 |
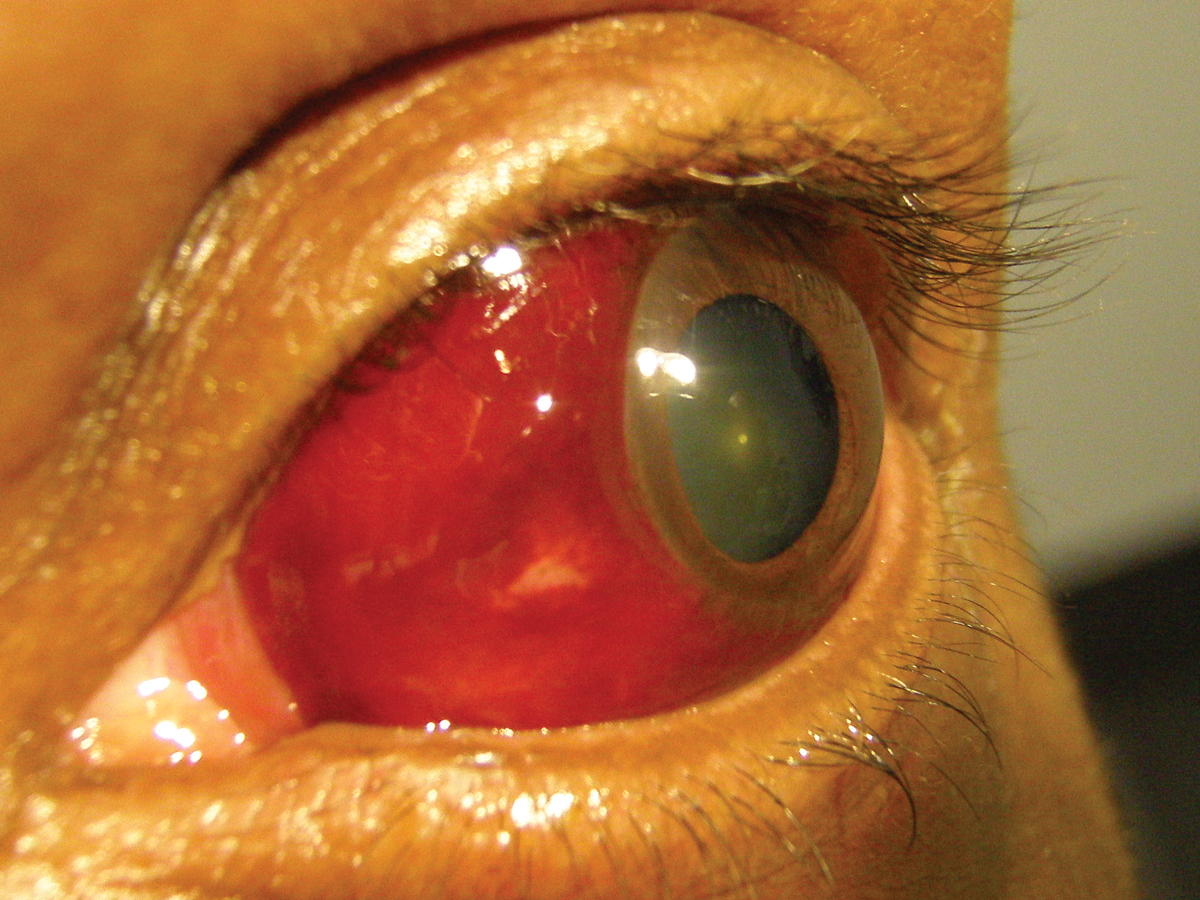
Despite enactment of the ACA, eye-related conditions presenting to the ED did not decrease. A high percentage of visits still focused on non-emergent conditions such as subconjunctival hemorrhage. Photo: Andrew S. Gurwood, OD. Click image to enlarge. |
Recent findings suggest that while the Affordable Care Act (ACA) increased insurance coverage for Americans, it did not decrease emergency department (ED) reliance for the management of eye-related conditions.
This retrospective, cross-sectional study included patients who presented to the ED with an eye-related primary diagnosis. Researchers used nationally representative data from the US Nationwide Emergency Department Sample to analyze eye-related ED visits before (2010-2013) and after (2014-2017) the ACA was mandated. They categorized ED visits as emergent, non-emergent or indeterminate.
During the 2010-2017 study period, a total of 16,808,343 eye-related ED visits occurred in the United States. Of these, 8,088,203 occurred before the ACA was mandated and 8,720,766 happened after it went into effect.
The researchers observed an initial decline in the incidence of eye-related ED visits following the ACA mandate, from 652.4 per 100,000 people in 2013 to 593 per 100,000 people in 2014. Following this, they reported a rapid increase in incidence to 658.5 per 100,000 people in 2015 and a further increase to 746.6 per 100,000 people in 2016.
The data showed that the percentage of uninsured patients decreased from 19% to 14.3% while individuals with Medicaid coverage increased from 29.4% to 36%. The study authors found that the increase in ED use was greatest among individuals in the lowest income category.
During the study period, they reported that 44.8% of ED visits were due to non-emergent eye conditions. More than one-third (35.0%) of non-emergent ED visits were due to conjunctivitis, styes/chalazion and subconjunctival hemorrhage, the researchers found. That these common and fairly innocuous conditions are still being seen in a hospital emergency ward shows the extent of work still needed to improve the efficient delivery of eyecare in America. The percentage of visits for a non-emergent cause did decline slightly, from 46.4% pre-ACA to 43.2% post-ACA.
“Our study shows that although the ACA increased insurance coverage for Americans, especially those belonging to low socioeconomic status, it did not result in decreased ED reliance for ophthalmic conditions,” the study authors concluded in their paper for the Ophthalmology journal. “A significant proportion of ED visits continue to be for non-emergent ophthalmic conditions which can be managed in the outpatient setting. This results in more costly and less specialized care.”
They noted that additional measures—beyond expanding insurance coverage—may be required to ensure all Americans have access to high quality, efficient and more equitable outpatient eye care.
Mir TA, Mehta S, Qiang K, et al. Association of the affordable care act with eye-related emergency department utilization in the United States. Ophthalmology. July 2, 2022. [Epub ahead of print]. |

