 History
History
A 58-year-old black female presented for an ocular health evaluation with a chief complaint of difficulty reading. Her ocular history was noncontributory.
Her systemic history was remarkable for hypertension, for which she was compliant and properly medicated. She reported no known allergies.
Diagnostic Data
Her best-uncorrected visual acuity measured 20/25 OU at distance and near. Her external examination was within normal limits, and she exhibited no afferent pupillary defect.
Her anterior segment examination was normal OU. Intraocular pressure measured 14mm Hg OU. The dilated fundus examination also was within normal limits, with quiet grounds, normal posterior poles and distinct optic nerves. Her cup-to-disc ratio appeared to be 0.2 x 0.2.
The significant external observation is illustrated in the photograph.
Your Diagnosis
How would you approach this case? Does the patient require any additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Discussion
Further evaluation included additional patient history regarding systemic health maintenance and baseline fundus photography.
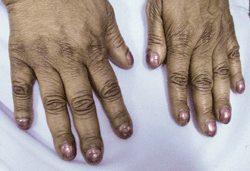
External inspection of our 58-year-old patient uncovered this finding. What is it?
The diagnosis in this case is clubbing of the fingers. This presentation is an observable physical finding that can be measured by the profile angle of the individual’s hand or by distal phalangeal-to-interphalangeal depth ratio.1 Most microscopic and imaging studies of clubbed fingers reveal hypervascularization of the distal digits.1,2
Recent research has shown that when platelet precursors fail to become fragmented into platelets within the pulmonary circulation, they are easily trapped in the peripheral vasculature. This process releases platelet-derived growth factor and vascular endothelial growth factor––both promoters of vascularity and finger clubbing.1,2
Clinically, clubbing is associated with a number of neoplastic, pulmonary, cardiac, gastrointestinal, infectious, endocrine, psychiatric and multisystem diseases.1 All the conditions associated with digital clubbing share the common pathway of enhanced platelet/endothelial cell activation.1,2
Emerging evidence indicates that hypoxic conditions with extrapulmonary blood shunting prohibit large megakaryocyte fragments from entering the pulmonary circulation.2 Instead, they gain access to the systemic circulation––impacting distal body sites via growth factor release and vascularity proliferation.2
Further, in cases of lung cancer, these purported growth factors could gain direct entrance to the systemic circulation and yield a similar situation.2 So, a detailed history and physical examination accompanied by focused laboratory studies and imaging often can help determine the underlying cause.
We prescribed presbyopic spectacle correction to remedy the patient’s chief complaint of blurred near vision. Additionally, we informed her general medicine team of our findings. The team acknowledged the issue, and suggested that the search for an underlying cause was ongoing.
1. Spicknall KE, Zirwas MJ, English JC 3rd. Clubbing: an update on diagnosis, differential diagnosis, pathophysiology, and clinical relevance. J Am Acad Dermatol. 2005 Jun;52(6):1020-8.
2. Martinez-Lavin M. Exploring the cause of the most ancient clinical sign of medicine: finger clubbing. Semin Arthritis Rheum. 2007 Jun;36(6):380-5.

