 Q: A 31-year-old black female presented to my office with intermittent alternating unilateral lid swelling but no bulbar injection. What systemic diseases should I consider?
Q: A 31-year-old black female presented to my office with intermittent alternating unilateral lid swelling but no bulbar injection. What systemic diseases should I consider?
A: “The first conditions that come to mind as a cause of lid swelling—although not necessarily systemic diseases—include thyroid eye disease, preseptal cellulitis, contact dermatitis or myasthenia gravis,” says Eric Harris, O.D., resident at Omni Eye Services of Atlanta. “But it’s the intermittent frequency, the laterality and the lack of redness that suggest a systemic autoimmune disease—possibly thyroid or postorbital etiology.”
Dr. Harris adds, “In a case like this, the history is going to be the most important element of the exam.”
The intermittent nature of this patient’s condition suggests that she might have been treated previously for the lid swelling. So the history may reveal which treatment(s) were already attempted—and failed to work—to help you rule out possible etiologies, Dr. Harris says.
The history will also bring to light other concomitant or associated signs and symptoms, he says. In this case, it’s unlikely that the lid swelling is her only problem.
Indeed, this proved to be true in the patient’s history. And, Dr. Harris happens to know her history well, because this patient is his sister.
“This whole thing started about a year and a half ago,” he says. “About that time, she was having digestive issues, pretty bad migraines and photosensitivity. Her doctor did some preliminary work and said she had irritable bowel syndrome.”
Dr. Harris wrote a letter to his sister’s primary care physician and requested she receive lab testing when she experienced her next episode. And, as it turned out, her anti-nuclear antibody (ANA) test and lupus prep came back positive.
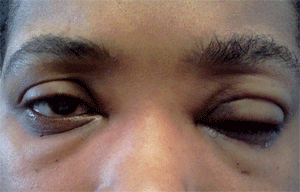
This patient presented with lid swelling and non-specific systemic symptoms.
“Lupus is a non-specific, inflammatory collagen vascular disease,” he says. “The thing about all collagen vascular diseases is that they are very non-specific, and they cause inflammatory damage to connective and vascular tissue. So they’re difficult to tell apart.”
Characteristics that distinguish lupus are that it affects a much higher prevalence of females than males, and affects black females approximately three times more than white females. “The usual profile is a young woman of childbearing age, but plenty of juvenile cases have been documented as well,” Dr. Harris says.
Lupus can cause different and varying symptoms in many organs and organ systems, although the skin is the most common. “The hallmark picture of a typical lupus patient is one who comes in with a malar rash (a dark reddish, “butterfly” rash) or discoid lesions across the face,” he says. But other typical symptoms include joint pain, joint swelling, photosensitivity, headaches, nausea, fatigue and/or chronic low-grade fever.
If you see a similar patient, request an ANA test (among other lab testing). If it comes back positive, send the patient to a primary care doctor for further evaluation. Of course, be sure not to frighten patients with the label of “lupus suspect,” Dr. Harris says.
In cases of lupus, comanagement with the rheumatologist is essential, “because the medications that the rheumatologist prescribes, such as oral steroids or NSAIDs, may affect the ocular manifestations,” he says. Also, certain courses of systemic treatment, such as Plaquenil (hydroxychloroquine, Sanofi-Aventis), may initiate other ocular problems of their own. In his sister’s case, she is still being tested by the rheumatologist to determine her course of treatment.
Above all, “It’s important not to skip steps in these patients,” Dr. Harris says. “And the most important step is a thorough and specific history.”

