 A 46-year-old woman was referred for a specialty ocular surface evaluation after being seen by her family optometrist. “My eyes feel like sandpaper in the morning,” she claimed. “Some days, they burn so badly I can barely open them. I get a little relief after I shower, but my eyes are still very red and irritated for most of the day. I’ve tried all types of eye drops, but most of them sting and nothing provides the relief I need.”
A 46-year-old woman was referred for a specialty ocular surface evaluation after being seen by her family optometrist. “My eyes feel like sandpaper in the morning,” she claimed. “Some days, they burn so badly I can barely open them. I get a little relief after I shower, but my eyes are still very red and irritated for most of the day. I’ve tried all types of eye drops, but most of them sting and nothing provides the relief I need.”
What can we do to help provide this patient with some relief?
Beyond Dry Eye
Many patients present with ocular burning and irritation as either a chief or peripheral complaint. Most eye care providers tend to lump these individuals into the broad diagnostic category of “dry eye,” and treat reactively with one or more artificial tear solutions.
In some instances, we may sense a bacterial or allergic component, and will then add an antibiotic, antihistamine or anti-inflammatory agent (or a combination of these) to the mix. But, in all cases of ocular surface disease, it is important to inspect for mechanical and anatomical dysfunctions that can be at the root of the problem.
In the case presented above, a few simple questions helped lead us to the appropriate cause:
• Are your symptoms worse upon awakening, and do they tend to improve throughout the day?
• Do you sleep under an air vent or ceiling fan?
• Has anyone ever mentioned that you sleep with your eyes partially open?
If the answer to these questions is “yes”––as was the case in our patient––then the likely diagnosis is nocturnal lagophthalmos.
What is Nocturnal Lagophthalmos?
One of the first individuals to discuss nocturnal lagophthalmos in the modern era was Herbert Kaufman, M.D. Dr. Kaufman, and fellow researcher Jeffrey Katz, M.D., described nocturnal lagophthalmos as “corneal exposure during sleep […] a relatively common cause of previously undiagnosed, chronic keratitis.”1
The term lagophthalmos has a most interesting derivation; it comes from the Greek word lagos––meaning hare––as members of the rabbit family were once believed to sleep with their eyes open.2,3 Lagophthalmos can result from a number of potential causes, but usually is attributable to one of three etiologies: proptosis, or excessive ocular surface exposure; palpebral insufficiency (e.g., shortened tarsal height or reduced tonus); and idiopathic.2
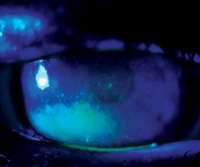
Patients with nocturnal lagophthalmos characteristically present with this telltale staining of the inferior cornea that corresponds to the area of exposure. Photo: Diana L. Shechtman, O.D.
While some of the syndromes associated with nocturnal lagophthalmos may be readily obvious (i.e., thyroid eye disease and cicatricial lid scarring), other cases may be more elusive. In some patients, the eyelashes may obscure a definite gap in the palpebral fissure, making it difficult to observe on clinical examination.
Even more confusing is the situation in which the upper lid extends beyond the edge of the lower eyelid, leaving a small gap that allows the ocular surface to remain exposed to the environment.2 So, it is important to recognize the classic, symptomatic presentation and discern the specific elements of the patient history outlined above to accurately diagnose these patients.
Testing for Lagophthalmos
Additional testing can help you confirm a diagnosis of nocturnal lagophthalmos. Slit lamp evaluation may reveal an incomplete blink along with desiccation and inflammation of the exposed region. Typically, the patient will demonstrate fluorescein staining at the exposed area of the ocular surface that usually occurs in a “band” pattern along the lower third of the cornea.
Conjunctival injection in the interpalpebral zone, with or without associated lissamine green dye staining, is another important sign. Chronic disease can lead to inferior corneal scarring and vascularization as well as conjunctivochalasis.3
Direct testing for lagophthalmos is not complicated. First, slightly recline the patient in the exam chair and dim the overhead room lights. Then, instruct him or her to gently close both eyes, as if preparing to take a nap. Exposure is often not immediately apparent, but after 30 to 60 seconds, the upper eyelid on the most afflicted side frequently begins to twitch. Exposure of the ocular surface then may be observed using a penlight or transilluminator that is directed beneath the lower lid.3
Treatment Options
Treatment of nocturnal lagophthalmos can be supportive or invasive, depending upon the patient’s disposition and the condition’s severity. All attempts should be made to rearrange the patient’s sleeping environment in a way that minimizes direct airflow toward the eyes and maximizes environmental moisture, including the possible use of a room humidifier in dryer climates.
Likewise, any concurrent blepharitis or meibomian gland dysfunction (MGD) should be addressed and treated accordingly because these conditions only exacerbate the inflammation and intensify the symptoms experienced upon awakening.
Mildly symptomatic individuals with nocturnal lagophthalmos may find relief with the use of bland ointments at bedtime, such as Refresh Lacri-Lube (Allergan) or Systane Nighttime (Alcon). For patients who prefer not to use eye ointments due to blur or discomfort, we often recommend higher- viscosity tear products, such as GenTeal Gel (Novartis) or Refresh Celluvisc (Allergan).
In addition to generous lubrication of the eyes at bedtime, it is also important to ensure mechanical lid closure. Physical taping of the eyelids has been advocated in the past; however, this approach is often not well tolerated, and may result in contact dermatitis or iatrogenic lash epilation in some individuals.1-3
Typically, we recommend the use of a “sleep mask” as a first-line therapy for these patients, which may be obtained at virtually any drugstore or beauty supply shop. Eye Eco, Inc., for example, has developed numerous products to shield and protect the eyes from dryness and lagophthalmos, such as the Tranquileyes line and its newer silicone sleep shields.
More symptomatic patients, however, may require pharmacologic intervention. The use of certain topical antibiotics (e.g., erythromycin or azithromycin) may be beneficial in addressing some of the chronic lid changes seen concurrently with nocturnal lagophthalmos, such as anterior blepharitis and MGD.4,5
Likewise, the use of topical NSAIDs or corticosteroids may be beneficial in the initial management of severely inflamed or symptomatic patients. However, these rarely are a long-term solution and likely should be limited to no more than two weeks of therapy.
The use of oral tetracycline derivatives is often recommended for a variety of inflammatory lid disorders, because these agents have been shown to reduce the expression of matrix metalloproteinases, decrease the production of lipase by staphylococci, reduce the eyelid bacterial flora and alter meibum secretion in a positive way.2
Some researchers have even advocated the administration of a Botox (onabotulinumtoxinA, Allergan) injection into the levator of these patients; however, this treatment is not widely accepted as an effective long-term strategy.6
For patients with unrelenting lagophthalmos that impacts sleep and daily quality of life, surgical intervention may be necessary.7 Lid lengthening procedures typically are reserved for patients who may have mechanical obstruction or cicatricial scarring. For those with neural dysfunction (e.g., seventh nerve palsy), tarsorrhaphy may be required.
However, for individuals with idiopathic nocturnal lagophthalmos, “lid loading” with weighted implants often helps facilitate complete closure with minimal effort.6 Complications of this procedure may include implant migration or extrusion, excessive ptosis and secondary astigmatism. But, because the weights are easily removed, this procedure offers great promise for the most symptomatic patients.6,8
Patients with dryness, burning and irritation may indeed have “dry eye syndrome,” but this is just one diagnosis in a litany of ocular surface disorders. The successful clinician is one who takes the time to scrutinize, examine, converse with and educate his patients, no matter how seemingly trivial or routine the presentation may seem.
Drs. Kabat and Sowka are paid consultants for Alcon, and Dr. Kabat serves on the Institutional Advisory Board for Allergan.
1. Katz J, Kaufman HE. Corneal exposure during sleep (nocturnal lagophthalmos). Arch Ophthalmol. 1977 Mar;95(3):449-53.
2. Latkany RL, Lock B, Speaker M. Nocturnal lagophthalmos: an overview and classification. Ocul Surf. 2006 Jan;4(1):44-53.
3. Tsai SH, Yeh SI, Chen LJ, et al. Nocturnal lagophthalmos. Int J Gerontol. 2009;3(2):89-95.
4. Haque RM, Torkildsen GL, Brubaker K, et al. Multicenter open-label study evaluating the efficacy of azithromycin ophthalmic solution 1% on the signs and symptoms of subjects with blepharitis. Cornea. 2010 Aug;29(8):871-7.
5. Opitz DL, Tyler KF. Efficacy of azithromycin 1% ophthalmic solution for treatment of ocular surface disease from posterior blepharitis. Clin Exp Optom. 2011 Mar;94(2):200-6.
6. Pereira MV, Glória AL. Lagophthalmos. Semin Ophthalmol. 2010 May;25(3):72-8.
7. Waller EA, Bendel RE, Kaplan J. Sleep disorders and the eye. Mayo Clin Proc. 2008 Nov;83(11):1251-61.
8. Bergeron CM, Moe KS. The evaluation and treatment of upper eyelid paralysis. Facial Plast Surg. 2008 May;24(2):220-30.

