 |
Q:
A 66-year-old patient with dry age-related macular degeneration (AMD) presented with new symptoms. What are the best next steps to evaluate, educate and manage?
A:
“Just knowing the right diagnosis is not enough to ensure the best care for our patients,” says Jeff Gerson, OD, of Grin Eyecare in Kansas City, KS. “We need to let them know what to expect and how things could progress on the journey ahead of them.”
The patient that was being followed for dry AMD was using a digital home monitoring system. She was called and asked to come in for an evaluation because the system sent an alert. Dr. Gerson uses Notal Vision ForeSee Home on all patients with intermediate AMD. It is approved for intermediate AMD with vision of 20/50 or better.
 |
|
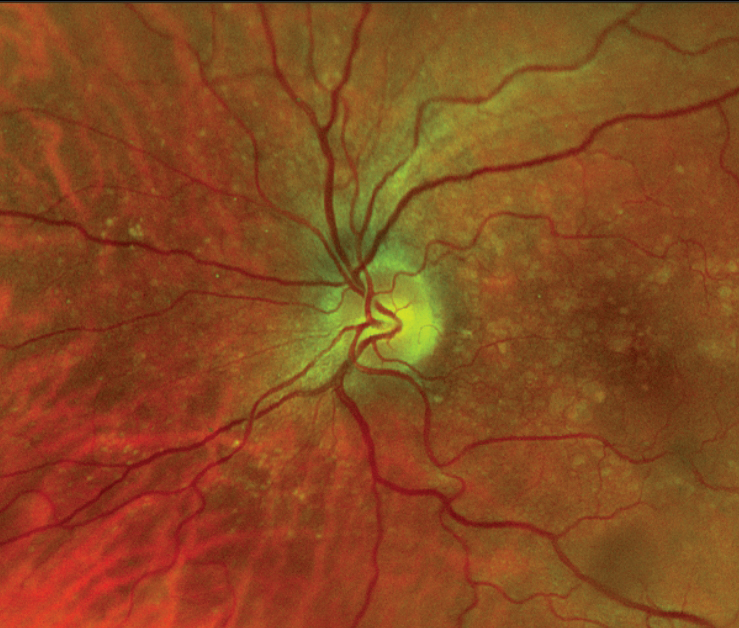
Intermediate AMD with large drusen. |
Stay on Top of AMD
When Dr. Gerson called her, she said that her vision seemed fine, but she came in the next day and her best corrected vision was 20/30 in the affected eye, down from 20/25. Examination with optical coherence tomography (OCT) revealed that her left eye had converted from dry to wet AMD. A choroidal neovascular membrane with subretinal fluid was noted.
“We discussed the findings, happy that this was being detected before anything catastrophic had occurred,” Dr. Gerson says. “While in the office, we called the retina specialist we trust and scheduled an appointment for her the next day, not leaving it to chance.”
When evaluating patients with a progressive eye disease like AMD, it’s crucial to remain aware of clinical signs that may indicate potential advancement. Educate all patients with AMD on symptoms of exudative conversion and the need for prompt examination, typically within 24 hours of onset.
To differentiate between stages of AMD, recall that the AREDS defined intermediate AMD as being any retinal pigment epithelium changes or the presence of drusen 125µm or more in diameter.1
Dr. Gerson discussed the patient’s prognosis and what the retina doctor would do regarding diagnosis and treatment. He also reviewed the research that had shown that vision at time of diagnosis helps predict prognosis.2
Treatment
We discussed that anti-VEGF injections are the mainstay of wet AMD treatment, and that the worst part of the injection is the anxiety beforehand. I told her that most people will have a few loading dose injections, and then it is likely that with the new medications, specifically Vabysmo (faricimab, Genentech), injections will be able to be spread out to every 12 to 16 weeks. Also, just-released data from the PULSAR study has shown that 8mg Eylea (aflibercept, Regeneron) will allow up to 80% of wet AMD patients go 12 to 16 weeks between injections.3 While Vabysmo will allow for longer intervals between injections, the previously approved drugs still work well and are sometimes what insurance will cover.
Prompt treatment of wet AMD is associated with better long-term visual outcomes, and many cases of severe vision loss can actually be prevented through early detection and referral.
Optometrists must stay current on the latest advancements in anti-VEGF therapies as well as how to manage and follow patients long-term. This includes recognizing potential adverse events and any safety concerns.
Dr. Gerson strongly encourages home self-screening, and patients should be educated on how to properly use these screening tools. “The percentage of retina doctors (and optometrists) using it is growing,” he says. “No retina doc will say home screening is a bad idea; however, they should take the time to tell a patient about it.”
Despite their utility, home self-screening tools do not replace the need for frequent in-office examinations.
Dr. Ajamian is board certified by the American Board of Optometry and serves as Center Director of Omni Eye Services of Atlanta. He is vice president of the Georgia State Board of Optometry and general CE chairman of SECO International. He has no financial interests to disclose.
1. Macular Photocoagulation Study Group. Risk factors for choroidal neovascularization in the second eye of patients with juxtafoveal or subfoveal choroidal neovascularization secondary to age-related macular degeneration. Arch Ophthalmol. 1997;115(6):741-7. 2. Ho AC, Kleinman DM, Lum FC, et al. Baseline visual acuity at wet AMD diagnosis predicts long-term vision outcomes: an analysis of the IRIS Registry. Ophthalmic Surg Lasers Imaging Retina. 2020;51(11):633-9. 3. ClinicalTrials.gov. Study to gather information on safety and use of high dose aflibercept injection into the eye in patients with an age-related eye disorder that causes blurred vision or a blind spot due to abnormal blood vessels that leak fluid into the light sensitive lining inside the eye (PULSAR). clinicaltrials.gov/ct2/show/NCT04423718. Accessed December 1, 2022. |

