A 79-year-old Hispanic female presented with blurred vision and a visual “gray spot” in her left eye. She reported that the spot appeared fairly suddenly in her central vision, but she believed that it would improve. When it didn’t, she decided to seek a medical opinion.
 |
|
Her ocular history was remarkable for cataract surgery OU about 10 years earlier. She noted excellent vision in both eyes until approximately three months ago. She reported no visual problems OD.
Her medical history was significant for hypertension and a heart condition, which were controlled with digoxin, Crestor (rosuvastatin calcium, AstraZeneca), nifedipine and hydrochlorothiazide.
On examination, her best-corrected visual acuity measured 20/20 OD and 20/60 OS. Extraocular motility testing was normal. Confrontation visual fields were full to careful finger counting OU. Her pupils were equally round and reactive, with no evidence of afferent defect OU. Amsler grid testing of the right eye was normal; however, the left eye exhibited central metamorphopsia. Her anterior segment exam revealed well-centered posterior segment IOLs OU.
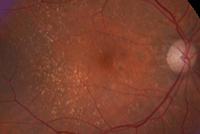
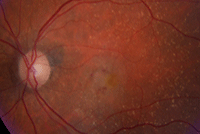
Dilated fundus exam showed a small cup with good rim coloration and perfusion OU. We noted obvious macular pathologies in both eyes (figures 1 and 2). The left eye, in particular, showed elevation and other significant changes. Additionally, we obtained a spectral-domain optical coherence tomography (SD-OCT) scan OS (figure 3).
Take the Retina Quiz
1. What do the focal white deposits in both maculae represent?
a. Drusen.
b. Exudate.
c. Retinal crystals.
d. Dalen-Fuchs nodules.
 |
| |
|
1, 2. Fundus examination of our patient (OD left, OS right). What changes do you note in her left eye?
| ||
2. What does the area of elevation seen on SD-OCT represent?
a. Choroidal mass.
b. Hemorrhagic pigment epithelial detachment (PED).
c. Serous PED.
d. Large choroidal neovascularization (CNV).
3. What is the likely diagnosis?
a. Choroidal hemangioma.
b. Wet age-related macular degeneration (AMD).
c. Central serous chorioretinopathy.
d. Retinal angiomatous proliferation.
4. How should she be managed?
a. Observation.
b. Thermal laser treatment.
c. Photodynamic therapy (PDT).
d. Anti-VEGF injection.
5. What is the likely long-term management protocol for this case?
a. Continued observation.
b. Monthly anti-VEGF injections.
c. Anti-VEGF injections, as needed.
d. PDT and laser, as needed.
For answers, see below.
Discussion
The small focal deposits scattered throughout both posterior poles represent drusen. Based on these changes alone, our patient has macular degeneration. Additionally, she has converted from dry to wet AMD in her left eye.
There is an obvious subretinal hemorrhage surrounding a focal elevation in the left fovea that appeared to be a retinal pigment epithelial detachment. Considering the lesion’s central location and three-month duration, her visual acuity actually is quite good.
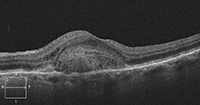
Her SD-OCT scan proved very interesting. There is an obvious focal area of elevation involving the macula. This appears to originate from a highly reflective, dome-shaped mass located just above the retinal pigment epithelium (RPE). The initial clinical impression was that the elevation represented a PED. But, based on the SD-OCT scan, the RPE is fairly intact––so it doesn’t appear to be a PED.
Instead, the reflective area likely represents a vascular meshwork of choroidal neovascularization that is growing above (or anterior to) the RPE. The elliptical zone (formerly known as the photoreceptor integrity line or the inner segment/outer segment junction) seems to be fairly intact, except near the lesion’s apex. This explains why her vision isn’t significantly compromised OS.
|
|
|
3. A spectral-domain optical coherence tomography scan through the macula of our patient's left eye.
|
The treatment for wet AMD has evolved considerably over the past decade. Intravitreal anti-VEGF therapy has revolutionized the management of neovascular AMD. Available medications include ranibizumab, bevacizumab and aflibercept. All three agents demonstrate tremendous efficacy in treating CNV; however, specific treatment selection usually is dictated by physician preference and/or economic considerations (bevacizumab is profoundly less expensive than either ranibizumab or aflibercept).
The majority of clinical trials have shown that monthly injections are slightly more effective than PRN treatment, although the clinical differences between a monthly and PRN injection schedule are not statistically significant. The primary advantage of PRN therapy is reduced treatment frequency during the first year (i.e., roughly six or seven injections vs. 10 or 11 injections).1 Further, PRN treatment yields clear economic advantages and improved patient tolerance.
Treat and extend (TREX) management is now employed by approximately 77% of retinal specialists in the US.2 With this protocol, patients are treated during each visit, regardless of disease activity. If there is no sign of exudation, the treatment intervals are extended gradually by one to two weeks. When there are signs of disease recurrence, the intervals are shortened. The shortest interval between injections is four weeks, and the longest interval is up to 12 weeks.
The fundamental goal of TREX is to maintain an exudation-free macula using the fewest injections possible.2,3 Ideally, this approach will reduce treatment costs to insurance companies, health care providers and patients.
To date, the Lucentis Compared to Avastin Study (LUCAS) is the largest prospective trial to evaluate the clinical efficacy of the TREX protocol.3 The researchers randomized 420 Norwegian patients with wet AMD to receive either ranibizumab or bevacizumab injections for up to one year. Subjects in the ranibizumab group received an average of 8.0 injections compared to 8.8 injections in the bevacizumab group.3 At one year, both agents performed equally well, with patients in the ranibizumab group gaining 8.2 ETDRS letters vs. 8.0 letters in the bevacizumab group.3 Two other prospective clinical trials evaluating the TREX approach are also underway in the US.4,5
Our patient received an intravitreal bevacizumab injection and was instructed to return in four weeks. At the four-week follow-up, she still exhibited considerable exudation and macular edema, so we ordered a second injection. She was then scheduled to return in another four weeks.
If the exudation has resolved, she will receive third injection and the follow-up period will be extended to six weeks.
1. Martin DF, Maguire MG, Ying GS, et al. Ranibizumab and bevacizumab for neovascular age-related macular degeneration. N Engl J Med. 2011 May 19;364(20):1897-908.
2. Wykoff CC. Treat and Extend Management of Neovascular AMD: What Data Do We Have? AMD Update. Available at:
www.visioncareprofessional.com/emails/amdupdate/index.asp?issue=74. Accessed October 21, 2014.
3. Berg K. LUCAS (Lucentis Compared to Avastin Study). ClinicalTrials.gov identifier: NCT01127360. Available at:
http://clinicaltrials.gov/ct2/show/NCT01127360?term=LUCAS&rank=4. Accessed October 20, 2014.
4. Regillo C. Repeated Eye Injections of Aflibercept for Treatment of Wet Age Related Macular Degeneration (ATLAS). ClinicalTrials.gov identifier: NCT01773954. Available at:
http://clinicaltrials.gov/ct2/show/NCT01773954?term=Regillo&rank=1. Accessed October 20, 2014.
5. Wykoff CC. Treat and Extend Treatment With 0.5mg Ranibizumab vs Monthly Treatment With 0.5mg Ranibizumab (T-REX). ClinicalTrials.gov identifier: NCT01748292. Available at:
http://clinicaltrials.gov/ct2/show/NCT01748292? term=wykoff&rank=2. Accessed October 20. 2014.

