 |
Nothing makes your heart race faster than a patient who presents with the words, Doc, I splashed something in my eyes! Depending on the substance, a chemical ocular injury can represent a sight-threatening emergency. As a clinician, you must recognize products that can cause harm to the eyes, and act quickly to minimize pain and prevent serious complications.
Sources of Chemical Injury
Chemical injuries typically fall into two categories: those caused by acids and those caused by alkalis (bases).
Acidic substances bind with corneal and conjunctival proteins and coagulate the surface epithelium. This creates a barrier to further penetration, so acid burns typically are confined to superficial tissues. Common sources of acid burns include toilet bowl cleaners, older car batteries and additives for swimming pools (muriatic acid). Weaker acids are found in food items, such as vinegar or concentrated lemon juice.
Alkaline agents can induce far more serious burns. These substances saponify the fatty components of the cornea, thereby destroying the cell structure. In effect, strong alkalis melt the corneal epithelium and stroma and may continue to penetrate deeper into the ocular tissues, even after the initial trauma. Alkaline burns occur more frequently than acid burns. Common sources include detergents and household cleaners, ammonia, bleach, pool chlorinators, and lime (calcium oxide, a component of cement).
In general, we categorize acids as substances that have a pH of 6.0 or lower and alkalis as those that have a pH of 8.0 or higher. However, many other substances do not fall neatly into the acidic or alkaline category but can still cause ocular injury. Alcohol is one such substance.
Depending on the concentration, alcohol can cause a significant (though self-limiting) keratitis with an associated inflammation of the ocular surface structures. Isopropyl alcohol, methanol and ethanol can all induce this type of ocular injury. This means that everything from hairspray to vodka is a potential ocular irritant. The severity of the burn depends on the concentration of the liquid and whether there are other potentially toxic additives.
 |
|
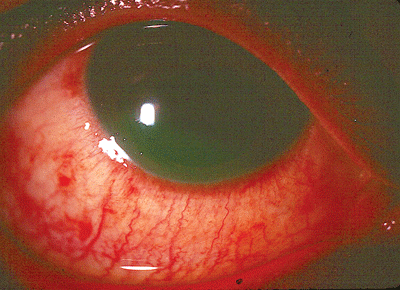
An eye that sustained a chemical burn from alcohol. |
Organic irritants, such as hot pepper sauce or pepper spray, are also potential culprits for ocular injury. The irritants in these products, called capsaicinoids, are derived from the peppers placentaa white tissue inside the fruit that envelops the seeds. Oleoresin capsicum is the distilled, concentrated derivative of the peppers placentas; this is the primary ingredient in pepper spray, which is used for law enforcement and personal defense. Pepper spray is known to cause significant pain and lacrimation with resultant epithelial erosions and has been linked with potential neurotrophic damage.1,2
Feel the Burn
Its easy to get flustered when faced with a chemical injury. The patient is often in severe pain, the presentation can be dramatic, and time is working against you. But the successful clinician remembers to apply the appropriate diagnostic and therapeutic measures in the proper order:
Irrigate the eye. Do this regardless of the type of chemical or the duration of the exposure. If the patient calls the office, instruct him to flush his eyes with water (via a shower, water fountain, garden hose, etc.) for at least 20 minutes before coming to the office. If he does not call first, rinse his eyes immediately with water or saline upon presentation. This is a critical issue, as copious irrigation helps neutralize the injury and prevent further damage to the ocular tissues.
Obtain a history. Following (or during) the irrigation process, obtain a detailed history regarding the nature of the injury and, if possible, the offending substance. If acidic or alkaline in nature (or if the patient is unsure of the substance), test the conjunctiva with litmus paper, and continue irrigating until the pH is neutral (i.e., between 6.0 and 8.0).
Always remember to obtain as detailed an ocular and systemic history as possible once the situation has been stabilized. This is important, as you do not wish to prescribe medically contraindicated drugs, or overlook potentially confounding ocular disorders (e.g., cataracts, glaucoma, etc.).
Sweep the lid surface and fornices. Once youve assessed the damage with biomicroscopy, sweep the lid surface and fornices of any particulate matter using a cotton-tipped applicator moistened with antibiotic solution. This is particularly important if the injury involved cement or drain cleaner because these represent depot accumulations of alkaline material, which will continue to degrade the ocular tissues. Also, debride any necrotic corneal or conjunctival tissue from the ocular surface. This minimizes the antigenic response and helps initial re-epithelialization by virtue of a smooth, uniform basement membrane.
Prescribe appropriate agents. Instill a strong cycloplegic, such as scopolamine 0.25% or atropine 1%, to ameliorate secondary inflammation.
Topical corticosteroids, such as prednisolone acetate 1% q2-4h may be extremely beneficial in the first few days following trauma.3 However, steroids must be used judiciously, as prolonged use (i.e., >10 days) may induce collagen breakdown and corneal melting.4
Prophylactic antibiotics are essential in cases of chemical keratitis. Topical fluoroquinolones (e.g., moxifloxacin, gatifloxacin) or aminoglycosides (e.g., tobramycin) q.i.d. are acceptable choices.
If pain is substantial, as it often is with chemical injuries, the addition of topical nonsteroidal anti-inflammatory drugs (e.g., ketorolac tromethamine 0.4% q.i.d.) may be beneficial.5 Consider oral narcotic analgesics for only the most symptomatic individuals.
Patients with chemical injuries should be evaluated daily. While most will improve over time, those with alkaline burns have the worst prognosis and often require surgical intervention. Also realize that secondary glaucoma is a common late complication associated with chemical burns.
Drs. Sowka and Kabat are members of Alcons speakers alliance. They have no financial interest in any of the products mentioned.
1. Zollman TM, Bragg RM, Harrison DA. Clinical effects of oleoresin capsicum (pepper spray) on the human cornea and conjunctiva. Ophthalmology 2000 Dec;107(12):2186-9.
2. Holopainen JM, Moilanen JA, Hack T, Tervo TM. Toxic carriers in pepper sprays may cause corneal erosion. Toxicol Appl Pharmacol 2003 Feb 1;186(3):155-62.
3. Donshik PC, Berman MB, Dohlman CH. Effect of topical corticosteroids on ulceration in alkali-burned corneas. Arch Ophthalmol 1978 Nov;96(11):2117-20.
4. Brown SI, Weller CA, Vidrich AM. Effect of corticosteroids on corneal collagenase of rabbits. Am J Ophthalmol 1970 Nov;70(5):744-7.
5. Kaiser PK, Pineda R II. A study of topical nonsteroidal anti-inflammatory drops and no pressure patching in the treatment of corneal abrasions. Corneal Abrasion Patching Study Group. Ophthalmology 1997 Aug;104(8):1353-9.

