 |
When Bev, a 41-year-old white female at the time, walked into my (JS) exam room decades ago, it was a trip down memory lane. My memories of her dated back to the year I graduated from high school and when I escorted her to her senior prom.
Bev wasn’t visiting to rehash our past romance but to obtain a second opinion about her right eye and to test my memory. Bev began experiencing occasional blurred vision in her right eye, and when she looked in a mirror, she observed that her right eye looked different from her left. Bev was now quite concerned and decided to be examined by a local ophthalmologist. The MD detected both an unusual-shaped pupil and iris structure in her right eye only but a normal exam otherwise. He reassured Bev that she wasn’t going blind, had 20/20 visual acuity in each eye and suggested that the findings may have been congenital and perhaps slowly progressive but less than obvious because of Bev’s dark brown eyes.
As recommended by the ophthalmologist, Bev decided to obtain a second opinion from her old high school prom date. Bev asked me, “When you looked into my eyes the night of the senior prom, did I look like a cat?” I did not recall anything unusual about Bev’s eyes the night of prom, but perhaps we both had too much scotch.
 |
|
ICE in this patient. Click image to enlarge. |
Testing
Bev was quite cooperative with numerous imaging procedures and, as requested, brought in several dozen pictures of her face over the years. I performed what we facetiously term a “FAT-scan”—or family album tomography—and could not detect any previous evidence of the cat’s eye pupil in her right eye. Hence, the condition appeared to be acquired and unilateral.
Bev was in good health, had no history of trauma and had no family history of eye problems. Uncorrected VA was 20/20 in each eye, and IOPs were 16mm Hg OD and 17mm Hg OS. A slit lamp exam revealed a vertical pupil in the right eye only, and both pupils constricted normally. The iris stroma was observed to be thickened in some areas but atrophic in others. The Swiss-cheese appearance of her right iris appeared to be due to parts of her iris literally wasting away, and other areas were thickened, likely resulting in traction. The resulting regrouping of the iris tissue produced a rather remarkable vertical pupil. Gonioscopy revealed an unusual trabecular meshwork and mild peripheral anterior synechiae (PAS) in the right eye only. A dilated fundus exam was unremarkable, and both optic nerve heads appeared normal with cup-to-disc ratios judged as 0.4 OU.
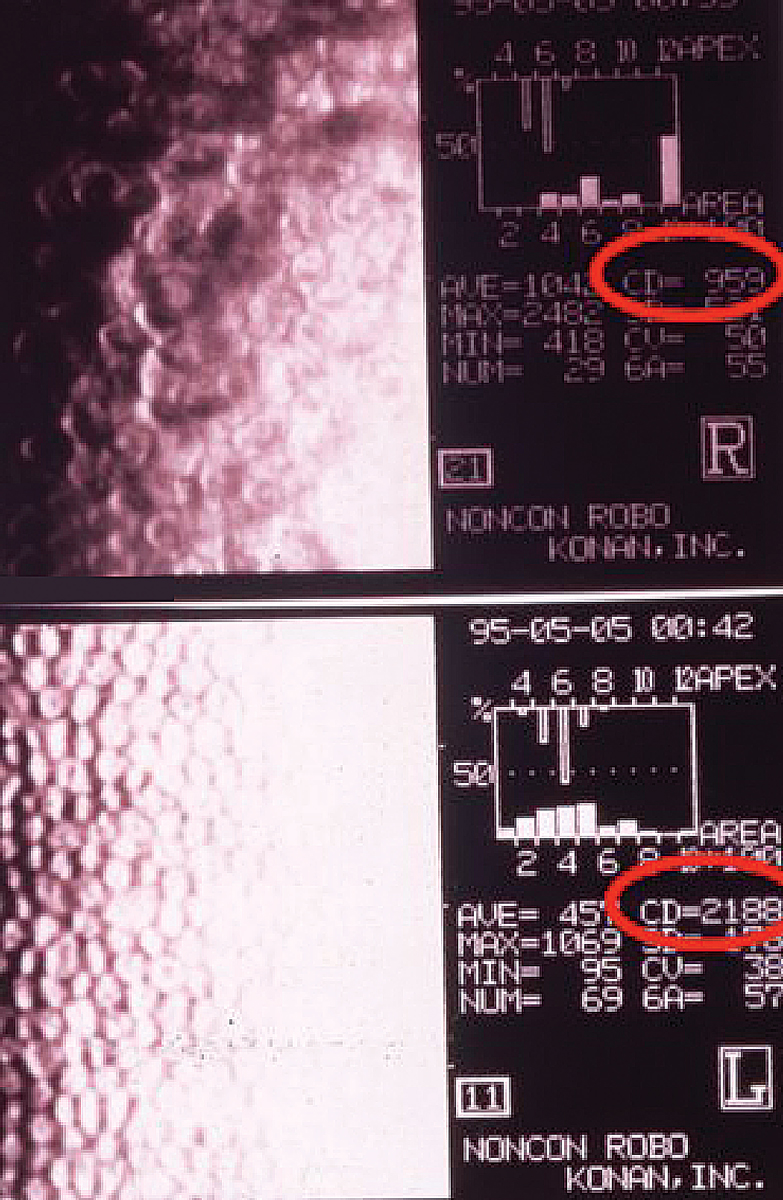
Threshold fields were obtained on the second visit and were normal OU. Imaging of the corneal endothelial cells with the Noncon Robo specular microscope by Konan revealed a remarkable difference between the two eyes. Of importance, the cell density in the right eye was 959mm2 in contrast to 2,188mm2 in the normal left eye.
Ultrasound biomicroscopy was later performed and revealed the iris in contact with the corneal endothelium in several clock hours. The PAS appeared to be extending above the normal position of Schwalbe’s line.
Diagnosis
Based on all of the above, the most probable diagnosis was iridocorneal endothelial (ICE) syndrome. This unique, most often unilateral ophthalmic disorder involves an irregular corneal endothelium that can lead to varying degrees of corneal edema, iris atrophy and secondary angle-closure glaucoma.1 The etiology is unknown, but herpes virus has been implicated in some cases.2
Follow-up
Over the next decade, Bev’s ICE progressed slowly. IOP in her right eye was occasionally elevated, and I treated her with various drops to lower it. I told Bev that she would likely need surgery in the future since she was slowly developing a form of angle-closure glaucoma in her right eye.
Bev eventually decided to be followed by a local ophthalmologist rather than making frequent trips into the big city. Her vision eventually dropped to 20/40 OD, and a local cataract surgeon recommended that she have cataract surgery in the right eye. Bev told the ophthalmologist all about the ICE syndrome that was diagnosed and treated over the past decade by her prom date optometrist and all the imaging that was performed and available. The cataract surgeon responded that it did not matter.
As recommended by the ophthalmologist, Bev had the routine procedure—with disastrous results. Her vision after cataract extraction was dramatically reduced and has not improved to this day. Corneal decompensation resulted, and steroid drops increased her IOPs.
Bev has undergone three penetrating keratoplasties and two glaucoma surgeries and still can barely see the big E on the Snellen chart at high contrast. Of even greater concern to Bev, her right eye remains cosmetically unacceptable and still appears abnormal even when viewed from across the room.
Bev decided to initiate a lawsuit against the surgeon and, as recommended by her attorney, against two ODs who examined Bev along the way, since she was not warned about the significant risk of cataract surgery in a patient with ICE.
 |
|
Note the difference in endothelial cell density between the right eye (top circle) and left (bottom circle). Click image to enlarge. |
You Be the Judge
Questions to consider:
- If the patient has an irregular corneal endothelium and iris atrophy, what secondary conditions may result?
- If this patient develops a cataract in the affected eye, what are the risks of cataract surgery?
- If the patient develops a cataract, should you refer for cataract surgery or for a cataract surgery consult?
- Is referring this or a similar case for cataract surgery malpractice?
- Is performing cataract surgery without appropriate discussion of risks and benefits malpractice?
Our Opinion
We find the surgeon culpable of malpractice for not explaining the risks and benefits of cataract surgery to a patient with only a mild to moderate cataract and with ICE. However, for the case to go forward, an ophthalmologist, preferably a cataract surgeon, will need to render the same opinion.
The surgeon recommended and performed cataract extraction on an eye with a previous diagnosis of ICE. By definition, Bev had a condition affecting her iris and her corneal endothelium. The surgeon should have known and recognized that, with ICE, there is a reduced number of endothelial cells and that increases the risk of corneal decompensation because of the trauma of cataract surgery.
It is important to note that corneal endothelial cells function to maintain corneal clarity by regulating corneal hydration. Corneal endothelial cells do not regenerate. A dramatic reduction in the number of corneal endothelial cells as documented by the endothelial cell device predicts corneal decompensation and bullous keratopathy because of the trauma of cataract surgery. Changes to corneal endothelial density are often considered the canary in the coal mine for distress to the cornea.
We recommend never referring atypical patients for cataract surgery but for a cataract surgery consult. This distinction may be critical in impending lawsuits. We recommend endothelial cell counts in all patients who may have a reduced cell density because of conditions such as Fuchs’ dystrophy and similar ones involving the endothelium.
Outcome of Malpractice Litigation
It is unclear how far the case went forward, but it is known that the case did not go to trial. I (JS) was not contacted for old records and was never deposed. However, we believe the case has substantial educational value.
| NOTE: This article is one of a series based on actual lawsuits in which the author served as an expert witness or rendered an expert opinion. These cases are factual, but some details have been altered to preserve confidentiality. The article represents the authors’ opinion of acceptable standards of care and do not give legal or medical advice. Laws, standards and the outcome of cases can vary from place to place. Others’ opinions may differ; we welcome yours. |
Dr. Sherman is a Distinguished Teaching Professor at the SUNY State College of Optometry and editor-in-chief of Retina Revealed at www.retinarevealed.com. During his 52 years at SUNY, Dr. Sherman has published about 750 various manuscripts. He has also served as an expert witness in 400 malpractice cases, approximately equally split between plaintiff and defendant. Dr. Sherman has received support for Retina Revealed from Carl Zeiss Meditec, MacuHealth and Konan.
Dr. Bass also holds the position of Distinguished Teaching Professor at the SUNY State College of Optometry. She is a Diplomate of the American Board of Optometry. She is an attending in the Retina Clinic of the University Eye Center and currently serves as the residency supervisor for the Residency in Ocular Disease at SUNY. She has no financial disclosures.
1. Oldham Gw, Wang C, Owaidhah OA, et al. Iridocorneal endothelial syndrome and secondary glaucoma. EyeWIki. eyewiki.aao.org/iridocorneal_endothelial_syndrome_and_secondary_glaucoma. August 18, 2022. Accessed February 9, 2023. 2. Walkden A, Au L. Iridocorneal endothelial syndrome: clinical perspectives. Clin Ophthalmol. 2018;12:657-64. |

