 |
History
A 27-year-old female presented to office urgently with a red, painful left eye of three days’ duration. The patient also complained of blurred vision and photophobia in the same eye. Her history was positive for extended soft contact lens wear. The patient explained that she regularly slept in lenses. She had no other ocular disease history and said that something like this had never happened before. She denied any exposure to trauma, had no systemic disease, took no medications and had no allergies.
Diagnostic Data
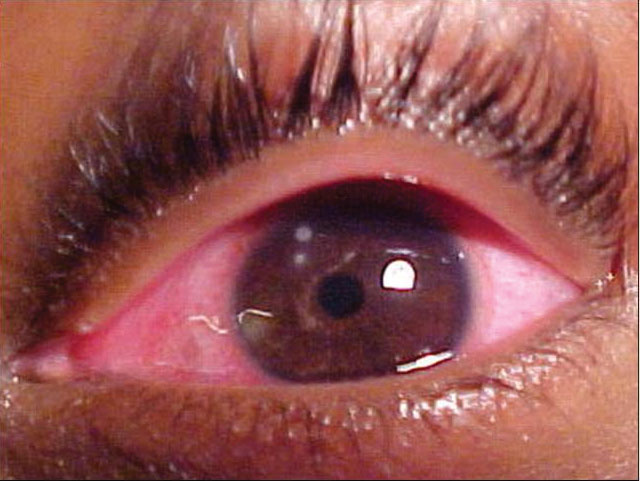
Using contact lenses, her best-corrected entering visual acuities were 20/20 OD and 20/40 OS, with improvement to 20/20 OS upon the pinhole. The external examination observation is demonstrated in the photograph. Her extraocular muscle motilities were normal and her confrontation visual fields were full. The patient’s color vision found no abnormalities using the red, green, blue and yellow cap screening test and no afferent pupillary defects were observed.
Given the urgent nature of the presentation, refraction was not completed on this visit. Biomicroscopy revealed tightly fitting, poorly moving soft contact lenses in both eyes. After the patient’s contact lenses were removed, the left eye demonstrated conjunctival injection of 360 degrees, corneal inflammation with diffuse punctate sodium fluorescein staining, an old circular corneal scar at 9 o’clock and two circular subepithelial inflammatory areas with mild overlying sodium fluorescein staining. Her intraocular pressures measured 17mm Hg OU by Goldmann applanation. The posterior segments demonstrated normal, round nerves exhibiting 30% cupping and normal posterior poles with no peripheral pathology.
 |
| This 67-year-old woman is blind in her left eye, but her family was concerned that the eye itself was shrinking. Can this external examination help explain her condition? Click image to enlarge. |
Additional Testing
Additional studies included:
- An examination of the lesions for foreign matter to rule out sequestered foreign body
- An examination of the anterior chamber to determine the level of iritis or iridocyclitis (and to ensure there was no evidence of a corneal puncture wound)
- An eyelid eversion to assess the physiologic relationship of the ocular tissues to the contact lens material
- Bacterial culturing with either a calcium alginate swab culturette or Kimora platinum spatula with plating on blood agar (general growth), chocolate agar (sexually transmitted diseases such as neisseria gonorrhea), thioglycolate media (anaerobic bacteria), sabouraud’s media (fungi) and non-nutrient agar with e. coli overlay (Acanthamoeba)
Diagnosis
The diagnosis in this case is sterile corneal ulceration secondary to contact lens associated acute red eye (CLAARE). The malady has also been referred to as “contact lens over wear” and “immobile lens syndrome.”1-5 As the name implies, this is an acute inflammatory condition associated with excessive, poorly fitting, usually dehydrated, tight-fitting contact lens wear.1-5 The literature also recognizes scleral lenses as a potential source.6 The classic presentation involves a patient in extended-wear hydrogel contact lenses who, upon awakening, experiences unilateral ocular pain (e.g., foreign body sensation), tearing, variably decreased vision and photophobia.
Clinically, CLAARE manifests as an acute corneal-mediated ocular inflammation marked by mid-peripheral subepithelial corneal infiltrates. These infiltrates may be seen to emanate from and accumulate near encroaching limbal vessels.
Associated clinical signs include moderate to severe conjunctival and limbal hyperemia, corneal edema and mild to moderate blepharospasm. Corneal epitheliopathy and anterior chamber reaction are variable depending upon the severity of the condition and the delay in presentation to the treating clinician. Although eyelid edema is typically absent, if the superior palpebral conjunctiva is inflamed or the condition has induced eye rubbing it may be present.6
Often, patients with CLAARE will have a history of poor contact lens hygiene, excessive wearing time or frank contact lens abuse.1-8 In some cases, the contact lens shows inadequate movement, and the patient may be physically unable to remove the lens from the eye during the initial episode.1-6 Immobility of the lens is, however, not uniformly encountered. CLAARE may occur with both well-fitted and poorly-fitted lenses and may be seen with low or high dK/L materials, including silicone hydrogels.7,8
Contact lens wear is a major risk factor for microbial keratitis and Fusarium and Acanthamoeba keratitis specifically.4 Even when lens wear is not abused, both ocular hygiene and maintenance of the contact lens case are major risk factors for a spectrum of eye complications, including microbial keratitis and other contact lens-related inflammations.4 The results of one analysis of the burden of contact lens complications in the United States showed that an estimated 930,000 doctor's office and outpatient clinic visits and 58,000 emergency department visits resulted secondary to contact lens related blepharokeratitis.4 An estimated 76.5% of these visits resulted in the prescribing of antimicrobial medications at a an estimated $175 million in direct health care expenditures ($58 million, Medicare/$12 million, Medicaid, per year).4 Office and outpatient clinic visits occupied more than 250,000 hours of clinician time annually.4
CLAARE represents a sterile inflammatory keratitis that is induced by, among other things, bacterial colonization of the contact lens.1-5 Gram-negative bacteria, particularly Pseudomonas but also Haemophilus and Serratia species, have been implicated.7 In CLAARE, these bacteria do not invade the cornea, but rather release endotoxins that recruit inflammatory cells. It may also represent an inflammatory response to an excessively tight fitting, immobile lens or stagnating tears.1-8
When the eye is open, under normal conditions, it receives its oxygen supply directly from the atmosphere. When the eye is closed or covered by a contact lens, oxygen is supplied to the anterior corneal surface via diffusion from the vascular capillary plexus of the upper palpebral conjunctiva as well as the tear layer. Contact lenses, hydrogels in particular, can reduce the amount of oxygen that reaches the anterior corneal surface. Contact lens movement, decay-accelerating factor (DAF-complement activation fragments which have been detected in the anterior segment during eye closure, contact lens wear and contact lens-associated pathologies), oxygen permeability of the contact lens itself, along with alteration due to poor care or long wear time, thickness profile and wearing schedule all influence corneal oxygen availability and physiology.1-10
The etiology of contact lens over wear syndrome remains controversial. Corneal hypoxia, toxins released by contaminants trapped underneath a stagnant lens during closed-eye wear and poor physiology secondary to tightening of the lens-base curve-cornea relationship or combinations, are all postulated as potential etiolopathiologies.1-10
Management
Clinical management begins with removal of the lenses and cessation of contact lens wear. Visual acuity, along with an evaluation of the pain response to extraocular muscle movement and light exposure will provide circumstantial clues regarding the degree of inflammation. Biomicroscopy of the cornea will uncover the presence of epithelial defects, corneal edema, subepithelial infiltration and anterior chamber involvement. Sodium fluorescein staining will expose areas of punctate epithelial compromise. All tissues should be inspected to rule out other sources of pathology that might require attention. Lids should be everted.
The initiation of a cycloplegic agent is recommended. The choice of homatropine 5% or atropine 1% is dictated by the severity of the presentation and the discomfort of the patient; cyclopentolate 1% and 2% and even tropicamide 1% work well in mild cases.15 If significant corneal staining or an overlying epithelial defect above an area of infiltration exist, topical antibiotic therapy, QH to Q4H should be initiated using either a topical aminoglycoside or fluoroquinolone.11-15 Fortified agents are generally not required in these cases as most are not the result of corneal microbial infection.12-15 Some of the topical fluoroquinolones are on label for treatment of conjunctivitis and not for the treatment of presumed or confirmed microbial keratitis. Generally, all of them are used interchangeably by the community.11-15 The ones on label for treating bacterial keratitis are ciprofloxacin, ofloxacin and levofloxacin.16,17 If corneal subepithelial infiltration is present and the epithelium is intact, depending on the patient’s visual disability, discomfort and the severity of the inflammation, the addition of a topical steroidal preparation, BID to QID is an option.13,14
Follow up should be started over days to one week depending on severity. Generally, the antibiotic treatment should be maintained for at least seven days. The topical steroid may be tapered as a matter of style; however, as long as it as not been used for more than two weeks, it may be discontinued without tapering. Intraocular pressure should be checked at each visit to ensure there is no steroid response. The practitioner should review the contact lens strategy, fit, material and solutions before allowing the patient to resume wear. If this has happened more than once, rigid lenses or not wearing contact lenses (poor candidate) should be discussed.
Since the threat of microbial contamination and infection exists in all cases of contact lens pathology, using topical steroids at the first visit should be considered with great caution. Topical nonsteroidal anti-inflammatory preparations are an option but only work well for reducing pain; they are not reliable for reducing the effects inflammation and its sequelae. In most cases, conservative initial treatment with cycloplegics and topical antibiotics allow the healing process to begin. Once the corneal epithelium is intact or it is determined that the threat of infection has faded, topical steroids may be added as necessary. Pressure patching is contraindicated. If an infectious corneal ulcer is suspected (central lesion, singular, large, very painful, loss of acuity, heavy cell and flare), culturing may be necessary.
|
1. Tarff A, Behrens A. Ocular Emergencies: Red Eye. Med Clin North Am. 2017;101(3):615-639. 2. Yeung KK, Forister JF, Forister EF, et. al. Compliance with soft contact lens replacement schedules and associated contact lens-related ocular complications: the UCLA Contact Lens Study. Optometry. 2010;81(11):598-607. 3. Dumbleton KA, Woods CA, Jones LW, Fonn D. The relationship between compliance with lens replacement and contact lens-related problems in silicone hydrogel wearers. Cont Lens Anterior Eye. 2011;34(5):216-22. 4. Collier SA, Gronostaj MP, MacGurn AK, et al. Estimated burden of keratitis--United States, 2010. MMWR Morb Mortal Wkly Rep. 2014;63(45):1027-30. 5. Holden BA, McNally JJ, Egan P. Limited lateral spread of stromal edema in the human cornea fitted with a ('donut') contact lenswith a large central aperture. Curr Eye Res. 1988;7(6):601-5. 6. Bruce AS, Nguyen LM. Acute red eye (non-ulcerative keratitis) associated with mini-scleral contact lens wear for keratoconus. Clin Exp Optom. 2013;96(2):245-8. 7. Sankaridurg PR, Willcox MD, Sharma S, et al. Haemophilus influenzae adherent to contact lenses associated with production of acute ocular inflammation. J Clin Microbiol. 1996;34(10):2426-31. 8. Sweeney DF, Jalbert I, Covey M, et al. Clinical characterization of corneal infiltrative events observed with soft contact lens wear. Cornea. 2003;22(5):435-42. 9. Snyder C. Infiltrative keratitis with contact lens wear--a review. J Am Optom Assoc. 1995;66(3):160-77. 10. Szczotka LB, Cocuzzi E, Medof ME. Decay-accelerating factor in tears of contact lens wearers and patients with contact lens-associated complications. Optom Vis Sci. 2000;77(11):586-91. 11. McDonald EM, Ram FS, Patel DV, McGhee CN. Topical antibiotics for the management of bacterial keratitis: an evidence-based review of high quality randomised controlled trials. Br J Ophthalmol. 2014;98(11):1470-7. 12. Shah VM, Tandon R, Satpathy G, et al. Randomized clinical study for comparative evaluation of fourth-generation fluoroquinolones with the combination of fortified antibiotics in the treatment of bacterial corneal ulcers. Cornea. 2010;29(7):751-7. 13. Srinivasan M, Mascarenhas J, Rajaraman R, et al. Corticosteroids for bacterial keratitis: the Steroids for Corneal Ulcers Trial (SCUT). Arch Ophthalmol. 2012;130(2):143-50. 14. Ni N, Srinivasan M, McLeod SD, et al. Use of adjunctive topical corticosteroids in bacterial keratitis. Curr Opin Ophthalmol. 2016;27(4):353-7. 15. Gokhale MS. Medical management approach to infectious keratitis. Indian J Ophthalmol. 2008;56(3):215–220. 16. Dea L, Lewis J, Sharma A. The pharmacist’s role in managing keratitis. US Pharmacist.2018;44(7):1-8. 17. American Academy of Ophthalmology Cornea/External Disease Panel. Preferred practice pattern guidelines, bacterial keratitis-limited revision. San Francisco, CA: American Academy of Ophthalmology; 2013. |

