fracture centers around ocular first aid. The most challenging aspect of beginning an examination on patients that have encountered facial blunt-force injury is getting the eye open so as to take a look. Facial and orbital swelling or orbital emphysema can literally force the lids shut. Here, a lid retractor can be placed in between the eye lids and used as a speculum to achieve lifting of the superior lid or lowering of the inferior lid.
Eyes sustaining blunt-force trauma must have proper imaging to rule out concomitant maxillofacial-orbital fracture or ruptured globe.17 Facial lacerations can be treated with topical antibiotics unless they require cosmetic or functional closure. Seidel testing is essential to rule out perforating injuries. Topical anti-infective drops can be prescribed for any observed conjunctival/corneal laceration or abrasion and topical and oral anti-inflammatory therapy can be used for resultant ocular inflammation along with the appropriate strength topical cycloplegic. Topical and oral nonsteroidal preparations can assist with analgesia.
Since blunt ocular trauma involving the eye or face is the result of being struck by an object at velocity, a shockwave within the local area is generated upon contact. This produces what is known as the “coup” injury, from the French/Scottish derivation meaning “to upset.” Injuries may also seen directly opposite the impact point, in line with the shockwave; these are known as the “contrecoup” effects, (from the French derivation meaning “occurring at a site opposite the area of impact”). For these reasons, dilated fundus evaluation ruling out vitreous hemorrhage, retinal tearing and retinal detachment are required.
Computed tomography (CT) remains the gold standard for assessing orbital fractures.4,17,19 The CT technology (multislice CT) has improved the acquisition of coronal images of the orbit without the need for hyperextension of the neck.4,19 Treatment of blowout fracture may not be emergent. If there is a compressive threat to the optic nerve via swelling and retrobulbar hemorrhage, that will require referral for an emergent lateral canthotomy and orbital decompression. Typically, surgical intervention is postponed until orbital health is consistent with a good surgical environment unless large amounts of soft tissues are incarcerated in the bony ruture.13,17,20 Management of orbital floor fractures traditionally has been accomplished through transnasal, transcutaneous, transconjunctival, transcaruncular and subciliary incisions.13,17,19 However, postoperative lid malposition is a complication.18 Some surgeons have begun to evaluate an endoscopic approach to orbital floor fractures. The endoscopic approach offers a hidden incision and improved fracture visualization.21
When the orbital floor requires replacement (inlay technique) or reconstruction (repositioning technique), numerous materials are available to make the repair.17,22 Autologous materials include bone, cartilage, fascia lata and periosteum.17 Natural materials are favored because of their mechanical properties, ability to revascularize and low potential for infection or scarring.17 Other materials include titanium, porous polyethylene, resorbable materials, gel films, bioglass and silastic sheeting.17
In cases that are seen before an orbital fracture is diagnosed and in cases of orbital fracture where surgery is being postponed or not being considered, a course of broad-spectrum oral antibiotics such as keflex or amoxicillin 500mg BID PO is indicated to protect against secondary infection while the osseous tissues heal.
Patients presenting following orbital blunt trauma should be discouraged from nose blowing until orbital fractures can be positively ruled out via imaging (X-ray, CT or magnetic resonance imaging). This helps to avoid the unwanted complication of orbital emphysema. The only way to diagnose definitively diagnose an orbital fracture is by neuroimaging. Air from the external environment may enter the subcutaneous tissue surrounding the orbit or globe via a communication created by a fracture. This is often visible as “soft” or “puffy” swelling, known as orbital emphysema.
| 1. Lelli GJ Jr, Milite J, Maher E. Orbital floor fractures: evaluation, indications, approach and pearls from an ophthalmologist’s perspective. Facial Plast Surg. 2007; 23(3):190-9 2. Burm JS, Chung CH, Oh SJ. Pure orbital blowout fracture: new concepts and importance of medial orbital blowout fracture. Plast Reconstr Surg. 1999; 103(7):1839-49. 3. Guly CM, Guly HR, Bouamra O et al. Ocular injuries in patients with major trauma. Emerg Med J. 2006;23(12):915-7. 4. Kim YH, Park Y1, Chung KJ. Considerations for the Management of Medial Orbital Wall Blowout Fracture. Arch Plast Surg. 2016;43(3):229-36. 5. McGwin G Jr, Owsley C. Incidence of emergency department-treated eye injury in the United States. Arch Ophthalmol. 2005; 123(5):662-6. 6. Lee J, Lee HK, Lee H, et al. Epidemiology of Oculoplastic and Reconstructive Surgeries Performed by a Single Specialist With 15 Years’ Experience at a Tertiary Center. J Craniofac Surg. 2015;26(4):e308-11. 7. Roh JH, Jung JW, Chi M. A clinical analysis of bilateral orbital fracture. J Craniofac Surg. 2014;25(2):388-92. 8. Shin JW, Lim JS, Yoo G, Byeon JH. An analysis of pure blowout fractures and associated ocular symptoms. J Craniofac Surg. 2013;24(3):703-7. 9. Lehto KS, Sulander PO, Tervo TM. Do motor vehicle airbags increase risk of ocular injuries in adults? Ophthalmology. 2003; 110(6):1082-8. 10. García-Medina JJ, García-Medina M, Pinazo-Durán MD. Severe orbitopalpebral emphysema after nose blowing requiring emergency decompression. Eur J Ophthalmol. 2006;16(2):339-42. 11. Snell RS, Lemp, MA. The orbital cavity. In: Snell RS, Lemp, MA. Clinical anatomy of the eye 2nd ED. Blackwell Science, Malden, MA 1998: 59-77. 12. Snell RS, Lemp, MA. The The paranasal sinuses. In: Snell RS, Lemp, MA. Clinical anatomy of the eye 2nd ED. Blackwell Science, Malden, MA 1998: 78-89. 13. Chung KJ, Lim JH, Kim TG, et al. Correction of Medial Blowout Fractures According to the Fracture Types. Ann Plast Surg. 2016;76(1):46-50. 14. Burnstine MA. Clinical recommendations for repair of orbital facial fractures. Curr Opin Ophthalmol. 2003; 14(5):236-40. 15. Nagasao T, Miyamoto J, Nagasao M et al. The effect of striking angle on the buckling mechanism in blowout fracture. Plast Reconstr Surg. 2006; 117(7):2373-80. 16. Ahmad F, Kirkpatrick NA, Lyne J et al. Buckling and hydraulic mechanisms in orbital blowout fractures: fact or fiction? J Craniofac Surg. 2006; 17(3):438-41. 17. Yong-Ha Kim, Youngsoo Park, Kyu Jin Chung. Considerations for the Management of Medial Orbital Wall Blowout Fracture. Arch Plast Surg. 2016;43(3): 229–236. 18. Rhee JS, Kilde J, Yoganadan N et al. Orbital blowout fractures: experimental evidence for the pure hydraulic theory. Arch Facial Plast Surg. 2002; 4(2):98-101. 19. Cruz AA, Eichenberger GC. Epidemiology and management of orbital fractures. Curr Opin Ophthalmol. 2004; 15(5):416-21. 20. Harris GJ. Orbital blow-out fractures: surgical timing and technique. Eye. 2006 ; 20(10):1207-12. 21. Farwell DG, Strong EB. Endoscopic repair of orbital floor fractures. Facial Plast Surg Clin North Am. 2006; 14(1):11-6. 22. Ozturk S, Sengezer M, Isik S, et al. Long-term outcomes of ultra-thin porous polyethylene implants used for reconstruction of orbital floor defects. J Craniofac Surg. 2005; 16(6):973-7. |

