 Dont ask, dont tell is what fellow practitioners tell us when discussing how often they see ocular surface disease (OSD) in their glaucoma patients. Nonetheless, a number of questions arise when we start to think about glaucoma and OSD together: How much of a problem truly exists? What are the clinical implications? What can I do to improve their ocular health and enhance satisfaction?
Dont ask, dont tell is what fellow practitioners tell us when discussing how often they see ocular surface disease (OSD) in their glaucoma patients. Nonetheless, a number of questions arise when we start to think about glaucoma and OSD together: How much of a problem truly exists? What are the clinical implications? What can I do to improve their ocular health and enhance satisfaction?
New Findings on OSD
New information became available this year regarding glaucoma and OSD. Ocular Surface Disease Index (OSDI) results from a study involving 630 glaucoma patients with a mean age of 69.4 years indicated that OSD occurred in 48.4% of patients: 21.3% mild, 13.3% moderate and 13.8% severe.1 Patients on multiple medications reported statistically significantly higher scores.
In a cross-sectional study of 101 medically treated glaucoma or ocular hypertensive patients, 59% reported symptoms, and Schirmer testing showed a decrease of 61% in tear production in at least one eye.2 Corneal and conjunctival lissamine green staining showed positive results in 22%. Tear film break-up time (TFBUT) was significant, with abnormal tear quality in 78%; severe decrease was found in 65%. Researchers found that each additional benzalkonium chloride (BAK)-containing eyedrop was associated with a doubled risk of abnormal lissamine green staining.
Clinical Implications
There are a number of things to think about as we look at these patients. The most obvious: patient comfort. Common symptoms of OSD include itching, burning, stinging, grittiness, redness, irritation, dryness and excessive tearing. Patient comfort can impact adherence. Adverse effects have been reported to be the third most common reason for poor adherence in glaucoma patients.3
Visual function is another important consideration. Changes in the ocular surface with dry eye can be observed as a significant decrease in TFBUT. Alterations in TFBUT, reflective of ocular surface and tear film changes, negatively impact visual image quality, resulting in blurred vision.4 Clinically, we hear complaints about difficulty reading, driving or watching TV, or having frequent eyeglass prescription changes.
These can be a factor in patient satisfaction. In a three-month study of 690 patients who switched to the BAK-free prostaglandin, Travatan Z (travoprost, Alcon Laboratories) from prior therapy with either latanoprost or bimatoprost, 72% desired to remain on the new medication after treatment.5 Most patients improved by at least one OSDI grade; half returned to normal and 57% decreased by 9 points on the OSDI at the conclusion of the switching study. Significant improvements in symptoms (e.g., photophobia, pain, grittiness and blurred vision) and visual function (e.g., driving at night, reading and computer use) accounted for this satisfaction.
What Can You Do?
Ask about concurrent problems when taking a patients history. Document all of the medications being taken, including all topical medications, over-the-counter (OTC) products and systemic agents.
The OSDI and TFBUT are two useful tools that can be clinically meaningful. The OSDI, a validated patient-reported survey, consists of 12 questions, which are graded from zero to four, and provides an appreciation for patient symptoms, visual function, precipitating conditions and quality of life.6 It can provide a useful, objective patient-based baseline and way to follow OSD symptom data. This easy-to-administer survey can be given to patients as theyre waiting to see you.
The TFBUT is one of the best screening tests for dry eye disease.6 Fluorescein staining can easily be used to visualize TFBUT and indicate areas of corneal damage. Considering the blink cycle, a TFBUT of less than six seconds points to underlying OSD.7
A decrease in TFBUT results in redness, itching and discomfortand it can signify something deeper: chronic inflammation. Use this test on patients in whom you suspect OSD problems and need an objective sign that can be consistently followed.
This chart demonstrates the impact of decreased tear film break-up time. Note the amount of time that the ocular surface is unprotected.
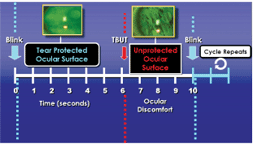
Courtesy: Ophthalmic Research Associates
Management Strategies
In managing glaucoma patients, practitioners should begin to think about their medicationsnot just from their ability to lower IOP, but whether they contain BAK.
Clinicians should be aware of all topical preparations used by patients, including OTC agents. Often, we will reach for a tear to manage patients with OSD. A BAK-free product should be selected so as not to further exacerbate existing inflammation and to alleviate OSD symptoms.8
An ongoing assessment of medications should be made to minimize patients BAK load. Fortunately, there are several BAK-free products available:
Timoptic in Ocudose (Aton Pharma), a unit-dose timolol formulation product without BAK.
Alphagan P (brimonidine tartrate 0.1% and 0.15%, Allergan), preserved with Purite. Prostaglandin analogues are commonly used in glaucoma patients.
Travatan Z, which uses an alternative preservative system, sofZia, an effective preservative in the bottle that breaks into non-toxic components on the ocular surface. Recent clinical experience points to significant improvements in OSDI and TFBUT scores in patients previously treated with other prostaglandins.9
When changing the glaucoma regimen, patient counseling is important. OSD will take some time to return to normalit may take one to three months for patients to notice a difference, and sometimes signs that reflect improvement in the cornea may occur before patients report better symptoms.
OSD is a condition that exists in at least half of our glaucoma patients. Patient comfort and visual function are of concern, influencing adherence, quality of life and satisfaction.
We have the ability to identify these patients by asking about concurrent conditions, medications and OSD; noting discomfort complaints or the need for lens prescription changes; and employing the OSDI and TFBUT.
Decreasing the BAK load of these patients may be done with both BAK-free tear preparations and glaucoma medications.
Proper counseling is imperative; managing OSD in our glaucoma patients is not a short-term issue, and it requires a long-term view focused upon the overall health of the eye.
Drs. Sowka and Kabat are members of the Alcons Speaker Bureau and have had lecture sponsorship by Allergan. This manuscript was prepared following an Alcon-sponsored lecture done by Dr. Sowka, and the authors thank John York of Akita Biomedical for his help in assembling this column.
1. Fechtner RD, Budenz DL, Godfrey DG, et al. Prevalence of ocular surface disease symptoms in glaucoma patients on IOP-lowering medications. Poster presented at American Glaucoma Society 18th Annual Meeting, March 6-9, 2008,
2. Leung EW, Medeiros FA, Weinreb RN. Prevalence of ocular surface disease in glaucoma patients. J Glaucoma 2008 Aug;17(5):350-55.
3. Chawla A, McGalliard JN, Batterbury M. Use of eyedrops in glaucoma: how can we help to reduce non-compliance? Acta Ophthalmol Scand 2007 Jun;85(4):464.
4. Tutt R, Bradley A, Begley C,
5. Henry JC, Peace JH, Stewart JA, Stewart WC. Efficacy, safety, and improved tolerability of travoprost BAK-free ophthalmic solution compared with prior prostaglandin therapy. Clin Ophthalmol 2008 Oct;2(3):613-21.
6. Ozcura F, Aydin S, Helvaci MR. Ocular surface disease index for the diagnosis of dry eye syndrome. Ocul Immunol Inflamm 2007 Sep-Oct;15(5):389-93.
7. Abelson MB, Ousler GW 3rd, Nally LA, et al. Alternative reference values for tear film break up time in normal and dry eye populations. Adv Exp Med Biol 2002;506(Pt B):1121-5.
8. The definition and classification of dry eye disease: report of the Definition and Classification Subcommittee of the International Dry Eye WorkShop (2007). Ocul Surf 2007 Apr;5(2):75-92.
9. Horsley MB, Kahook MY. Changes in tear break-up time and ocular surface disease index after initiation of travoprost with sofZia in patients previously using latanoprost with benzalkonium chloride. Presented at American Glaucoma Society 18th Annual Meeting, March 6-9, 2008,
10. Noecker R. Ophthalmic Preservatives: Considerations for Long-term Use in Patients With Dry Eye or Glaucoma. Rev Ophthalmol 2001 June. Available at: www.revophth.com/2001/june/cme0601_article.htm (Accessed June 5, 2006).

