History

Her systemic history was significant for hypertension and a cerebralvascular accident, for which she was properly medicated. The stoke had mildly paralyzed the right side of her body.
Her ocular history was significant for cataracts.
Diagnostic Data
Her best-corrected visual acuity measured 20/40 O.U. at distance and near. External examination was normal, with no evidence of afferent pupillary defect or visual field involvement.
The pertinent anterior segment findings are illustrated in the photograph.
Intraocular pressure measured 14mm Hg O.U. Dilated fundoscopy was within normal limits in both eyes.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis?
How would you manage this patient? What’s the likely prognosis?
Discussion
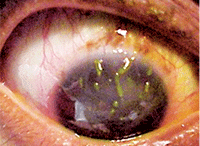
This 57-year-old patient with a history
of hypertension and cerebralvascular
accident presented with pain,
photophobia and lacrimation.
Additional patient examination should include: a Schirmer tear test to evaluate tear volume; tear quality testing; sodium fluorescein, lissamine green and rose bengal dye tests to confirm and grade the corneal and conjunctival epitheliopathy; eyelid strength testing and blink analysis to rule lagophthalmos and cranial nerve VII palsy; additional history to rule medications that are capable of causing dry eye and systemic laboratory investigations to rule out systemic etiologies.
The diagnosis in this issue is dry eye secondary to incomplete eyelid closure, poor tear spread and reduced tear quality, which resulted in filamentary keratopathy in the patient's right eye.
Many collagen vascular diseases can result in unilateral or bilateral dry eye and/or noninfectious peripheral corneal inflammation. Rheumatoid arthritis and secondary Sjögren's syndrome probably are the most common systemic causes of dry eye. Other differential diagnoses of dry eye include poor lid-to-globe congruity and poor lid closure secondary to CN VII palsy, dry eye secondary to radiation or chemical exposure, severe atopic keratoconjunctivitis, scleroderma, erythema multiforme, trachoma, Beçhet’s disease and sarcoidosis. Various medications, such as systemic birth control pills, practolol, topical epinephrine, idoxuridine, echothiophate iodide, pilocarpine, timolol and dipivefrin have also been implicated.1-4
The combination of punctate epithelial keratitis and increased mucus often leads to the development of filamentary keratitis.4-14 One common treatment for tenacious mucus deposition—which adheres to the superior eyelid cobblestones or the cornea as thick, ropy strands—or filamentary keratitis is a preparation known as acetylcysteine.4-6 This medication is known to break the disulfide bonds, thereby dissolving the mucus, and is effective for all three types of excessive mucus. It is formulated from commercially available Mucomyst (Bristol-Myers Squibb) that is diluted to a 5% or 10% solution with artificial tears and is applied q.i.d.4-6
Another mainstay treatment is the use of ocular surface lubricants—artificial tears and/or ointments—or pressure patches to improve patient comfort and perhaps reduce the frictional effects of eyelid blinking. Another option is the use of hypertonic sodium chloride either as a solution (three to four times a day) or as an ointment (once at bedtime). Depending upon the patient's symptoms or severity of injury, you can prescribe antimicrobial prophylaxis and cycloplegics. Finally, behavioral modification and conscientious training may help such patients learn to open their eyes more slowly upon waking.4-6
In cases of bigger erosions with loose sheets of epithelium, scraping and debridement—either with a Weck-Cel cellulose sponge, Kimura Spatula or soaked cotton-tipped applicator—may help induce efficient healing.4-6 Extended-wear bandage soft contact lenses may provide comfort and support the healing process with minimal compromise of vision.9 Additionally, they protect and isolate the fragile, healing epithelium from the windshield-wiper effects of blinking eyelids.9,10 These lenses should remain on the cornea for at least six to eight weeks to afford the basement membrane and hemidesmosomes sufficient time to reorganize. An alternative for short-term relief and epithelial support is a collagen shield.11 Oral acetominophen and ibuprofen can provide adequate analgesia.
If the erosions are severe or frequent, anterior stromal micropuncture or laser superficial keratectomy are therapeutic options.12
If scarring does not occur naturally, punctal occlusion with plugs or cautery may be performed to increase the lacrimal lake. Any blepharitis may be controlled with regular lid scrubs and antibiotic drops or ointments. If all else fails, mucous membrane grafts can be used to replace irreparably scarred conjunctivae. Systemic immunosuppressive therapies (such as cyclosporin, cyclophosphamide, azathioprine or corticosteroids) could also be regarded as a potential treatment option.16
Our patient was treated with debridement of the filaments (anesthetized, with each filament removed via forceps) and then medicated with topical antibiotic drops q.i.d. during the day and supported with an ointment antibiotic at night. A contact lens with lubrication drop solution normally would have been considered, but the patient was still in the critical care unit. The condition resolved well, without incident. Following complete corneal epithelial recovery, the patient was placed on NaCL ointment at bedtime to provide lubrication for the cornea, eliminate the risk of morning recurrent erosion and maintain appropriate corneal hydration. The patient has done well on this regimen for more than three years.13,14
1. Tavares Fde P, Fernandes RS, Bernardes TF, et al. Dry eye disease. Semin Ophthalmol. 2010;25(3):84-93.
2. Jackson WB. Management of dysfunctional tear syndrome: a Canadian consensus. Can J Ophthalmol. 2009;44(4):385-94.
3. Gayton JL. Etiology, prevalence, and treatment of dry eye disease. Clin Ophthalmol. 2009;3(7):405-12.
4. Filamentary keratopathy. In: Anterior Eye Disease and Therapeutics A-Z. Bruce AS, Loughnan, MS (eds.). Butterworth-Heinemann: Philadelphia; 2003:128-9.
5. Diller R, Sant S. A case report and review of filamentary keratitis. Optometry 2005;76(1):30-6.
6. Albietz J, Sanfilippo P, Troutbeck R, Lenton LM. Management of filamentary keratitis associated with aqueous-deficient dry eye. Optom Vis Sci. 2003;80(6):420-30.
7. Pons ME, Rosenberg SE. Filamentary keratitis occurring after strabismus surgery. J AAPOS. 2004;8(2):190-1.
8. Kakizaki H, Zako M, Mito H, Iwaki M. Filamentary keratitis improved by blepharoptosis surgery: two cases. Acta Ophthalmol Scand. 2003;81(6):669-71.
9. Kanpolat A, Uçakhan OO. Therapeutic use of Focus Night & Day contact lenses. Cornea. 2003;22(8):726-34.
10. Cher I. Blink-related microtrauma: when the ocular surface harms itself. Clin Experiment Ophthalmol. 2003;31(3):183-90.
11. Hadassah J, Prakash D, Sehgal PK, et al. Clinical evaluation of succinylated collagen bandage lenses for ophthalmic applications. Ophthalmic Res. 2008;40(5):257-66.
12. Tsai TY, Tsai TH, Hu FR, et al. Recurrent corneal erosions treated with anterior stromal puncture by neodymium: yttrium-aluminum-garnet laser. Ophthalmology. 2009;116(7):1296-300.
13. Grinbaum A, Yassur I, Avni I. The beneficial effect of diclofenac sodium in the treatment of filamentary keratitis. Arch Ophthalmol. 2001;119(6):926-7.
14. Avisar R, Robinson A, Appel I, et al. Diclofenac sodium, 0.1% (Voltaren Ophtha), versus sodium chloride, 5%, in the treatment of filamentary keratitis. Cornea. 2000;19(2):145-7.
15. Dua HS , Azuara-Blanco A . Autologous limbal transplantation in patients with unilateral corneal stem cell deficiency. Br J Ophthalmol. 2000;84(3):273-8.
16. Tatlipinar S. Akpek EK. Topical cyclosporine in the treatment of ocular surface disorders. Br J Ophthalmol 2005;89(10):1363-7.

