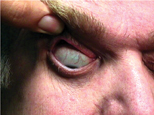
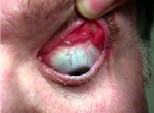
Q. A 55-year-old male presented with a six-month history of a mildly red, irritated left eye, keratitis and some GPC. Two doctors diagnosed him with dry eye and gave him artificial tears. Another gave him an antibiotic. On inferior gaze, he exhibited a lack of eyelid-globe contact (figures 1 and 2). What is the diagnosis?

A. This patient likely has floppy eyelid syndrome (FES), characterized by loose lids that spontaneously evert resulting in a loss of eyelid-globe contact. The symptoms of a chronically red, irritated eye combined with loose, rubbery lids that are easily everted, suggest the diagnosis, says Maynard Pohl, O.D., clinical director of the Pacific Cataract and Laser Institute in Bellevue, Wash.
Many doctors misdiagnose FES as conjunctivitis because of its non-specific symptoms.1 Punctate keratitis, beginning SPK and inflamed conjunctivae are specific to too many different ocular diseases to make a diagnosis, says Michael Hung, O.D., of Omni Eye Services in Atlanta. The lid laxity is the key. Have the patient look down and put pressure on the upper lid. FES patients will have a rubbery tarsal and spontaneous lid eversion.
Dr. Pohl suspects this patient experienced nocturnal lagophthalmos, causing the tarsal conjunctiva to rub against the adjacent bedding, exposing the cornea. Scientists originally thought that FES was more prevalent in obese men, but recent studies have shown that a genetic collagen and/or elastin abnormality and not obesity is the culprit.2
A decrease in tarsal elastin causes collagenous connective tissue to degenerate in these patients, causing eyelid eversion during sleep, with subsequent drying and mechanical irritation.3,4
Loss of eyelid globe-contact in our patient.
Q. Whats the best management plan for patients with floppy lid syndrome?
A. Patient education and preventing recurrence should be first in your immediate management plan. Recommend to the patient that he sleep on his back or opposite side to avoid further exposure, Dr. Pohl says.
Floppy eyelid syndrome is mechanical in nature, so you wont be able to eliminate the cause, Dr. Hung says. Youll only be able to deal with the inflammatory res-ponse component. Topical treatment includes preservative-free artificial tears to address irritation and a mild steroid such as Alrex (loteprednol, Bausch & Lomb) for patients with more severe conjunctivitis or keratitis. Dr. Pohl also suggests an antibiotic if signs of infection are present.
Using tape or an eyeshield to keep the lids closed while the patient sleeps may help prevent lid eversion and help keep the eye from becoming dry. Moisture chambers are designed for post-LASIK patients to induce moisture into the ocular environment, prevent desiccation and exposure keratopathy. These may be beneficial as an off-label treatment for these patients, Dr. Hung says.
FES patients are often sensitive to their environmental conditions. Advise patients to use a humidifier at home and to stay away from heating and air conditioning vents that could cause further exposure, Dr. Hung says. Patients with sleep apnea syndrome (SAS) are also predisposed to FES. In one Swiss study, 61% of FES patients were diagnosed with SAS.5 Patients with FES should be referred to a pulmonologist for SAS testing due to the high morbidity rate of the disease.6
If palliative treatments fail, a horizontal shortening procedure or eyelid wedge resection may be indicated. This also represents an ideal comanagement opportunity with an oculoplastic surgeon, Dr. Pohl says.
1. Dufek MA, Shechtman DL. Floppy eyelid syndrome:adiagnostic dilemma. J Am Optom Assoc 1999 Jul;70(7):450-4.
2. Netland PA, Sugrue SP, Albert DM, Shore JW. Histopath-ologic features of the floppy eyelid syndrome. Involvement of tarsal elastin. Ophthalmology 1994 Jan;101(1):174-8.
3. Mazal Z. The floppy eyelid syndrome. Cesk Oftalmol 1990 Nov;46(6):434-8.
4. Lee WJ, Kim JC, Shyn KH. Clinical evaluation of corneal diseases associated with floppy eyelid syndrome. Korean J Ophthalmol 1996 Dec;10(2):116-21.
5. Mojon DS, Goldblum D, Fleischhauer J, et al. Eyelid, conjunctival, and corneal findings in sleep apnea syndrome. Ophthalmology 1999 June;106(6):1182-5.
6. McNab AA. Floppy eyelid syndrome and obstructive sleep apnea. Ophthal Plast Reconstr Surg 1997 Jun;13(2):98-114.

