
|
A 63-year-old Argentinean woman presented with a chief complaint of burning eyes (O.D. > O.S.), which had persisted for six months. Her systemic history was remarkable for hypertension, for which she was compliant and properly medicated. Presently, the patient also had a common cold. Her ocular history was unremarkable, and she reported no known allergies.
Diagnostic Data
Her best-corrected visual acuity measured 20/70 O.U. at distance and near. Extraocular muscles and pupils were normal. Her intraocular pressure measured 14mm Hg O.U. The dilated fundus examination was normal. The significant anterior segment findings are illustrated in the photograph.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What’s the likely prognosis?
Discussion
Additional tests might include sodium fluorescein staining to rule out compromised corneal integrity and corneal sensitivity testing.
The diagnosis in this case is bilateral, visually significant pterygia that require excision. Pterygia are wedge-shaped fibrovascular growths that extend onto the cornea. They are frequently—but not always—the product of chronic pathophysiological sequelae, introduced by pingueculae.1-5 Both lesions may become vascularized and inflamed, and typically are associated with corneal punctate epitheliopathy and dellen (corneal thinning secondary to dryness).1-5 When a pinguecula becomes acutely inflamed, vascularized, red, irritated and highly symptomatic, it is referred to as pingueculitis.3-6
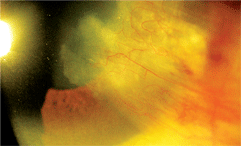
An anterior segment image of our 63-year-old patient’s right eye. What do you notice?
Pinguecula formation typically is seen in the older population and is considered to be a conjunctival degenerative process initiated by exposure to noxious environmental stimuli and UV light.2-5 The initial lesion is thought to result from the chronic action of solar radiation, which induces an alteration of the collagen and elastic tissues of the conjunctival stroma leading to elastotic degeneration and deposition of abnormal elastic fibers in the conjunctival substantia propria.1,2,5 Once a pinguecular elevation is formed––depending on its size––the tear film may become thin and discontinuous in that zone, producing a bed of dryness.1 When the lesion is sufficiently affected by the processes of inflammation, vascular dilation allows histamine, seratonin, bradykinin and prostaglandins to be released, which produces the acute irratative symptoms that characterize pingueculitis. In severe cases, the conjunctival surface becomes sufficiently dry to cause microulceration of the conjunctival epithelium. When this occurs, the eye enters into a protective mode in an attempt to cover the erosion. This protective process leads to pterygium formation.1 The classic fibrovascular, wing-shaped encroachment of the conjunctiva onto the cornea demonstrates prevalence rates that range from 0.7% to 31% among different populations. Additionally, disease prevalence is highly influenced by age, race and exposure to solar radiation.7 The accepted pathophysiology relates to ultraviolet light-induced damage to the limbal stem cell barrier with subsequent conjunctivalisation of the cornea.
Management of pinguecula chiefly is predicated on symptomatology. Patients who have occupations or hobbies that increase the risk of pinguecula formation should be counseled on the preventative benefits of sunwear, UV blocking coatings or goggles that limit dust exposure.3 In cases of mild pingueculitis—where symptoms are mild or dellen are present—ocular lubricating drops such as Tears Naturale II (Alcon), Cellufresh (Allergan) or Celluvisc (Allergan) and ointments such as Refresh P.M (Allergan ) or Lacrilube (Akorn) are indicated. When symptoms and inflammation become more significant, q2h to q.i.d. treatments of topical steroids such as 0.12% prednisolone acetate suspension (Pred Mild, Allergan), 0.12% prednisolone sodium phosphate solution (Inflamase Mild, CooperVision), 1% prednisolone acetate suspension (Pred Forte, Allergan), 1% prednisolone sodium phosphate solution (Inflamase Forte, CooperVision), 0.25% fluorometholone (Flarex, Alcon) and 1% rimexolone acetate (Vexol, Alcon) are acceptable options.2,3,5
A recently published report recognized that 0.1% indomethacin solution has a beneficial effect in cases of inflamed pinguecula or ptertgium; however, a commercial topical preparation is not currently available.6 In severe cases, where pterygia are present and interfering with vision, contact lens wear or corneal wetting, surgical resection is a possible treatment option.2,3
Indication for surgery includes visual impairment, cosmetic disfigurement, motility restriction, recurrent inflammation and interference with contact lens wear.7 In this case, we placed the patient on topical ocular lubricants and referred her to an oculoplactics specialist for bilateral pterigium resection. She was apprehensive about the procedure and was lost to follow-up. In one recent study using supero-temporal free conjunctivo-limbal autograft transplantation in the surgical management of pterygium, the success rate was upwards of 72%. Other researchers have investigated different methods of creating interface with the graft tissue. In one study, the rate of recurrence and pre- and postoperative complications were evaluated in pterygium surgery using fibrin glue to attach the conjunctival autograft.8
In a 20-month period, 35 patients were operated on for pterygium using a conjunctival autograft, of which seven patients had surgery (20%) for recurrent pterygium.8 In each case, the autograft was glued with Tissucol Duo 500, a human tissue glue. Follow-up was at least one year. The mean age of the patient population was 50.4 years (range of 23 to 80 years) and included 18 women and 17 men. The surgical success rate was 97.1%.8
1. Archila EA, Arenas MC. Etiopathology of pinguecula and pterigium. Cornea. 1995 Sep;14(5):543-4.
2. Wallace W. Diseases of the Conjunctiva. In: Bartlett JD, Jaanus SD. Clinical Ocular Pharmacology. Boston: Butterworth Heinmann Publishers; 1984:583-648.
3. Cullom RD, Chang B. Cornea: Pterygium/Pingueculum. In: Cullom RD, Chang B. The Wills Eye Manual: Office and Emergency Room Diagnosis and Treatment of Eye Disease. Philadelphia: J.B. Lippincott Co.; 1994:65-7.
4. Bergmanson JP, Söderberg PG. The significance of ultraviolet radiation for eye diseases. A review with comments on the efficacy of UV-blocking contact lenses. Ophthalmic Physiol Opt. 1995 Mar;15(2):83-91.
5. Cohen EJ, Rapuano CJ, Laibson PR. External Diseases. In: Tasman W, Jaeger EA. The Wills Eye Atlas of Clinical Ophthalmology. Philadelphia: J.B. Lippincott Co.; 1996:1-85.
6. Frucht-Pery J, Solomon A, Siganos CS, et al. Treatment of inflamed pterygium and pinguecula with topical indomethacin 0.1% solution. Cornea. 1997 Jan;16(1):42-7.
7. Sadiq MN, Arif AS, Jaffar S, et al. Use of supero-temporal free conjunctivo-limbal autograft in the surgical management of pterygium: our technique and results. J Ayub Med Coll Abbottabad. 2009;21(4):121-4.
8. Nieuwendaal CP, van der Meulen IJ, Mourits M, et al. Long-term follow-up of pterygium surgery using a conjunctival autograft and Tissucol. Cornea. 2011;30(1):34-6.

