History
A 67-year-old black woman, who was admitted to the hospital for multiple systemic illnesses, presented to the eye clinic for a consult related to an unusual facial spasm that began 15 days earlier. She reported no local or generalized head pain, but noticed an increase in blinking and “eyelid twitching” approximately five to seven years ago.

Her systemic history was remarkable for arrhythmia and hypertension, for which she was properly medicated. She reported no known allergies.
Diagnostic Data
Her best-corrected visual acuity measured 20/20 O.U. at distance and near. Her external, corneal and internal ocular health was normal. She exhibited no evidence of afferent pupillary defect.
Her intraocular pressure measured 14mm Hg O.U. The dilated fundus examination was normal. The pertinent external examination finding is illustrated in the photograph.
Your Diagnosis
How would you approach this case? Does this patient require any additional tests? What is your diagnosis? How would you manage this patient? What’s the likely prognosis?
Additional Testing
Important questioning should have included a discussion about symptom severity, timing and frequency of the symptoms as well as any behavior or treatment that arrested the symptoms. Additional testing might have included evaluation and comparison of bilateral facial sensations, strength, and neuroimaging to rule out compression secondary to mass or aneurysm.
Discussion
The diagnosis in this case is essential blepharospasm of the ocular and facial muscles, or Meige’s syndrome. Patients with Meige’s syndrome frequently complain of photophobia and dry eye.1 An increased blinking frequency is often associated with these symptoms. The increased blinking rate becomes more frequent, forceful and sustained over period of two to seven years. The condition often results in intermittent functional blindness due to the inability to control these spasms and open the eyes.1-3 Factors that seem to exacerbate the disease include stressful situations (either at work or in social gatherings). As with other dystonias, patients are often able to employ sensory “tricks,” such as whistling, singing and the application of pressure to specific points on the face, to temporarily arrest spasms.1
The extension of essential blepharospasm to include adjacent focal oromandibular dystonia is referred to as Meige’s syndrome. As the disease progresses to involve the face, patients frequently complain of difficulty talking, eating and swallowing. In severe cases, pronounced bruxism occurs (locking of the jaw), resulting in problems with dentition and subsequent malnutrition.1-3
Other associated features may include decreased tear production, secondary adjacent dystonias (such as spastic dysphonia and torticollis or respiratory dysfunction) and anatomic changes (such as eyelid and brow ptosis, dermatochalasis, entropion and canthal tendon abnormalities).1,3
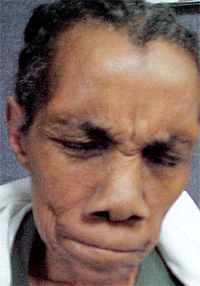
This 67-year-old patient presented with a significant facial spasm as well as increased blinking and eyelid twitching.
The anatomic site and the biochemical basis of essential blepharospasm is unknown. Most experts cite abnormalities in the basal ganglia or midbrain.1,3 Abnormal auditory brain stem response potentials have been noted in patients who have benign essential blepharospasm (BEB) and Meige’s syndrome.1 Further, abnormal levels of neurotransmitters have been detected in the midbrain and brain stem nuclei of patients with Meige’s syndrome. Additionally, researchers have isolated hyperactivities of the central dopaminergic and noradrenergic neurons as part of the pathophysiology of Meige syndrome.1,2
The treatment of choice for the initial management of BEB/Meige’s syndrome is botulinum toxin type A.1,4 This is one of seven antigenic-specific neurotoxins A, B, C1, D, E, F and G that are produced by the bacterium Clostridium botulinum. Botulinum neurotoxin, which reduces muscular contraction, blocks neuromuscular transmission by acting on peripheral cholinergic nerve endings to prevent acetylcholine release from presynaptic terminals.4 The onset of effect occurs within 24 to 72 hours, with a plateau at three to five days. Occasionally, however, the effect of the agent is delayed for as long as two to four weeks.1
The duration of denervation averages three months for BEB and slightly longer for hemifacial spasm.1 Frequently, the procerus and corrugator muscles are also involved and require injection. Other periorbital or facial sites may require treatment. Frequently, injections in the lower lid alone have a pronounced effect on spasms in the lower face, thus eliminating or decreasing the need for a second injection in that area.1,4 The recommended starting dose for botulinum toxin type A is 1.25 to 5 units per injection site. If a suboptimal response occurs, the clinician should double the dose.1,4
Major adverse reactions to botulinum toxin include ptosis, epiphora, keratitis, dry eye and diplopia. These effects are usually transient and resolve long before the beneficial effects of the drug are exhausted. A flu-like syndrome has been reported following botulinum toxin injections for blepharospasm; this effect generally is associated with higher doses.1 Studies also suggest the possibility of a transient increase in intraocular pressure and an abnormal emptying of the gallbladder, with secondary biliary colic as an additional side effect.1,4
We referred the patient to the neuro-ophthalmology department for evaluation and pharmacologic treatment.
1. Faucett D. Essential blepharospasm. In: Yanoff M, Duker JS. Philadelphia: Mosby; 1999: 7.10.1-4.
2. Yoshimura R, Kakihara S, Soya A, et al. Effect of clonazepam treatment on antipsychotic drug-induced Meige syndrome and changes in plasma levels of GABA, HVA, and MHPG during treatment. Psychiatry Clin Neurosci. 2001 Oct;55(5):543-6.
3. Kirton CA, Riopelle RJ. Meige syndrome secondary to basal ganglia injury : a potential cause of acute respiratory distress. Can J Neurol Sci. 2001 May;28(2):167-73.
4. Neuenschwander MC, Pribitkin EA, Sataloff RT. Botulinum toxin in otolaryngology: a review of its actions and opportunities for use. Ear Nose Throat J. 2000 Oct;79(10):788-9, 792, 794 passim.

