So, you have caviar and champagne tastes when it comes to your practice technology wish list, but, unfortunately, your financial reality is more in line with a hamburger and diet soda budget.
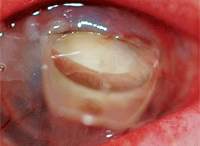
Keep in mind that gross
ophthalmic findings can be easily photographed but won’t always provide
great detail, such as this image of an intraocular lens protruding from
an elderly patient’s cornea, which was captured with an iPhone.
Not to worry!
If you can’t afford the latest and greatest technologies on the market, there are less expensive options available that will allow you to monitor, photograph and even diagnose patients while managing your practice investments on a limited budget.
“There are many diseases that can easily be monitored with a digital camera and attachments to your standard slit lamp,” says optometrist Jason Miller, M.B.A., of Powell, Ohio. “With today’s business economy and the increased costs of many ophthalmic instruments, it is important to evaluate less expensive equipment options as a viable alternative. This evaluation will be considered with increasing importance as health care reform begins to take shape."
Of course, you should keep in mind that some of the more advanced, higher-priced technologies will provide more options, greater detail and improved user-friendliness. However, take heart. If you are a budget-conscious optometrist, viable alternatives are still out there.
Frugal Anterior Segment Photography
Digital photography can get pricey. However, there are budget-friendly options, if you know how to find them.
“Quality images do not have to be expensive. Certainly, anterior segment photos can be done with an inexpensive digital camera through the slit lamp ocular,” says optometrist Christine Sindt, O.D., Director of Contact Lens Services at the University of Iowa Hospitals and Clinics. A basic digital camera will cost in the ballpark of $150 to $300. More advanced cameras and software packages can cost several thousands of dollars.
Anterior ocular structures and diseases can be diagnosed and/or monitored with a high quality digital camera with or without a slit lamp adapter, Dr. Miller adds. These conditions include most eyelid, conjunctival, corneal and iris pathologies. “For example, if a new patient presents with a corneal ulcer scar near the pupil, it would be important to document this condition, especially if the patient is a chronic abuser of contact lenses,” he says. “This photo-documentation can be used to educate the patient on future damage if the abuse continues. But, if the condition is microscopic in nature or in the posterior chamber of the eye, it may be difficult to obtain quality photos without a stabilizing adapter or a better system.”
Several slit lamp adapters are available at a reasonable cost, generally starting at approximately $400 and up. Some slit lamp manufacturers make adapters for their systems that are electronically compatible, and can capture images with just a touch of a button. These can run in the ballpark of around $5,000.
“I have been able to monitor neovascularization, corneal abrasion and keratitis this way,” says optometrist Michael Mayers, of Powell, Ohio. “Very fine neovascularization is difficult to capture, but I have monitored corneal infiltrates and punctate keratits with my digital slit lamp mounted camera.”
If you do decide to purchase a digital camera and/or slit lamp adapter, Dr. Mayers offers some tips on best usage for optimum photographs:
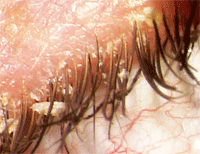
A patient with advanced anterior blepharitis, captured with an anterior segment camera mounted on a slit lamp.
• First, use the manual mode to control the settings on the digital camera.
• Be sure to talk to the vendor to get detailed information on best usage. “They have lots of knowledge about aperture speed and exposure setting,” he adds.
•Avoid direct lighting. “What I can tell you from experience is that direct lighting always washes out the image you want to capture, so you always want diffuse lighting adjacent to the image or diffuse lighting across the entire surface,” Dr. Mayers says.
Limitations
Of course, anterior segment images captured with a simple digital camera or with the help of a slit lamp adapter do have drawbacks.
“Essentially, (with the slit lamp adapter) you are taking two completely different systems and incorporating them together,” Dr. Mayers says. “You can get good pictures, and you can bill for them as long as you include the medically necessary reason for the ophthalmologic testing and interpretation in the report. But if you use a higher-end piece of equipment, you can get a superior quality picture because the company packages it all together and optimizes the slit lamp controls, digital camera, and ocular optics for digital photography,” he adds.
Practice management consultant and optometrist Gary Gerber cautions, “The CPT codes do not specify the exact extent of the technology to be used. For example, they don’t specify things like the number of pixels needed in a photograph or how the resolution should be on your viewing monitor.”
Gross ophthalmic findings can be easily photographed but won’t provide great detail, adds Joseph P. Shovlin, O.D., of Scranton, Pa. “For the detail needed to follow some corneal and retinal conditions, much more elaborate hardware and software features are required. Unfortunately there is no substitute for the real thing, and that requires some cash.”
And, of course, less expensive options pose more difficulty in taking high quality photographs of posterior structures within the eye, Dr. Miller adds.
Investing in Retinal Photography
If you are in a glaucoma specialty practice, your budget options are more limited. “Monitoring glaucoma progression is a different situation,” Dr. Miller says. “There is software available that can easily track for progression over a series of images. This analysis is much more precise than the human eye in detecting progression. It requires high- quality images and image aligning software to detect the smallest of changes. Early detection and treatment is critical to preventing visual field loss in glaucoma patients. When developing a strong glaucoma treatment center, high quality equipment is critical to good outcomes.”
However, proven methods for photographing and monitoring your glaucoma patients should be first on the list—before you decide to purchase a more high- tech (and more expensive) piece of equipment, experts advise.
“Photography is an integral part of an eye care practice, and the first image device before an HRT, OCT or GDX needs to be a retinal camera,” says optometrist James L. Fanelli, of Cape Fear Eye Institute, of Wilmington, N.C.
True, a retinal camera costs in the ballpark of $19,000 to $24,000, but it can provide an excellent means of monitoring diseases of the optic nerve and retina.
“Studies have shown validity of HRT and OCT, (but) a good majority of diseases, including glaucoma, can be followed very nicely with good stereo optic nerve photographs,” Dr. Fanelli says. “Fundus and optic nerve photography is a tried-and-true technology, especially for a first-time investment.”
For glaucoma, baseline stereo photography can monitor the optic nerve over time, when combined with subsequent stereo images. In addition, a myriad of retinal conditions, such as disc swelling, retinal vascular disorders, hypertensive retinopathy, macular disease and wet and or dry age-related macular degeneration can be followed with retinal photography.
“You generally get what you pay for,” Dr. Gerber says. “There’s a reason a $23,000 retinal camera costs that much. The images are genuinely sharper than you’d get by setting up a Rube Goldberg contraption with your iPhone.”

Many anterior segment conditions can be photographed while on a budget, such as this photo of tarsal plate papillae, taken with a digital slit lamp-mounted camera by Michael Mayers, O.D.
Additionally, the software you might use to view the images probably won’t be as robust and won’t integrate well, if at all, with your EMR (electronic medical records) system, Dr. Gerber adds. “From a marketing and practice building perspective, there is certainly something to be said for using, for example, a retinal camera instead of a camera your patient might be able to buy at Radio Shack, or worse, have in their own pocket during their exam.”
Of course, a retinal camera can’t do it all. A basic retinal camera’s biggest drawback is lack of quantification of nerve tissue volume or retinal thickness, Dr. Fanelli says. More expensive optic nerve imaging devices, such as the HRT-3 (Heidelberg Engineering), actually quantify images, and with image registration, subsequent scans can be done in the same location, he says.
Fundus Camera Alternatives
If you aren’t prepared to purchase a fundus camera yet, there are alternatives. If a patient needs a fundus photo, consider partnering with a local ophthalmologist. The ophthalmologist can take the photo and manage the technical component of the billing, while you can handle the interpretation fee, Dr. Mayers suggests.
Alternatively, you could share the equipment—and the cost—with another optometric practice in your area.
An additional option is considering adding the Optomap (Optos) to your practice. “With the Optomap, there is no up front investment. You pay on an ongoing basis for use, but it’s not a big investment to get started,” says Jeffry Gerson, O.D., of WestGlen Eyecare and Omni Eye Center of Kansas City. The Optomap provides a much wider view of the retina and aims to reveal important information for the comprehensive evaluation of systemic and ocular health. It also creates more potential for medical billing as well, he adds.
Dr. Gerson had originally planned to eventually purchase a fundus camera, but he decided not to after four years of exceptional use of retinal imaginge with the Optomap, he says.
Traditional Visual Field Testing VS. HRT
Visual field testing is a standard in a glaucoma practice. However, a glaucoma patient’s subtle changes on a traditional white-on- white visual field test generally will not show up for up to five years, whereas more sophisticated scanning can predict these subtle optic nerve changes more quickly. Therefore, imaging has become the standard of care, experts say.
“In a true glaucoma practice, you need both pieces of equipment—visual field testing and an optic nerve imaging device,” says optometrist Robert Cole, of Bridgeton, N.J. “Visual fields have been a standard of care, and scanning instruments are fast becoming a standard of care. Even for a young practitioner on a limited budget, it would behoove them to have it.”
Dr. Cole suggests two options for O.D.s on a limited budget:
1. Shop around for a used optic nerve imaging device.
2. Consider sharing the cost and usage of a more expensive piece of equipment with another practice.
“Some of the equipment today is portable—and it can move from one office to the other,” Dr. Cole says. “You can block off scheduled times when one office has the equipment.”
The disadvantage of this alternative: The optometrist would need to make hard copies of images, because the data is stored directly in the instrument. For those who do purchase or lease an optic nerve imaging device exclusively, images can be viewed directly at any time, which is a plus.
Leasing Options
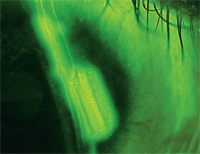
This photo was taken with an anterior segment camera mounted on a slit lamp, which captures a corneal abrasion.
For the optometrists on a limited budget: don’t forget about leasing options if you determine your practice can sustain adding a more expensive, high tech piece of equipment.
The first step: Look at your practice, and determine if you can afford the monthly payment. “Everyone wants, for example, an OCT,” says Dr. Gerson. “But, if you don’t have the population to afford it, it may not be the right piece of equipment for your practice. You need to analyze your practice and make sure you have enough the volume to support this technology.”
Careful analysis may show that the practice does have a fair amount of patients who could benefit from a specific technology, which would warrant the investment.
Secondly, if you do get the technology, don’t be afraid to use it, Dr. Gerson adds. “If you do have a piece of equipment, you will probably use it more than you think. For example, you may have a patient with a borderline pathology. You figure you could monitor this on your own. If you do have the equipment, you can tell the patient ‘I have this test that is easy to use and that I think would benefit you.’ Essentially, if you do have the equipment, take advantage of what you have.”
Another piece of advice if you do decide to lease: Plan in advance.
“Keep a list, in advance, of patients who need the technology you’re considering buying,” says Dr. Gerber. “Once you buy it, call up your back-log list of patients and use it right away on those patients. Of course, this assumes those patients you keep waiting do not have a time-sensitive urgent condition requiring immediate attention,” Dr. Gerber says. “Also, interest rates for loans or leases are still very low, making most technology quite affordable.”
Bottom Line
Many options exist that will allow you to get the technology you need at a price you can afford.
No matter if you find yourself on a limited budget, remember, whether it’s leasing, monitoring anterior segment conditions with a digital camera or considering buying used equipment, several low-cost options are out there for you to provide high-quality patient care.

