Advanced imaging technologies are showing that corneal ectasias such as keratoconus are more prevalent than previously thought—up to 265 cases per 100,000 people.1 Those with family history, eye rubbing and atopy, as well as Down syndrome tend to be more commonly affected, and are typically diagnosed during puberty.2 Acute corneal hydrops—a severe complication of corneal ectasia—occurs in as few as 2%, and up to 13%, of patients.3-5
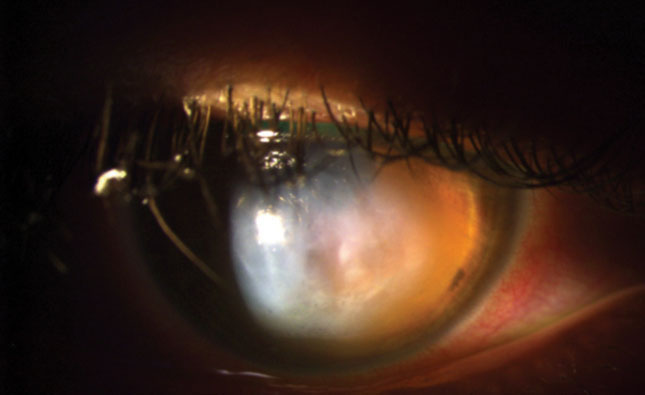 |
Fig. 1. This patient’s right eye shows grade 3+ global conjunctival injection, grade 3+ corneal edema, trace micro bullae and epithelial defects. |
History
A 40-year-old African-American male presented with sudden-onset pain in the right eye for the last two days, and associated blurry vision. He rated the pain an “eight out of 10” in severity. He also complained of redness and photophobia but denied any discharge, history of ocular surgery, foreign material entering the eye or trauma. This was the first occurrence of these symptoms. The patient attempted to use artificial tears without relief. His ocular his-tory was significant, however, for keratoconus, for which he was prescribed scleral lenses.
Examination
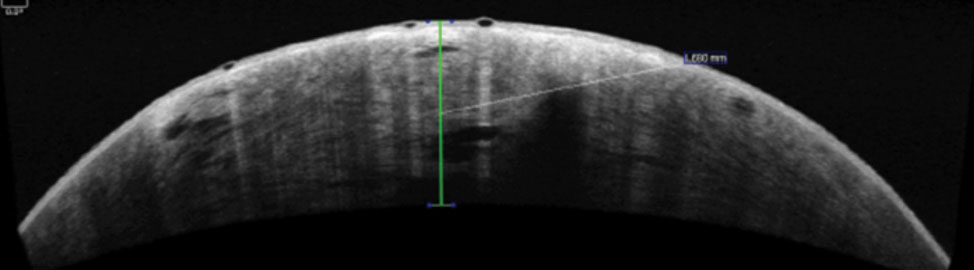
The patient’s entering uncorrected visual acuity was 20/800 at one foot in the right eye, with mild improvement on pinhole to 20/400 at two feet. Corrected visual acuity in the left eye with the scleral lens was 20/20. An external examination revealed an area of corneal opacification in the right eye, causing pupil testing to be difficult. The left pupil was round, reactive and had no signs of an afferent pupillary defect. Confrontation visual fields were full to hand motion in the right eye and full to finger counting in the left eye. Extraocular muscle testing was normal. Biomicroscopy of the right eye revealed grade 3+ global con-junctival injection, grade 3+ corneal edema, trace micro bullae and epi-thelial defects (Figure 1). Intraocular pressure was normotensive and dilated fundus exam was unremarkable. An anterior segment OCT was performed revealing a break in Descemet’s membrane and corneal edema (Figure 2).
 |
Fig. 2. This anterior segment OCT shows a break in the patient’s Descemet’s membrane and corneal edema. |
Diagnosis
Corneal hydrops is caused by split-ting of Descemet’s membrane, leading to an influx of aqueous into the corneal stroma with resultant edema and haze.6 Depending on the patient and the extent of the tear, corneal edema and pain can range from relatively asymptomatic to severe with visual impairment.4,6 Corneal hydrops is more common in males between the ages of 20 and 40, but has no race predilection.3-6
Acute corneal hydrops is self-limiting, with or without treatment, and tends to resolve over the course of three to four months as Descemet’s membrane re-seals.3 Depending on the size of the break and the patient’s risk of corneal infection or neovascularization, time to complete healing may be extended.3,4,6 Corneal perforation, although rare, occurs in 3% of patients who develop hydrops.3 To prevent secondary complications, minimize patient symptoms and limit corneal scarring, initiation of medical management is typically warranted.
Treatments
A variety of medical and surgical options are available to treat corneal hydrops. Topical hyperosmotics, can reduce corneal edema (albeit slowly), and improve acuity. To further manage corneal edema while also reducing the risk for potential neo-vascularization, ODs can prescribe topical steroids—usually starting with a twice-daily dose.
Since steroids have the potential to hinder corneal healing or cause corneal perforation, initiating steroid treatment at onset, or even once Descemet’s membrane heals, is controversial. A cycloplegic agent, typically dosed at twice per day (more if pain persists), can be added to reduce ocular pain from a secondary uveitis. Other options for pain relief include oral or topi-cal nonsteroidal anti-inflammatory agents or a bandage contact lens. However, depending on the severity of the patient’s keratoconus the lens may fail to fit appropriately with significant edge fluting and decentration. As long as epithelial defects are present, a prophylactic antibiotic should be prescribed to decrease the potential for infection.
Research shows oral doxycycline (10mg to 50mg twice per day) and vitamin C (1,000mg per day)—typically dosed early in the course of acute hydrops—can be beneficial.7,8 Doxycycline may also reduce matrix metalloproteinases, which promotes corneal healing.8 Vitamin C has a role in the extracellular matrix and corneal composition, and can decrease opacification and neovascularization.7 Other options to enhance corneal healing include amniotic membrane transplants and copious preservative-free artificial tears.
Surgical interventions include injection of air or gas, sulfur hexafluoride (SF6) or perfluoropropane (C3F8), into the anterior chamber to mechanically close the opening in Descemet’s membrane.9,10 These improve healing time but do not impact visual acuity outcomes, making them controversial due to potential adverse events.9,10 For maximum effect, these procedures must be per-formed typically within days after the initial onset of symptoms.9,10
 |
| Fig 3. This image shows the patient’s corneal thickness three weeks after treatment. It had thinned by approximately 400µm. |
Recovery
The longer the hydrops takes to heal, the more likely a transplant will be required, due to residual scarring. If this scar is large, or directly on the visual axis, either a deep anterior lamellar kerato-plasty or a penetrating keratoplasty may be performed, depending on the extent of the scarring.3 Some surgeons advocate for earlier intervention before any corneal neovascularization occurs, to decrease the risk of transplant rejection. Prior to any surgical referral, attempting a gas permeable contact lens fitting will allow for assessment of best visual acuity and can delay surgery, if the patient can achieve functional vision.
In our patient’s case, we prescribed a hyperosmotic ointment, cycloplegic and antibiotic, along with oral doxycycline and vitamin C. Within three weeks, his corneal thickness was thinner by approximately 400µm (Figure 3). Although standard pachymetry can be helpful to monitor for resolution, ‘global’ pachymetry or AS-OCT are more beneficial as a larger area of the cornea can be imaged and healing of Descemet’s membrane can be visualized. Patients with acute corneal hydrops should be monitored every two to three days after initial onset, followed by every one to two weeks once healing has begun. However, if the cornea appears significantly thinned, more frequent follow-up is prudent to prevent perforation. Use of a fox shield is recommended. Once healed, these patients should follow-up every three months for repeat imaging.
Practitioners should strive to minimize patient symptoms and avoid devastating long-term com-plications with appropriate medical management. Diagnostic imaging equipment can be helpful not only with initial diagnosis, but also in monitoring resolution. While corneal hydrops is rare, advances in detection and treatments of kera-toconus, with corneal crosslinking may reduce or eliminate it in the future.
Dr. Morrow is an assistant clinical professor at the State University of New York College of Optometry.
| 1. Godefrooij D, de Wit G, Uiterwaal C, et al. Age-specific incidence and prevalence of keratoconus: a nationwide regis-tration study. Am J Ophthalmol. 2017;175(3):169-72. 2. Gokhale N. Epidemiology of Keratoconus. Indian J Oph-thalmol. 2013;61(8):382-3. 3. Barsam A, Petrushlin H, Brennan M, et al. Acute corneal hydrops in keratoconus: a national prospective study of inci-dence and management. Eye (Lond). 2015;29(4):469-74. 4. Gokul A, Krishnan T, Emanuel P, et al. Persisting extreme acute corneal hydrops with a giant intrastromal cleft secondary to keratoconus. Clin Exp Optom. 2015;98(5):483-6. 5. Thimons J. Managing acute corneal hydrops in keratoconus. Rev Cornea & Cont Lens. 2015;152(3):32-3. 6. Fuentes E, Sandali O, El Sanharawi M, et al. Anatomic predictive factors of acute corneal hydrops in keratoconus: an optical coherence tomography study. Ophthalmol. 2015;122(8):1653-9. 7. Cho Y, Yoo W, Kim S, et al. Efficacy of systemic vitamin c supplementation in reducing corneal opacity resulting from infectious keratitis. Medicine (Balt). 2014;93(23):1-8. 8. Perry H, Hodes L, Seedor J, et al. Effect of doxycycline hyclate on corneal epithelial wound healing in the rabbit alkali burn model. Cornea. 1993;12(5):379-82. 9. Maharana P, Sharma N, Vajpayee R. Acute corneal hydrops in keratoconus. Indian J Ophthalmol. 2013;61(8):461-4. 10. Shaw J. Acute hydrops: rethinking treatment. EyeNet Magazine. www.aao.org/eyenet/article/acute-hydrops-rethinking-treatment. June 2012. Accessed October 15, 2018. |

