 |
 |
Fungal keratitis is perhaps one of the most feared ocular conditions. This fear is justified when you consider that fungal keratitis is difficult to diagnose, treatment options are limited and poor outcomes are common. Here, well review the risk factors, diagnosis and management of this condition.
Risk Factors
Fungal keratitis shows no predilection for age, gender or race.1 Risk factors include ocular trauma, (particularly if the patient was injured by a tree branch or other organic vegetative matter) pre-existing ocular or systemic immunosuppressive diseases and topical steroid therapy.1-4 Fungal infections are more common in agricultural and tropical environments than in other locations.3 Patients who have an altered epithelial barrier are at an increased risk of fungal infection regardless of geographic location.
There are two types of fungi: molds (filamentary fungi) and yeasts. Molds are subdivided into septate and non-septate organisms. Septate organisms are the most common cause of fungal keratitis.
Yeasts are non-septate filamentary organisms. They are more commonly responsible for orbital disease.
Most fungal infections of the cor-nea are caused by Fusarium and Aspergillus (filamentary fungi) or Candida (a yeast).1,2,4-6
Clinical Presentation
Filamentary fungal infections of the cornea initially produce a feathery, branching pattern. The cornea appears a dull-gray with possible heaping of the epithelium and a dry, rough texture. Severe anterior uveitis, plasmoid aqueous and hypopyon often accompany the corneal findings.
But, the characteristic corneal appearance eventually disappears, making fungal keratitis resemble advanced bacterial keratitis. (There is no documentation of how long this process takes, but based on our own observations, we believe this conversion occurs within two to three weeks). Once this happens, there is a greater chance of misdiagnosis.
Diagnosis
Some clinicians only suspect fungal keratitis when presumed bacterial keratitis worsens during antibiotic therapy.
The standard corneal scraping used to diagnose bacterial keratitis is acceptable for culturing fungal infections as well. This includes regular cultures with blood and chocolate agar incubated at 37 C to check for bacteria. Also, blood and Sabouraud agar plates should be inoculated and kept at room temperature when you suspect fungal keratitis.
It is widely known that antifungal sensitivity testing is unreliable and correlates poorly with clinical efficacy. So, a corneal biopsy may be needed. Recently, confocal microscopy has been shown to be an accurate, non-invasive method for identifying fungal keratitis.7
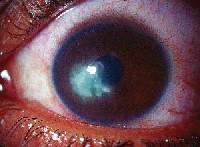 |
| Fungal keratitis may masquerade as bacterial keratitis. |
Management
Treating fungal keratitis is difficult. Most antifungal medications are merely fungistatic; that is, they inhibit the growth of fungi. These agents require an intact immune system and a prolonged therapeutic course.
Drug classes used to treat fungal keratitis include polyene antibiotics (e.g., nystatin, natamycin and amphotericin B,); pyrimidine analogs (e.g., flucytosine); imidazoles (e.g., clotrimazole, miconazole, econazole and ketoconazole); triazoles (e.g., voriconazole, fluconazole and itraconazole); and silver sulfadiazine. Natamycin can only be given topically, while the other antifungal drugs can be given both systemically and topically.4 Steroids are contraindicated, as they will exacerbate the disease.
One study recommends Natacyn (natamycin 5%, Alcon) as the first choice for treating filamentary fungal infections.8 Alternatives include amphotericin B 0.15% and flucytosine 1% 150 mg/kg. Natacyn, amphotericin B and flucytosine are also used for ocular yeast infections.
An alternative treatment for ocular yeast infections: fluconazole 0.5% 200mg or miconazole 1%. New research, however, suggests that voriconazole may be more effective than amphotericin B in treating Candida albicans keratitis.9 The study, done on 44 rabbits, revealed that in the initial homogenized samples, only those given voriconazole had significantly reduced colony-forming units compared to the control group. Also, the rabbits that received amphotericin B experienced significant increases in mucus discharge and conjunctival hyperemia when compared to the other groups, including rabbits who received fluconazole, another antifungal agent.
Itraconazole, given topically or systemically, is effective in treating fungal keratitis, particularly if the infections are due to Aspergillus or Curvularia species.8,10 Recent studies have shown that econazole 2% appears to be as effective as Natacyn for the management of fungal keratitis.11 However, the combined use of econazole and Natacyn do not seem to have any advantage over that of Natacyn alone.12
Regardless of which therapy you choose, patients should use their medication hourly around the clock. The length of treatment depends on the severity of the fungal keratitis. Also, be sure to monitor the patient for ophthalmic toxicity.
Treatment of fungal keratitis with medical therapy alone often leads to poor outcomes, necessitating surgery to affect a clinical cure.13,14 One study examined the efficacy of phototherapeutic keratectomy (PTK) in patients whose superficial fungal keratitis had infiltrated less than half the corneal thickness and responded poorly to topical antifungal therapy. Results showed that PTK shortened treatment time, hastened re-epithelialization and restored reasonably good vision (the average visual improvement was 2.9 2.1 lines).15
Although fungal keratitis is not exceedingly common, we must remain aware of its risk factors, clinical presentation and management, so we can promptly and aggressively eradicate this fungus among us.
Both Drs. Sowka and Kabat are members of Alcons speakers bureau, but do not have any financial interests in the products mentioned.
1. Hofling-Lima AL, Forseto A, Duprat JP, et al. Laboratory study of the mycotic infectious eye diseases and factors associated with keratitis. Arq Bras Oftalmol 2005 Jan-Feb;68(1):21-7. Epub 2005 Mar 30.
2. Basak SK, Basak S, Mohanta A, Bhowmick A. Epidemiological and microbiological diagnosis of suppurative keratitis in Gangetic West Bengal, eastern India. Indian J Ophthalmol 2005 Mar;53(1):17-22.
3. Bharathi MJ, Ramakrishnan R, Vasu S, et al. Epidemiological characteristics and laboratory diagnosis of fungal keratitis. A three-year study. Indian J Ophthalmol 2003 Dec;51(4):315-21.
4. Thomas PA. Fungal infections of the cornea. Eye 2003 Nov;17(8):852-62.
5. Chowdhary A, Singh K. Spectrum of fungal keratitis in North India. Cornea 2005 Jan; 24(1):8-15.
6. Doczi I, Gyetvai T, Kredics L, Nagy E. Involvement of Fusarium spp. in fungal keratitis. Clin Microbiol Infect 2004 Sep;10(9):773-6.
7. Avunduk AM, Beuerman RW, Varnell ED, Kaufman HE. Confocal microscopy of Aspergillus fumigatus keratitis. Br J Ophthalmol 2003 Apr;87(4):409-10.
8. Kalavathy CM, Parmar P, Kaliamurthy J, et al. Comparison of topical itraconazole 1% with topical natamycin 5% for the treatment of filamentous fungal keratitis. Cornea 2005 May;24(4):449-52.
9. Botelho PJ, Zhang C, Kuo IC, et al. Comparative efficacy of topical voriconazole with amphotericin B and fluconazole in the treatment of Candida albicans keratitis in an animal model. ARVO Abstract No. 2623, 2005.
10. Agarwal PK, Roy P, Das A, et al. Efficacy of topical and systemic itraconazole as a broad-spectrum antifungal agent in mycotic corneal ulcer. A preliminary study. Indian J Ophthalmol 2001 Sep;49(3):173-6.
11. Prajna NV, John RK, Nirmalan PK, et al. A randomised clinical trial comparing 2% econazole and 5% natamycin for the treatment of fungal keratitis. Br J Ophthalmol 2003 Oct;87(10):1235-7.
12. Prajna NV, Nirmalan PK, Mahalakshmi R, et al. Concurrent use of 5% natamycin and 2% econazole for the management of fungal keratitis. Cornea 2004 Nov;23(8):793-6.
13. Fong CF, Tseng CH, Hu FR, et al. Clinical characteristics of microbial keratitis in a university hospital in Taiwan. Am J Ophthalmol 2004 Feb;137(2):329-36.
14. Doczi I, Gyetvai T, Kredics L, Nagy E. Involvement of Fusarium spp. in fungal keratitis. Clin Microbiol Infect 2004 Sep;10(9):773-6.
15. Lin CP, Chang CW, Su CY. Phototherapeutic keratectomy in treating keratomycosis. Cornea 2005 Apr;24(3):262-8.

