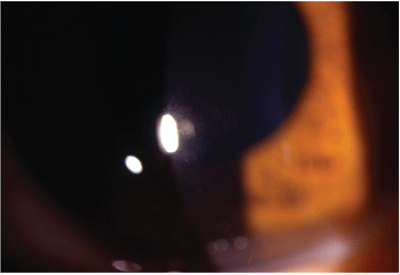
Vogts striae is one sign of keratoconus. The etiology of keratoconus remains unclear.
Q: There seems to be much new information about the relationship between aquaporin-5 deficiencies and keratoconus. What are aquaporins, and are they aberrant in any other ocular condition?
A: Aquaporin-5 (AQP5) is one of a large family of proteins on cell membranes. These proteins form pores to selectively usher water molecules in and out of the cell. Single file, H2O molecules make their way in and out of the cell through these openings. A cell membranes permeability to water is dependant on the presence of such pores.
The family of proteins to which aquaporins belong sometimes goes by the name integral membrane proteins (IMP) or major intrinsic proteins (MIP). Or, they are simply known as water channels. There are 13 known aquaporins, many of which are found in the kidneys.
Defects in aquaporin genes can cause disease. In humans, mutations in the aquaporin-2 gene lead to hereditary nephrogenic diabetes insipidus. In mice, mutations in the aquaporin-0 gene lead to congenital cataracts.
Aquaporin-5 is of particular interest in eye care because it is expressed in the secretory glands, including the lacrimal glands. AQP5 is also expressed in the cornea with AQP1. A study published in 2001 found a selective defect in AQP5 membrane trafficking in the lacrimal glands of patients who have Sjgrens syndrome, raising speculation that the absence of this protein may contribute to dry eye in these patients.1
Of further interest: a 2005 paper in which researchers found that keratoconus patients showed virtually no AQP5 transcripts.2 For years, researchers have believed that heredity plays some role in keratoconus, but this paper provided clear evidence of an associated genetic defect. Although the deletion of AQP5 induces corneal swelling in mice, this type of progression seems to be at odds with the stromal thinning that occurs in keratoconus. Even so, the authors of the study speculate that this disparity may be due to differences between the rodent and human eye. They also speculate that other genetic and environmental factors besides the absence of AQP5 likely play a role in the pathogenesis of keratoconus.
Q: What is the clinical significance of this AQP5 dysfunction?
A: The short answer: No one really knows. Despite advances, such as the AQP5 studies mentioned above, the etiology of keratoconus remains an unclear picture composed of disparate parts. Current breakthroughs are more beneficial to future research than to everyday practice, clinicians say.
I had a keratoconus patient a few years ago who wanted me to examine his child every three months for evidence of the disease, says Karla Zadnik, O.D., Ph.D, of the Ohio State University College of Optometry. Its not like that. We are not at that level yet.
Besides heredity, chronic inflammation appears to play a role, says Dr. Zadnik, who spearheaded the Collaborative Longitudinal Evaluation of Keratoconus (CLEK) study. The CLEK study evaluated a large cohort of patients over several years.
One surprising finding of the CLEK Study: Many subjects reported significant ocular pain, even those who did not wear contact lenses. Some report of pain kind of lends credence to a chronic inflammation etiology, Dr. Zadnik says. But, it could mean a lot of other things, too.
Bolstering the case for inflammation, a 2005 paper reported that the tear fluid of keratoconus patients contained inflammatory mediators, such as interleukin-6, tumor necrosis factor-alpha (TNF-a) and matrix mettaloproteinase-9 (MMP-9).3 Evidence linking the disease to Sjgrens-related dry eye and ocular inflammation has led some to wonder if keratoconus patients might benefit from an immunosuppressive agent, such as Restasis (cyclosporine A, Allergan).
Also, studies have shown an association between the disease and a history of eye rubbing.4,5 Finally, CLEK researchers found that 53% of the patients had a history of allergy.6 How all these elements contribute to the pathology of keratoconus, however, remains uncertain.
We are in a time when we are beginning to integrate all these disparate pieces of information, says Roslyn, N.Y., optometrist Arthur B. Epstein. There are various unified theories, but none are backed by scientific evidence.
His belief, based on years of treating keratoconus patients, revolves around the mechanics of blinking. He points out that many patients continue to progress even after they discontinue chronic eye rubbing.
Further, keratoconus may progress more slowly in patients who wear well-fit contact lenses, yet patients with poor lens fits and those who do not wear contacts usually degenerate rapidly.7 I think the essence of this equation is force distribution, Dr. Epstein says. A lifetime of blinking, he suggests, may be far more traumatic to the cornea than we realize, unleashing shearing forces that vary from patient to patient.
Genetically predisposed patients who also rub their eyes may be setting off a kind of mechanically induced autoimmune disease that attacks the eye from within, Dr. Epstein adds. Contact lenses forestall this process by distributing the shearing force of the blink over a wider area, according to his theory. It remains only a theory, but he plans to explore these ideas by studying the mechanics of blinking via high-speed radiology.
One tangible advance the near future may bring is a genetic test designed to identify patients predisposed to developing keratoconus. The lead investigator of the study linking the disease to the absence of AQP5, Yaron S. Rabinowitz, M.D., chairman of the division of ophthalmology research at Cedars-Sinai Medical Center in Los Angeles, is working on a test prototype, and preliminary data looks promising.
1. Tsubota K, Hirai S, King LS, et al. Defective cellular trafficking of lacrimal gland aquaporin-5 in Sjgrens syndrome. Lancet 2001 Mar 3;357(9257):688-9.
2. Rabinowitz YS, Dong L, Wistow G. Gene expression profile studies of human keratoconus cornea for NEIBank: a novel cornea-expressed gene and the absence of transcripts for aquaporin 5. Invest Ophthalmol Vis Sci 2005 Apr;46(4):1239-46.
3. Lema I, Duran JA. Inflammatory molecules in the tears of patients with keratoconus. Ophthalmology 2005 Apr;112(4):654-9.
4. Krachmer JH. Eye rubbing can cause keratoconus. Cornea 2004 Aug;23(6):539-40.
5. Jafri B, Lichter H, Stulting RD. Asymmetric keratoconus attributed to eye rubbing. Cornea 2004 Aug;23(6):560-4.
6. Zadnik K, Barr JT, Edrington TB, et al. Baseline findings in the Collaborative Longitudinal Evaluation of Keratoconus (CLEK) Study. Invest Ophthalmol Vis Sci 1998 Dec;39(13):2537-46.
7. Gorskova EN, Sevost"ianov EN. Contact correction: method for arresting the progress of keratoconus. Vestn Oftalmol 1998 Jan-Feb;114(1):48-50.

