 History
History
A 53-year-old white male presented with a chief complaint an “ugly growth” inside the superior portion of his left eyelid. He insisted that the growth be removed.
The patient explained that the growth began as a small bump, but steadily grew larger during the last two months. His medical doctor prescribed sulfacetamide cream and hot compresses, which did not appear to be working.
His systemic history was remarkable for hypertension, for which he was properly medicated (and compliant with the regimen). He reported no known allergies or contributory history.
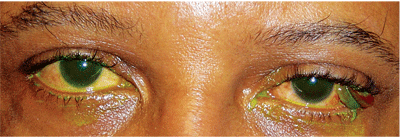
This 53-year-old patient presented with a chief complaint of an “ugly growth” inside the eyelid of his left eye. What is the likely cause of this growth?
Diagnostic Data
His best-corrected visual acuity was 20/20 O.U. at distance and near. External examination revealed a non-tender, lobular, pedunculated, soft, nodular papule on his left eyelid. The anterior segment examination was normal, with no corneal epitheliopathy or anterior chamber finding.
His intraocular pressure measured 14mm Hg O.U. The dilated fundus examination was normal.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What’s the likely prognosis?
Additional patient history should include questions about chronic eyelid disease or previous eyelid surgeries. This patient was queried, but had no relevant events. Additional tests should include an examination of the preauricular, submandibular and sublingual lymph nodes; evaluation of the eyelids for lumps or bumps; and analysis of the cilia for collarettes, nits and blepharitis.
The diagnosis in this case is pyogenic granuloma. Pyogenic granulomas result from vasoproliferation of granulation tissue.1-3 Granulomas represent a form of aberrant wound healing from mucous membranes and skin where capillaries and tissues evolve in a cascade that is sequenced by cytokines and angiogenic factors. Typically, the observed growth rate is rapid, which can serve as a differentiation indicator from neoplastic lesions. Granulomatous lesions often develop following oculoplastic procedures, chalazion appearance and adnexal surgery.1,2
Treatment of pyogenic granuloma consists of topical steroid drops q.i.d. and topical lubricating ointments. Cryosurgery, electrodessication, chemical cauterization, excision and biopsy or laser surgical procedures are also potential options.1-3
We put our patient on topical prednisolone acetate drops q.i.d. and bacitracin ointment h.s. O.S. At the two-week follow-up, the lesion was 95% resolved. With cosmesis protected and function secure, no additional treatments or procedures were explored. The bacitracin was continued until finished and the prednisolone drops were tapered slowly over a two-week period, then discontinued. Follow-up to ensure stability was established at three-month intervals.
1. Ajamian PC. A lesion a year after surgery. Rev Optom 2002 Sept;139(9):103.
2. Jordan DR, Brownstein S, Lee-Wing M, Ashenhurst M. Pyogenic granuloma following oculoplastic procedures: an imbalance in angiogenesis regulation? Can J Ophthalmol. 2001 Aug;36(5):260-8.
3. González S, Vibhagool C, Falo LD Jr, et al. Treatment of pyogenic granulomas with the 585 nm pulsed dye laser. J Am Acad Dermatol. 1996 Sep;35(3 Pt 1):428-31.

