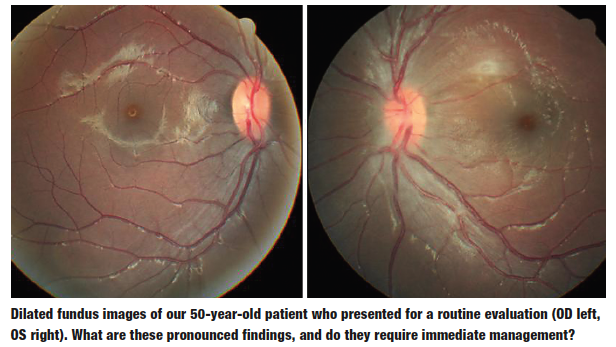
 History
History
A 50-year-old white female presented for a routine eye examination. During the work-up, she raised several questions regarding a “longstanding visual issue” in both eyes. The patient informed us that a previous eye care provider documented evidence of bilateral scarring secondary to an ocular infection earlier in her life. Nevertheless, the patient reported no visual complaints. Her systemic history was unremarkable, and she reported no known allergies of any kind.
Diagnostic Data
Following refraction, her best-corrected visual acuity measured 20/25 OU at distance and near. External examination was normal, with no evidence of afferent pupillary defect. The anterior segment structures were normal, and her intraocular pressure measured 15mm Hg OU. The dilated fundus examination and correlating visual fields are illustrated in the photograph.
Your Diagnosis
How would you approach this case? Does the patient require any additional tests? What is your diagnosis? How would you manage this patient? What is the likely prognosis?
Discussion
Additional testing included photodocumentation and automated perimetry. A more detailed patient history revealed that the patient both lives and works on a farm with livestock. The diagnosis in this case is retinal-choroidal scarring secondary to presumed toxoplamosis infection. Toxoplasma gondii is a protozoal parasite.1-10 It is among the most resilient protozoan parasites. Specifically, T. gondii has an uncanny ability to manipulate the immune system of its host.9
The disease was initially discovered and described in 1908. At that time, the parasite was believed to be carried exclusively by rodents.7 T. gondii may be transmitted from the mother to the fetus through the placenta, causing congenital infection. Alternatively, it may be acquired later in life through an exposure to an environment harboring the organism (i.e., soil that is contaminated by fecal matter from several species of birds and mammals).1-9
It is important to note that felines seem to be the parasite’s natural host.4-6 Raw or undercooked lamb, chicken or beef also may harbor T. gondii.1-6 According to one study, nearly one-third of humans worldwide have been exposed to this parasite via contact with infected pigs, bears, felids, fox, raccoons and skunks.7 Toxoplasmic retinochoroiditis is a phenomenon of the posterior pole. The lesions can be solitary, multiple or satellite.3-6
Active lesions present as grey-white foci of retinal necrosis with adjacent deep choroiditis, retinal vasculitis (vessel sheathing), intraretinal hemorrhage and varying amounts of vitritis.3-6 The condition is among the most common causes of posterior uveitis in both immunocompetent and immunocompromised individuals.3,5,6
Active disease in teenagers and adults frequently causes decreased vision. Patients often report the presence of floaters, as well as photophobia, pain and hyperemia.3-5 Granulomatous anterior uveitis is a common finding, with mutton-fat keratic precipitates, fibrin, cells and flare, iris nodules, and posterior synechiae.1-8 Scar formation occurs upon lesion inactivity, which is signified by variable pigmentary hyperplasia.1-6 Old retinal scars from previous episodes connote significant retinal destruction.3-6 As in any case of retinal and subretinal disruption, cystoid macular edema may develop. In the most severe cases, patients will exhibit choroidal neovascularization.4-6 Further, affected individuals may experience disc edema. (When retinal swelling and disc edema concurrently present, the condition is termed “neuroretinitis.”4-6)
The laboratory diagnosis of toxoplasmosis is based on antibody detection. Appropriate testing includes T. gondii DNA via polymerase chain reaction, antitoxoplasma antibody test, Sabin-Feldman methylene blue dye test and compliment fixation test.3-8 Toxoplasmosis therapy includes various combinations of specific oral and topical medications, including pirimetamine, sulfadiazine, clindamycin, trimethoprime-sulphamethoxazol, spiramycin, azithromycin, atovaquone, tetracycline and minocycline. Because the combinations require systemic monitoring, a retinology referral is recommended during the systemic treatment process. Concomitant uveitis management includes atropine BID for severe reactions and cyclopentolate BID to TID for lesser reactions, as well as topical steroids QID to Q2H.3-8 The prognosis of ocular toxoplasmosis generally is good in immunocompetent individuals, as long as the central macula is not directly involved.3-8 However, because the infection and inflammation involve both the choroid and retina, all associated lesions have the potential to induce localized neovascularization.1-10
Because there was no active retinal or subretinal inflammation, the patient required no additional topical or oral treatment.
1. Sukthana Y. Toxoplasmosis: beyond animals to humans. Trends Parasitol. 2006;22(3):137-42. 2. Rorman E, Zamir CS, Rilkis I, et al. Congenital toxoplasmosis--prenatal aspects of Toxoplasma gondii infection. Reprod Toxicol. 2006;21(4):458-72. 3. Bonfioli AA, Orefice F. Toxoplasmosis. Semin Ophthalmol. 2005;20(3):129-41. 4. Levinson RD, Rikkers SM. Ocular toxoplasmosis. In: Yanoff M, Duker JS. Ophthalmology, 2nd Ed. Philadelphia, Mosby; 2004:1167-71. 5. Alexander LJ. Exudative and nonexudative macular disorders. In: Alexander LJ. Primary Care of The Posterior Segment. Norwalk, Conn.: Appleton and Lange; 1994:277-344. 6. Benson WE, Tasman W. Retina: Toxoplasmosis. In: Rhee DJ, Pyfer MF. The Wills Eye Manual, 3rd Ed. Philadelphia: Lippincott Williams and Wilkins; 1999:406-9. 7. Hill DE, Chirukandoth S, Dubey JP. Biology and epidemiology of Toxoplasma gondii in man and animals. Anim Health Res Rev. 2005;6(1):41-61. 8. Jaeger EA, Benson WE, Tasman W, et al. Uveitis: Anterior uveitis. In: Rhee DJ, Pyfer MF. The Wills Eye Manual, 3rd Ed. Philadelphia: Lippincott Williams and Wilkins; 1999:393-400. 9. Saeij JP, Boyle JP, Boothroyd JC. Differences among the three major strains of Toxoplasma gondii and their specific interactions with the infected host. Trends Parasitol. 2005 Oct;21(10):476-81. 10. Mauget-Faysse M, Mimoun G, Ruiz-Moreno JM, et al. Verteporfin photodynamic therapy for choroidal neovascularization associated with toxoplasmic retinochoroiditis. Retina. 2006 Apr;26(4):396-403.

