
Dry eye disease, while common, still presents one of the most challenging and complex diagnostic dilemmas in all of eye care. A multifactorial disorder, the term dry eye represents myriad contributory elements, pathophysiologic processes and clinical presentations.
In the U.S. alone, 4.91 million individuals over the age of 50 suffer from chronic dry eye.1 And, tens of millions more have less severe symptoms and probably a more episodic manifestation of the disease.1-3 Women are affected more commonly than men, and those with such autoimmune disorders as Sjgrens syndrome, diabetes and AIDS also show a higher prevalence of dry eye.4
The core mechanisms in dry eye have been identified as tear film instability and hyperosmolarity, but many additional elements also contribute; of these, the most significant are tear hyposecretion, ocular surface inflammation and lid margin disease.4 Lid margin disease, such as posterior blepharitis or meibomian gland dysfunction (MGD), is currently recognized as the single most common cause of evaporative dry eye.4-6
Detecting Lid Margin Disease
The prevalence of lid margin disease in clinical practice is difficult to estimate because it varies with age and demographics and reflects a number of related disorders. One report, however, suggests that 67.2% of people over the age of 60 in the U.S. have MGD.5 In a study of 70 individuals who complained of ocular discomfort associated with computer use, 74.3% were found to have MGD.7 Lid margin disease can also be linked with a variety of systemic disorders, including rosacea, seborrheic dermatitis and psoriasis, as well as the use of some oral medications.4,8-9 Lid margin disease is an exceedingly common entity and is responsible for the vast majority of symptomatic dry eye patients seen in optometric practice.
The Role of Tear Lipids
All dry eye is either aqueous-deficient or evaporative in nature, according to the Dry Eye WorkShop (DEWS) report.1 Numerous elements, both intrinsic and extrinsic, can provoke or promote aqueous-deficient dry eye and evaporative dry eye. Environmental elements, such as high altitude, low relative humidity or poor air quality (pollution), all lead to enhanced evaporation of the tear film. Likewise, structural eyelid abnormalities (e.g., colobomas, large palpebral apertures and diminished blinking ability) allow for amplified exposure and evaporation.
The most important contributory element in evaporative dry eye, however, is undoubtedly lid margin disease, which manifests as a reduction in vital tear lipids. Tear film lipids originate from the meibomian glands and, to a lesser degree, from the accessory sebaceous glands of Zeiss, located along the eyelid margin. They consist of a variety of both polar and non-polar oils, including wax and sterol esters, triglycerides, hydrocarbons and phospholipids.10,11 With each blink, lipid secretions are expressed along the ocular surface, forming the most distal aspect of the tear film. In this capacity, the lipids serve to provide several essential functions, including:
Lubrication of the ocular surface, which diminishes lid-globe friction.
Reduction of tear film surface tension, allowing for more even distribution and spreading of the tears.
Establishment of a superficial barrier to aqueous tear evaporation.
MGD is believed to represent chronic inflammation within the meibomian glands that is indicated by stagnation of lipid flow and altered composition due to diminished solubility of the polar lipids.12 MGD results in a diminished quantity and/or quality of lipids on the ocular surface. So, patients with this condition experience more rapid tear evaporation and increased ocular surface friction. Ultimately, MGD can lead to significant inflammation of the ocular surface and symptoms of dry eye disease.
Clinical Urgency
From the practitioners point of view, it can be difficultif not impossibleto consistently identify a single causative factor for every patient with dry eye. Many tests, such as vital dye staining, tear volume assessment, interferometry and osmolarity, can be employed in an attempt to qualify and quantify the dry eye state. But, these procedures often yield less than stellar results.
One aspect of the exam that can be helpful, however, is biomicroscopic evaluation of the lid margins. Given the frequency of MGD in clinical practice and its high correlation with tear abnormalities, it is crucial to evaluate patients with dry eye symptoms for lid margin disease. Look for structural irregularities, telangiectatic blood vessels, and madarosis.
Expression of the meibomian glands is also paramount. The secretions should flow easily with moderate but firm pressure applied with a finger or cotton-tipped applicator just proximal to the glands. The expressed lipids should be clear and have the consistency and color of a light cooking oil. Glands that do not express easily with digital pressure or secretions that are thick and cheesy are indicative of MGD. Address MGD therapeutically when managing any case of dry eye.
Managing MGD
Treatment of MGD centers on restoring the glands to a normal, healthy, functional state. Warm compresses and digital lid massage several times daily help to thin the secretions and promote improved meibomian flow.
Supportive therapy also involves the use of artificial tears to help lubricate and maintain the integrity of the ocular surface. Many options for tear replacement exist, but in light of the role that lipids play, it may be logical to utilize a lipid-restorative agent in cases of lid margin disease and meibomian deficiency; those that are commercially available in the United States at this time include Soothe XP (Bausch & Lomb), FreshKote (Focus Laboratories) and Refresh Dry Eye Therapy (formerly Endura, Allergan Pharmaceuticals). For more advanced cases of MGD, clinicians may opt to prescribe a topical antibiotic or antibiotic-steroid combination, such as TobraDex (tobramycin/dexamethasone, Alcon) or Blephamide (sulfacetamide/prednisolone acetate, Allergan).
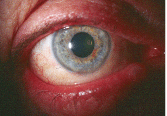
Red, thickened lid margins are a hallmark sign of posterior blepharitis and MGD.
In theory, antibiotics help to diminish the bacterial flora on the lids that are responsible for generating lipases, which alter meibomian gland secretions.12 The addition of a topical steroid can help to address concurrent lid margin inflammation, although not all practitioners prefer such therapy. Recently, a topical formulation of AzaSite (azithromycin, Inspire Pharmaceuticals) has gained significant popularity for the treatment of both anterior and posterior blepharitis. In addition to demonstrating potent antimicrobial activity against the most common lid flora, AzaSite purportedly possesses anti-inflammatory properties as well.13 A macrolide antibiotic, azithromycin has been shown to inhibit inflammatory cell infiltration, edema, mucus hypersecretion and expression of pro-inflammatory cytokines in human tissue.13 In a pilot study of 21 patients with posterior blepharitis, 67% demonstrated improvement in clinical signs and symptoms after just two weeks of AzaSite and lid hygiene therapy vs. 14% of the patients who used warm compresses alone.14 When using AzaSite in such a fashion, the dosing regimen is b.i.d. for two days, then q.d. for two to four weeks.
Another common treatment for chronic lid margin disease involves the use of essential fatty acid (EFA) supplements. EFAs, especially omega-3 fatty acids, tend to be deficient in the typical Western diet; however, these agents evidently have the capacity to improve meibomian secretions by stimulating tear-specific anti-inflammatory prostaglandins.15 Typical dosing consists of 2g to 4g daily, though many varieties of these dietary supplements are available. Patients should be advised to read all packaging directions and precautions. General consensus suggests that adults should consume a daily minimum of 500mg combined DHA and EPA.16
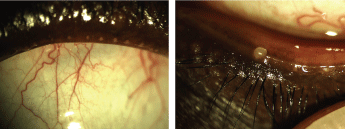
It is crucial to evert the lid margins and inspect the meibomian glands. Left, the gland orifices of the upper lid. Right, a large capped gland on the lower lid margin.
EFA supplements must be used with caution in those patients on systemic anticoagulant or anti-platelet therapy (e.g., blood thinners, such as aspirin, warfarin, clopidogral bisulfate or ticlopidine hydrochloride) because of a potential dose-related effect on bleeding time.17,18 Also, advise patients that increased urinary and/or bowel frequency can occur with these supplements, particularly at high doses or when first initiating therapy.
Oral tetracycline derivatives (e.g., doxycycline and minocycline) have also proven beneficial in cases of advanced MGD. These drugs may hinder the production of bacterial lipases, which serve to alter the consistency of the meibomian oils.19 Additionally, tetracyclines are recognized as potent anti-inflammatory agents that inhibit the expression of matrix metalloproteinases and other cytokines in a fashion similar to azithromycin.20,21 Therapeutic effects may be seen with as little as 40mg of doxycycline hyclate daily, though a delayed response is typical, often taking up to six weeks for patients to see symptomatic improvement.22
Traditional Dry Eye Therapies
Traditional dry eye therapies (artificial tears and topical corticosteroids) may or may not be of benefit in treating evaporative dry eye associated with MGD, and their usage and application have already been discussed. Restasis (cyclosporine A 0.05% ophthalmic suspension, Allergan) is indicated to increase tear production in patients whose tear production is suppressed due to ocular inflammation associated with keratoconjunctivitis siccain other words, in aqueous-deficient dry eye.23 To date, just two published studies have examined the efficacy of topical cyclosporine in patients with MGD.24,25 In the first, cyclosporine was found to be superior to tobramycin/dexamethasone in patients with posterior blepharitis after 12 weeks of therapy and to demonstrate greater improvement in Schirmer scores, tear film break-up time, meibomian gland secretion quality, resolution of lid telangiectasia and diminished symptoms of blurred vision, burning and itching.24
In the second study, a placebo-controlled, prospective three-month evaluation, patients who received topical cyclosporine showed a decrease in fluorescein staining, lid margin vascular injection, tarsal telangiectasis and the number of meibomian gland inclusions. But, no statistically significant improvement resulted in patient symptoms vs. the control (Refresh Plus preservative-free artificial tears).25 While these results are not necessarily conclusivethe studies were small and relatively short-term, at only three months duration eachit is reasonable to assume that the anti-inflammatory/immunomodulatory effects of Restasis would be beneficial for restoring ocular surface homeostasis, even in those with primarily evaporative dry eye.
Prescription oral agents may aid in the treatment of aqueous-deficient dry eye, and, like Restasis, they are utilized specifically to induce production of tears from the lacrimal gland. These secretagogues, which include Salagen (pilocarpine, MGI Pharma) and Evoxac (cevimeline, Daiichi Sankyo), are not yet FDA-approved for the treatment of dry eye; however, they are commonly used for the treatment of dry mouth (xerostomia) associated with Sjgrens syndrome. Numerous reports of concurrent improvement of dry eye symptoms has prompted some to prescribe these medications in an off-label fashion.26-28 Bear in mind, though, that these drugs have multisystem effects and can impact autonomic receptor sites throughout the bodydo not prescribe them haphazardly. In fact, it is recommended that these agents should only be used under the supervision of a rheumatologist.
Embrace the Challenge
Lid margin disease and dry eye are inextricably linked. As the primary driving force behind clinical dry eye syndrome, practitioners must identify, assess and effectively manage lid disease if they are to alleviate patients symptoms and diminish the potentially damaging sequellae of these two related disease states.
Many treatment options exist today, and more are currently under investigation. The real challenge for optometrists, however, is the commitment of time and effort to properly address these conditions within their practices. Too frequently, doctors become complacent, dismissing these disorders as nuisances without attempting to treat them thoroughly or perform the medically necessary follow-up.
Dry eye and lid disease represent tremendous areas of opportunity and growth for optometry, so long as we embrace them as true ocular disease entities worthy of our skill and expertise.
Dr. Kabat is a contributing editor to Review of Optometry. He is a speaker for Alcon Laboratories and Inspire Pharmaceuticals, and he is a member of the Board of Optometric Consultants for Cynacon/ OCuSOFT. He has no direct financial interest in any of the products mentioned in this article.
1. The epidemiology of dry eye disease: report of the Epidemiology Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 2007 Apr;5(2):93-107.
2. Schaumberg DA, Sullivan DA, Buring JE, Dana MR. Prevalence of dry eye syndrome among US women. Am J Ophthalmol 2003 Aug;136(2):318-26.
3. Miljanovic B, Dana MR, Sullivan DA, Schaumberg DA. Prevalence and risk factors for dry eye syndrome among older men in the
4. The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 2007 Apr;5(2):75-92.
5. Bron AJ, Tiffany JM. The contribution of meibomian disease to dry eye. Ocul Surf 2004 Apr;2(2):149-65.
6. Foulks GN. The correlation between the tear film lipid layer and dry eye disease. Surv Ophthalmol 2007 Jul-Aug;52(4):369-74.
7. Fenga C, Aragona P, Cacciola A, et al. Meibomian gland dysfunction and ocular discomfort in video display terminal workers. Eye 2008 Jan;22(1):91-5.
8. Mcculley JP, Dougherty JM. Blepharitis associated with acne rosacea and seborrheic dermatitis. Int Ophthalmol Clin 1985 Spring;25(1):159-72.
9. Fu YA. Ocular manifestation of polychlorinated biphenyls intoxication. Am J
10. McCulley JP, Shine WE. Meibomian gland function and the tear lipid layer. Ocul Surf 2003 Jul;1(3):97-106.
11. McCulley JP, Shine WE. The lipid layer of tears: dependent on meibomian gland function. Exp Eye Res 2004 Mar;78(3):361-5.
12. McCulley JP, Shine WE. Changing concepts in the diagnosis and management of blepharitis. Cornea 2000 Sep;19(5):650-8.
13. Ianaro A, Ialenti A, Maffia P, et al. Anti-inflammatory activity of macrolide antibiotics. J Pharmacol Exp Ther 2000 Jan;292(1):156-63.
14. Luchs J. Efficacy of topical azithromycin ophthalmic solution 1% in the treatment of posterior blepharitis. Adv Ther 2008 Sep;25(9):858-70.
15. Pinna A, Piccinini P, Carta F. Effect of oral linoleic and gamma-linolenic acid on meibomian gland dysfunction. Cornea 2007 Apr;26(3):260-4.
16. Simopoulos AP, Leaf A,
17.
18. Jalili M, Dehpour AR. Extremely prolonged INR associated with warfarin in combination with both trazodone and omega-3 fatty acids. Arch Med Res 2007 Nov;38(8):901-4.
19. Dougherty JM, McCulley JP, Silvany RE, Meyer DR. The role of tetracycline in chronic blepharitis. Inhibition of lipase production in staphylococci. Invest Ophthalmol Vis Sci 1991 Oct;32(11):2970-5.
20. Ralph RA. Tetracyclines and the treatment of corneal stromal ulceration: a review. Cornea 2000 May;19(3):274-7.
21. Stone DU, Chodosh J. Oral tetracyclines for ocular rosacea: an evidence based review of the literature. Cornea 2004 Jan;23(1):106-9.
22. Yoo SE, Lee DC, Chang MH. The effect of low-dose doxycycline therapy in chronic meibomian gland dysfunction. Korean J Ophthalmol 2005 Dec;19(4):258-63.
23. Allergan, Inc. Restasis package insert, 2008.
24. Rubin M, Rao SN. Efficacy of topical cyclosporin 0.05% in the treatment of posterior blepharitis. J Ocul Pharmacol Ther 2006 Feb;22(1):47-53.
25. Perry HD, Doshi-Carnevale S, Donnenfeld ED, et al. Efficacy of commercially available topical cyclosporine A 0.05% in the treatment of meibomian gland dysfunction. Cornea 2006 Feb;25(2):171-5.
26. Tsifetaki N, Kitsos G,
27 Ono M, Takamura E, Shinozaki K, et al. Therapeutic effect of cevimeline on dry eye in patients with Sjgren"s syndrome: a randomized, double-blind clinical study. Am J Ophthalmol 2004 Jul;138(1):6-17.
28. Samarkos M, Moutsopoulos HM. Recent advances in the management of ocular complications of Sjgren"s syndrome. Curr Allergy Asthma Rep 2005 Jul;5(4):327-33.

