 |
Color vision testing is a staple to screen for congenital color vision defects; it’s also helpful to detect or monitor disease progression in patients with various neuro-ophthalmic conditions. Often, a color vision test can be a cost-effective and readily accessible technique to identify and monitor certain ocular diseases and enable earlier intervention.
The Options
Color vision tests are comprised of two categories:1
Pseudoisochromatic plates, such as the Ishihara and Hardy-Rand-Rittler tests, distinguish between the different types of dichromatism, such as protanopia and deuteranopia (red-green), or tritanopia (blue-yellow).1,2 Widely available, inexpensive and easy to perform and interpret, these are the most commonly used color tests in clinical practice.1,2
When clinicians use color plate testing, they should record not only the number of plates identified but also the speed in which the patient identifies the plates.4
Color arrangement tests, such as the Farnworth-Munsell 100 hue test, involve patients categorizing colored objects with a fixed chroma in sequential order.1 While providing more detail and a higher sensitivity, they are more time-consuming.1,2
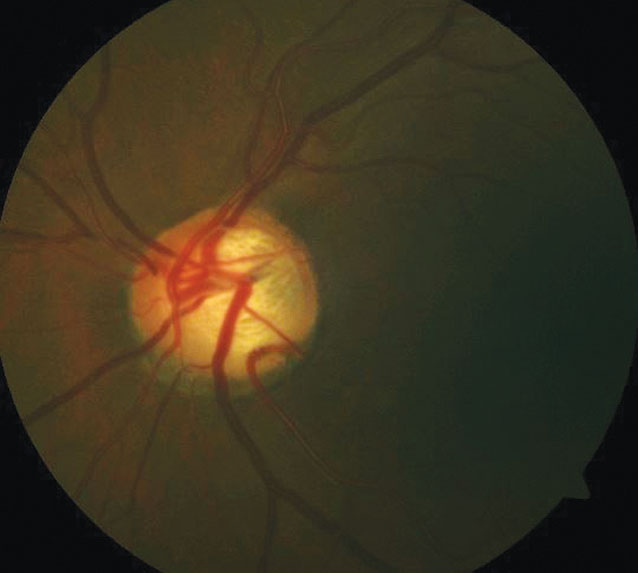 |
| POAG may create blue-yellow color vision defects. |
The Nerve
Because color discrimination is mediated through cones that absorb light stimuli and transmit that sensory information to the optic tract and, ultimately, the occipital cortex, the optic nerve is sensitive to changes in color.3 Thus, defects in the optic nerve or photoreceptors can alter color perception, leading to dyschromatopsia. Optic nerve disease will affect color vision more so than any other disease.2
In a study evaluating color vision defects in the presence of optic neuropathies, macular diseases, media opacities and amblyopia, preserved visual acuity (VA) with loss of color vision was strongly correlated with optic neuropathy. While profound vision loss in macular disease and amblyopia also leads to reduced color vision, this is likely due to the poor VA and trouble identifying the color plates.2
In patients with primary open-angle glaucoma (POAG), color vision defects are more likely to affect the blue-yellow spectrum. Often, color deficits will present prior to a visual field defect. As a result, color testing may be beneficial in monitoring ocular hypertension patients and their probability of developing glaucoma. Because the color deficiency progresses as glaucomatous damage does, it can also offer a quantifiable measurement of retinal ganglion cell damage.3
A New Use
Color vision testing may also be an inexpensive alternative to optical coherence tomography (OCT) for diabetic macular edema. Studies using the Farnworth-Munsell 100 hue test uncovered blue-yellow defects in diabetic patients, and researchers have developed a computerized color vision test that shows promise. It reveals a correlation between the degree of color vision abnormality and macular thickness volume on OCT.5
Color vision screening can offer great clinical insight on disease identification and progression. While it is sensitive to optic neuropathies, it may also show future promise in the detection of macular diseases. As such, optometrists should not overlook this valuable tool.
1. Zhao J, Davé SB, Wang J, et al. Clinical color vision testing and correlation with visual function. Am J Ophthalmol. 2015;3(140):547-52. 2. Almog Y, Nemet Y. The correlation between visual acuity and color vision as an indicator of the cause of vision loss. Am J Ophthalmol. 2010;149:1000-4. 3. Papaconstantinou D, Georgalas I, Kalantzis G, et al. Acquired color vision and visual field defects in patients with ocular hypertension and early glaucoma. Clin Ophthalmol. 2009;3:251-7. 4. Behbehani R. Clinical approach to optic neuropathies. Clin Ophthalmol. 2007:1(3):233-46. 5. Shin YJ, Park KH, Hwang JM, et al. A novel color vision test for detection of diabetic macular edema. Invest Ophthalmol Vis Sci. 2014;55:25-32. |

