 |
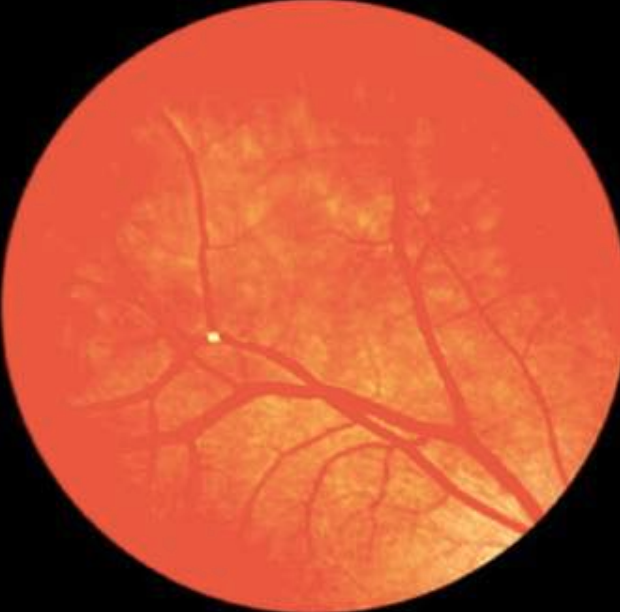
The risk for RVO after the first mRNA COVID-19 vaccination is not significantly different from the risk with influenza and Tdap vaccinations. Photo: Julie Rodman, OD. Click image to enlarge. |
Good news for those who worry about ocular adverse effects of COVID-19 vaccines: researchers find the risk of retinal vein occlusion (RVO) extremely low. The Cleveland-based team compared the COVID-19 mRNA vaccines from Pfizer and Moderna with two historically used ones—influenza and Tdap—in a database of more than 103 million patients. Electronic health records were searched for the presence of vaccination CPT codes and instances of newly diagnosed RVO within 21 days of vaccination were recorded and reported. Propensity score matching based on demographic characteristics (age, sex, race and ethnicity) and comorbidities (diabetes, hypertension and hyperlipidemia) was performed between vaccination groups for evaluation of relative risks.1
Of more than three million patients who received an mRNA COVID-19 vaccine, the study showed that 0.003% of patients had a new diagnosis of RVO within 21 days. The number in patients who received a second dose of the COVID-19 vaccine was less than half of those who received a first dose. While a similar risk for RVO after influenza and Tdap vaccinations compared with the first dose mRNA COVID-19 vaccination was found, the authors noted that it was important to consider that influenza and Tdap vaccination queries were performed from 2018 to 2019 to eliminate the possibility of COVID-19 vaccination within this group.
The decreased risk for RVO after the second dose of the vaccine compared with the first dose may be explained by a true increased physiologic risk for RVO after the first dose, possibly that a naïve immune response is more likely to provoke a hyperviscous state related to RVO, the authors noted in their paper for JAMA Ophthalmology. “However, this finding may also be explained by a hesitancy to receive the second dose based on symptoms that occur after the first dose, uncontrolled differences in patient populations, differences in patient insurance status or differences in recording practices between the two events,” they wrote.
Authors noted that differences in willingness to present to a health care professional with possible RVO must be considered as substantial changes in ophthalmology visits were observed during the COVID-19 pandemic.
“The results do not intend to belittle the experience of patients with debilitating vision loss after vaccination but aim to describe how often this phenomenon occurs as a contribution to the safety profile of the first mRNA vaccine widely administered in humans,” the authors explained. “The results of the post hoc analysis additionally suggest that the risk for a new-encounter RVO diagnosis is greater acutely after COVID-19 infection itself than after the mRNA COVID-19 vaccine.”1
In response to this study, a commentary also published in JAMA Ophthalmology pointed out that it’s very difficult to determine whether the association of RVO and prior vaccination was coincidental. Other vascular diseases have been attributed to COVID-19 vaccines, and it should be noted that different vaccines could have different adverse effects.2
Because of the low incidence of RVO, the study had limited feasible approaches to evaluate risk factors for retinal vascular occlusion after vaccination. “The authors have chosen a straight-forward approach of a cohort study by identifying people who had received one of the two mRNA vaccines and then examining their records for 21 days after vaccination, a period of time that seems reasonable if indeed the vaccine causes retinal vascular occlusion,” the commentary authors explained. “The challenging aspect of such studies is the choice of comparable comparison group. The authors used an ingenious approach by also reviewing cohorts of patients who received influenza or tetanus, diphtheria, pertussis (Tdap) vaccines.”
This has advantages and disadvantages. By comparing only people who have received some sort of vaccine, the groups may have been more comparable with respect to health behaviors and access to care, factors that are not generally available in the EHR.
The commentary authors also explained that the results do not provide a comparison with a group of people who did not receive any recent vaccination, or especially those who did not receive the COVID-19 vaccine.
“Without a comparable group of people without mRNA COVID-19 vaccination, it is difficult to rule out an association between mRNA COVID-19 vaccination and retinal vascular occlusion based on the results provided by Dorney and coworkers,” they wrote. “Nonetheless, the very low incidence is noteworthy. However, these results for mRNA vaccines are not applicable to other COVID-19 vaccines, such as viral vector and protein subunit vaccines, which could have different results.”
“We should realize that evidence associating other vaccinations, such as hepatitis A and B and influenza, with inflammatory or vascular retinal problems is very weak, with just a few case reports,” the commentary concluded. “We do not know whether these vaccinations increase the risk of retinal vascular occlusion or other retinal complications.”2
1. Dorney I, Shala J, Kaelber DC, et al. Risk of new retinal vascular occlusion after mRNA COVID-19 vaccination within aggregated electronic health record data. JAMA Ophthalmol. April 13, 2023. [Epub ahead of print]. 2. Jampol LM, Maguire MG. No red flags for risk of retinal vascular occlusion after mRNA COVID-19 vaccination. JAMA Ophthalmol. April 13, 2023. [Epub ahead of print]. |

