 |
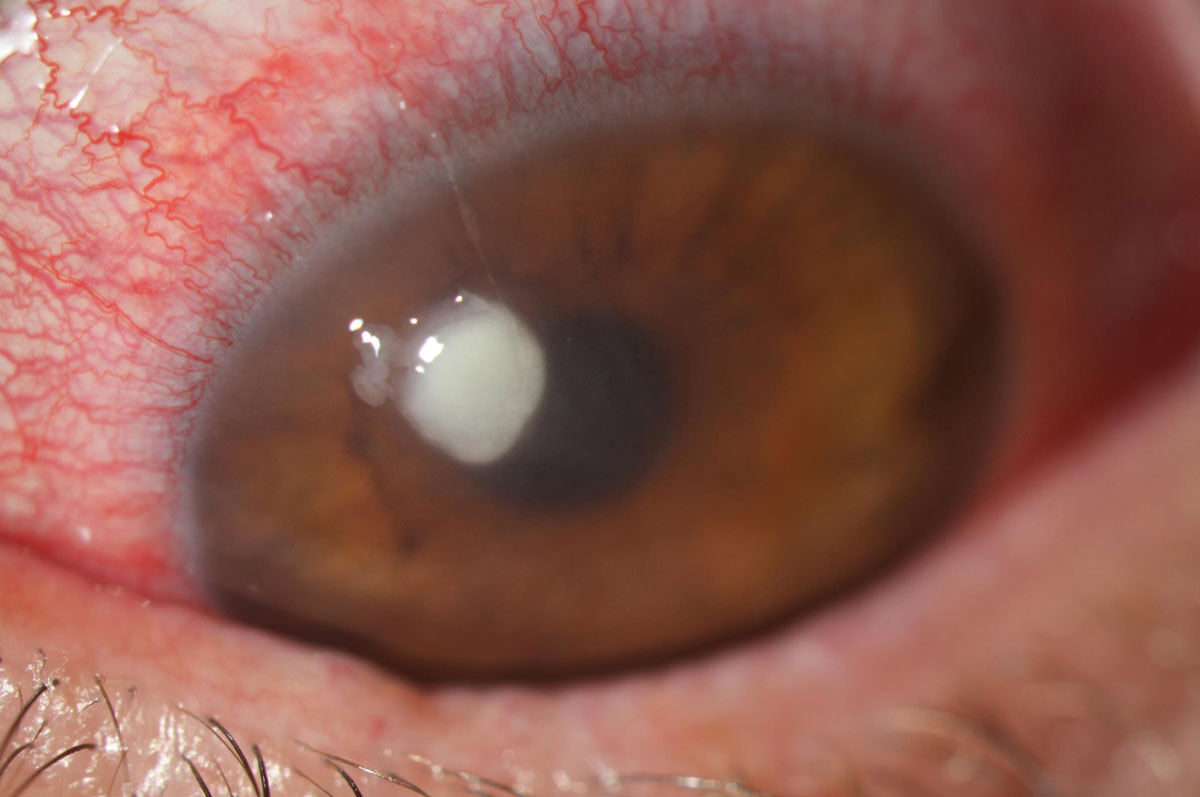
| Staphylococcal infections demonstrated greater susceptibility to even some older medications in the newest ARMOR study. Photo: Aaron Bronner, OD. Click image to enlarge. |
Treating ocular infections is hard enough as is when the drugs work as advertised, and so much worse when the offending microorganism is resistant or only weakly susceptible to therapy. Staphylococci are known causative pathogens in ophthalmic infections, and antibiotic resistance among these bacteria is of clinical concern. The long-running Antibiotic Resistance Monitoring in Ocular micRoorganisms (ARMOR) Study, the only nationwide surveillance study of its kind, captures in vitro data specific to common ocular pathogens. With two research posters, the same team presented their findings on the 14th year of the study’s data collection at ARVO 2023 in New Orleans. Each noted that, with preliminary data indicating lower resistance rates especially among Staphylococcus aureus, multidrug resistance was common among methicillin-resistant strains.
One analysis reported on 2022’s data, when 397 isolates were collected January through October of that year.1 Staphylococcus aureus, coagulase-negative staphylococci (CoNS), Streptococcus pneumoniae, Pseudomonas aeruginosa and Haemophilus influenzae from ocular infections were collected as part of ARMOR and submitted to a central laboratory for species confirmation and in vitro antibiotic susceptibility testing. Minimum inhibitory concentrations for up to 16 antibiotics (10 drug classes) were determined and interpreted.
The 142 CoNS isolates exhibited the highest resistance, with azithromycin, oxacillin/methicillin, trimethoprim, clindamycin and tetracycline resistance observed in 60%, 37%, 28%, 27% and 22% of isolates, respectively. Among the 161 S. aureus isolates, 46% were resistant to azithromycin, but <20% of isolates were resistant to other drugs. Multidrug resistance (poor or ineffective response to three or more drug classes) was observed in 14% of S. aureus, 39% of CoNS and in 59% and 88% of methicillin-resistant strains thereof, respectively. Among the five S. pneumoniae isolates, 60% were resistant to azithromycin, oral penicillin and tetracycline. Although all 72 P. aeruginosa isolates were resistant to polymyxin B, <5% were resistant to other drugs; no resistance was found among the 17 H. influenzae isolates.1
“The clinical significance of these in vitro data is unclear without consideration of the ocular pharmacokinetics of tested antibiotics,” the researchers concluded in their abstract.1
The team’s other study examined resistance trends over time among staphylococcal isolates collected from 2009 through 2022 in ARMOR. A total of 2,999 S. aureus and 2,575 CoNS were included in their analysis.2
In vitro resistance decreased to methicillin/oxacillin (S. aureus, 39% in 2009 to 18% in 2022; CoNS, 50% in 2009 to 37% in 2022) and to ciprofloxacin (S. aureus, 39% in 2009 to 17% in 2022; CoNS, 46% in 2009 to 20% in 2022). Additionally, among S. aureus, resistance to azithromycin decreased (62% in 2009 to 46% and 9% in 2022), as did resistance to tobramycin (24% in 2009 to 9% in 2022), while in contrast an increase in chloramphenicol resistance was observed (7% in 2009 to 3% in 2022, peaking at 30% in 2021). Cumulative multidrug resistance (three or more antibiotic classes) was observed in 30% of S. aureus and 41% of CoNS and in 76% and 79% of methicillin-resistant isolates thereof, respectively.
The researchers also noted that resistance data should be considered in combination with known ocular pharmacokinetics of antibiotics. However, this time they emphasized that practitioners should also consider resistance data when selecting empirical treatment for staphylococcal eye infections in particular.2
Original abstract content © Association for Research in Vision and Ophthalmology 2023.
1. Sanfilippo CM, DeCory H, Asbell PA. Antibiotic resistance among ocular pathogens – an update from the 2022 ARMOR Study. ARVO 2023 annual meeting. 2. Asbell PA, Sanfilippo CM, DeCory H. Longitudinal analysis of in vitro antibiotic resistance rates among ocular staphylococci collected in the ARMOR Study. ARVO 2023 annual meeting. |

