 |
A 66-year-old Asian female presented with a chief complaint of burning in her left eye for the past three months. She spoke limited English, which made it difficult (at least initially) to obtain a thorough history. Her medical history included diabetes, hypertension and high cholesterol, for which she was taking metformin, amlodipine and atorvastatin.
Best-corrected visual acuity was 20/200 OD and 20/60 OS. The reduction in her right eye was attributed to amblyopia, and the reduction in the left eye was attributed to nuclear sclerosis. Pupils were normal, round and equally reactive to light.
Gross observation showed facial asymmetry with the left eye pushed down and out. Extraocular motilities showed a restriction on upgaze (80%) and adduction (50%). Due to the language barrier, she was unable to perform cover test.
Exophthalmometry revealed proptosis in the left eye, which measured 15/19.5mm, and resistance to retropulsion was noted in the left eye. Other than cataracts, her anterior and posterior segments were unremarkable. Neither disc edema nor pallor was noted in either eye.
Upon further and more specific questioning, our patient reported the burning was periorbital—around her left forehead and left nostril. She also reported seeing double for the past few months.
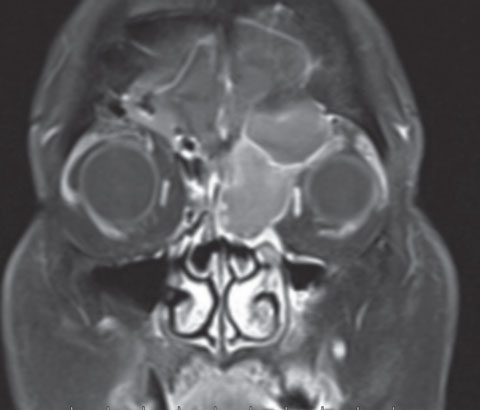 |
| Post-contrast coronal image shows a large left frontal sinus mass extending into the left orbit and ethmoid sinus, with peripheral enhancement of the lesion. |
Given our clinical findings and patient history, the most likely etiology was a compressive lesion. An orbital MRI was ordered with and without contrast, which revealed a large frontal sinus mass extending into the left orbit and left ethmoid sinus. The mass was hyperintense on T1 and showed minimal peripheral enhancement. Correlating the radiologic and clinical findings, this was most consistent with a mucocele; however, a soft tissue mass could not be excluded.
Our patient was referred to an ENT for further evaluation. A CT was performed to evaluate the extent of bone erosion, which was significant, and included anterior skull base erosion. She underwent endoscopic sinus surgery with ENT and neurosurgery; the surgeon confirmed and drained a mucocele. Two months later our patient showed complete resolution of her diplopia, headache, eye and nose pain. Her eyes were symmetrical, extraocular movements were full and exophthalmometry measured 15/16mm.
Discussion
The paranasal sinuses—air-filled spaces around the nasal cavity—include the frontal, sphenoid, maxillary and ethmoid sinuses. Sinus ostia are openings in the sinus cavities that connect and drain to the nasal cavity. Paranasal sinus mucoceles are mucus-filled cystic masses that result from obstruction of the sinus ostia.1 As mucoceles expand, they can cause bone erosion and displace surrounding structures.2 The frontal sinus is most commonly afffected (approximately 60 to 89%), and because of the close anatomic location, mucoceles can often spread intraorbitally and intracranially.2 Mucoceles can occur at any age, but are most commonly seen in patients 40 to 60-years-old.2 A pyocele or mucopyocele is an infected mucocele, which can lead to orbital abscess, meningitis or cavernous sinus thrombosis.3Depending on the location, symptoms of mucoceles can be rhinologic, neurologic or ophthalmologic.1 Patients will often present with periorbital pain and headache. If the globe becomes displaced, patients will also complain of diplopia. Clinical findings generally include proptosis, restricted extraocular motilities and periorbital swelling. Exophthalmometry is useful in measuring the degree of proptosis. Forced duction testing can help differentiate between a neurogenic or restrictive process, but is often unnecessary in these cases. The presence of proptosis and resistance to retropulsion as seen in our patient is strong evidence of a compressive and restrictive mass. Sphenoid and ethmoid mucoceles can cause divisional oculomotor palsies, and posterior ethmoid and sphenoid mucoceles can cause direct optic nerve compression, causing vision loss and optic atrophy.2,4,5 Sinus mucoceles are best observed with MRI and CT imaging, and often both are indicated prior to surgery. MRI allows for better visualization of the mass along with its intracranial and intraorbital extension, while CT allows for better visualization of bone destruction.6
Mucocele appearance on MRI can vary depending on their contents. For example, bright signal intensity on T2-weighted images correlates with increased water content while low signal intensity on T2-weighted images correlates with inspissated mucus.6 This variability can make it difficult to distinguish a mucocele from a neoplastic process.
The preferred treatment of frontal sinus mucoceles is drainage via endoscopic sinus surgery, which is minimally invasive and yields excellent clinical outcomes.2
|
1. Capra GG, Carbone PN, Mullin DP. Paranasal Sinus Mucocele. Head Neck Pathol. 2012 Sep; 6(3):369-72. 2. Aggarwal SK, Bhavana K, Keshri A, et al. Frontal sinus mucocele with orbital complications: management by varied surgical approaches. Asian J Neurosurg. 2012 Jul-Sep; 7(3):135-40. 3. Rajan K, Santhi T. Frontoethmoidal mucocele with orbital and intracranial extension. Indian J Otolaryngol Head Neck Surg. 2007 Dec;59(4):363-5. 4. Gupta AK, Menon V, Sharma P, et al. A sphenoid sinus mucocele simulating as retro bulbar optic neuritis. Indian J Ophthalmol. 2012 May-Jun;60(3):216-18. 5. Kim DW, Sohn HY, Jeon SY et al. Ethmoidal mucocele presenting as oculomotor nerve paralysis. Clin Exp Otorhinolaryngol. 2013 Jun;6(2):103–6. 6. Tassel PV, Lee YY, Jing BS, De Pena CA. Mucoceles of the paranasal sinuses: MR imaging with CT correlation. AJR Am J Roentgenol. 1989 Aug;153(2):407-12. Accessed Nov 2015. www.cancer.gov/about-cancer/causes-prevention/risk/alcohol/alcohol-fact-sheet. |

