A 57-year-old Hispanic male presented for an eye exam and requested an updated spectacle Rx. The patient did not remember when his eyes were last evaluated; however, he reported that his last check-up was “many years ago.” The patient also advised that his vision had been reduced for at least 25 years, but had remained stable. He denied any history of ocular trauma. His medical and family ocular histories were unremarkable.

On examination, the patient’s best-corrected visual acuity was 20/70 O.D. and 20/60 O.S. Extraocular motility testing was normal and he was orthophoric on cover testing O.U. His confrontation visual fields were full to careful finger counting O.U. Pupils were equally round and reactive, with no afferent pupillary defect. The anterior segment examination was unremarkable in both eyes. Intraocular pressure measured 17mm Hg O.U.
Dilated fundus exam showed a clear vitreous O.U. Examination of the optic nerve revealed small cups with good rim coloration and perfusion in both eyes. The vessels and peripheral retinae were normal O.U. We documented peculiar yellow changes in both foveae (figures 1 and 2). Also, we obtained a spectral domain optical coherence tomography (SD-OCT) scan of each macula (figures 3 and 4).
Take the Quiz Retina Quiz
1. How would you characterize the macular changes seen in both eyes?
a. Tractional.
b. Age-related degenerative.
c. Photochemical disruption.
d. Dystrophy.
2. What does the SD-OCT of the maculae reveal?
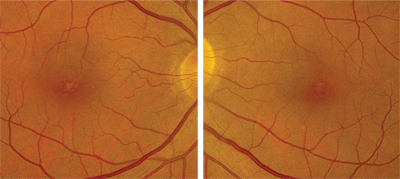
1, 2. The macular images of our patient reveal yellow-white spots and dots in both foveae.
a. Cystoid macular edema (CME).
b. Retinal pigment epithelial detachment.
c. Disruption of the inner and outer photoreceptor segments.
d. Disruption of the inner photoreceptor segments.
3. What is the correct diagnosis?
a. Dry macular degeneration.
b. Solar maculopathy.
c. Adult vitelliform macular dystrophy.
d. Nicotinic acid macular degeneration.
4. How should this patient be managed?
a. Electrodiagnostic testing.
b. Visual evoked potential.
c. Color vision testing.
d. Low vision exam.
For answers, see
below.
Discussion
It was difficult to explain the macular changes observed in our patient. The yellow spots and dots in the center of the fovea seemed nonspecific and not at all consistent with his level of visual acuity. Furthermore, there was no subretinal fluid or macular edema to help explain his vision loss. The SD-OCT scan provided the most useful information; it showed a clear defect in the outer retina at the level of the inner and outer photoreceptor segment (IS/OS) junction. This junction is also sometimes referred to as the photoreceptor integrity line (PIL), which is clearly irregular and even missing in some areas. Interestingly, only the fovea is involved in this case (the scan appeared normal immediately outside of the fovea, where the PIL was completely intact).
With the SD-OCT findings, we were able to explain why the patient’s visual acuity was reduced. But, this led directly to our next question: Why does the patient have this anatomical variation?
We considered several conditions, such as cone dystrophy and a rod monochromate, that could cause such a striking defect in the PIL. The patient returned two weeks later for an electroretinogram (ERG) and color vision testing, which were both normal. As we pondered other possibilities, the patient informed us that, for many years, he would stare at the sun with various optical and telescopic devices. Given this history––and a review of the relevant literature––we diagnosed solar maculopathy.
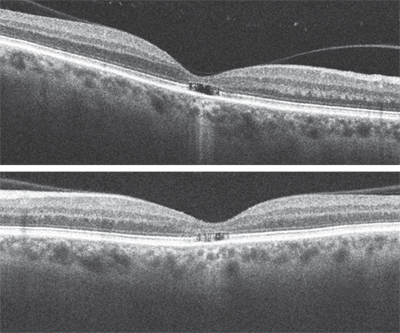
3, 4. Here are the SD-OCT images of our patient’s maculae. What do you notice?
Solar maculopathy develops as a result of photochemical damage to the retina when visible spectrum light (particularly from the blue end) causes retinal injury.1,2 It is thought that photoreceptors suffer fragmentation and vesiculation of the rod and cone outer segment lamellae as well as pyknosis of the nuclei, especially the parafoveal rods.3 We are starting to see these same ultrastructural changes on SD-OCT. Relative survival of foveal cones may account for a good prognosis for visual acuity.3
There are many factors that can determine the nature and extent of injury, including pigmentation, clarity, nature of the media, wavelength of light exposure, wavelength exposure duration and body temperature. Most patients maintain good acuity following exposure, but this is highly dependent upon how often and how long the patient has gazed at the sun.
The classic presentation of solar maculopathy is that of a brick red, sharply circumscribed, lamellar, faceted lesion in the fovea.1 This type of lesion is highly suggestive of previous sun gazing. In the early stages of solar maculopathy, a small, yellow-white spot surrounding a faint, gray zone will develop in the fovea. This presentation often fades over several days and will be replaced by a reddish spot with a pigment halo. After about two weeks, the reddish spot fades and is replaced by the brick red lamellar lesion. This is the most common presentation of solar maculopathy; however, this is not what our patient exhibited.1
Indeed, our patient had yellow spots and dots in the fovea, but not the more obvious brick red lamellar lesion. Perhaps this is due to more severe photochemical damage, resulting from repeated episodes of sun gazing using telescopic and optical devices.
Once we reached the diagnosis of solar maculopathy, we performed a literature search in an effort to find a documented case with a similar presentation to that of our patient. One report, which will be published in Optometry and Vision Science in August 2011, described SD-OCT findings in two patients with solar maculopathy. These two patients had clinical and diagnostic findings almost identical to those of our patient.4
Regarding treatment, there was not much more we could do for our patient beyond recommending a low vision exam. He has long since stopped sun gazing. Unfortunately, however, irreversable damage already has been done.
1. Gass JD. Photic maculopathy. In: Stereoscopic Atlas of Macular Diseases, vol. 2. St. Louis: The CV Mosby Company; 1987:570-3.
2. Stokkermans TJ, Dunbar MT. Solar retinopathy in a hospital-based primary care clinic. J Am Optom Assoc. 1998 Oct;69(10):625-36.
3. Hope-Ross MW, Mahon GJ, Gardiner TA, et al. Ultrastructural findings in solar retinopathy. Eye (Lond). 1993;7 ( Pt 1):29-33.
4. Klemencic S, McMahon J, Upadhyay S, et al. Spectral domain optical coherence tomography as a predictor of visual function in chronic solar maculopathy. Optom Vis Sci. 2011 May 5. [Epub ahead of print]
Answers to the Retina Quiz
1. c
2. c
3. b
4. d

